The evidence based dilemma of intraperitoneal drainage for pancreatic resection - a systematic review and meta-analysis
- PMID: 25291982
- PMCID: PMC4193685
- DOI: 10.1186/1471-2482-14-76
The evidence based dilemma of intraperitoneal drainage for pancreatic resection - a systematic review and meta-analysis
Abstract
Background: Routine placement of intraperitoneal drains has been shown to be ineffective or potentially harmful in various abdominal surgical procedures. Studies assessing risks and benefits of abdominal drains for pancreatic resections have demonstrated inconsistent results. We thus performed a systematic review of the literature and meta-analyzed outcomes of pancreatic resections with and without intraoperative placement of drains.
Methods: A database search according to the PRISMA guidelines was performed for studies on pancreatic resection with and without intraperitoneal drainage. The subgroup 'pancreaticoduodenectomy' was analyzed separately. The quality of studies was assessed using the MINORS and STROBE criteria. Pooled estimates of morbidity, mortality and length of hospital stay were calculated using random effects models.
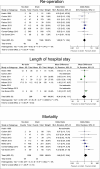
Results: Only two randomized trials were identified. Their results were contradictory. We thus included six further, retrospective studies in the meta-analysis. However, with I2 = 68% for any kind of complication, the estimate of inter-study heterogeneity was high. While overall morbidity after any kind of pancreatic resection was lower without drains (p = 0.04), there was no significant difference in mortality rates. In contrast, pooled estimates of outcomes after pancreaticoduodenectomy demonstrated no differences in morbidity (p = 0.40) but increased rates of intraabdominal abscesses (p = 0.04) and mortality (p = 0.04) without intraperitoneal drainage.
Conclusion: Although drains are associated with slightly increased morbidity for pancreatic resections, routine omission of drains cannot be advocated, especially after pancreaticoduodenectomy. While selective drainage seems reasonable, further efforts to generate more reliable data are questionable because of the current studies and the presumed small differences in outcomes.
Trial registration: Systematic review registration number CRD42014007497.
Figures





Similar articles
-
Prophylactic abdominal drainage for pancreatic surgery.Cochrane Database Syst Rev. 2018 Jun 21;6(6):CD010583. doi: 10.1002/14651858.CD010583.pub4. Cochrane Database Syst Rev. 2018. Update in: Cochrane Database Syst Rev. 2021 Dec 18;12:CD010583. doi: 10.1002/14651858.CD010583.pub5. PMID: 29928755 Free PMC article. Updated.
-
Duodenum-preserving pancreatic resection versus pancreaticoduodenectomy for chronic pancreatitis.Cochrane Database Syst Rev. 2016 Feb 3;2(2):CD011521. doi: 10.1002/14651858.CD011521.pub2. Cochrane Database Syst Rev. 2016. PMID: 26837472 Free PMC article.
-
Prophylactic abdominal drainage for pancreatic surgery.Cochrane Database Syst Rev. 2016 Oct 21;10(10):CD010583. doi: 10.1002/14651858.CD010583.pub3. Cochrane Database Syst Rev. 2016. Update in: Cochrane Database Syst Rev. 2018 Jun 21;6:CD010583. doi: 10.1002/14651858.CD010583.pub4. PMID: 27764898 Free PMC article. Updated.
-
Prophylactic abdominal drainage for pancreatic surgery.Cochrane Database Syst Rev. 2015 Aug 21;(8):CD010583. doi: 10.1002/14651858.CD010583.pub2. Cochrane Database Syst Rev. 2015. Update in: Cochrane Database Syst Rev. 2016 Oct 21;10:CD010583. doi: 10.1002/14651858.CD010583.pub3. PMID: 26292656 Updated.
-
Prophylactic abdominal drainage for pancreatic surgery.Cochrane Database Syst Rev. 2025 May 16;5(5):CD010583. doi: 10.1002/14651858.CD010583.pub6. Cochrane Database Syst Rev. 2025. PMID: 40377137 Review.
Cited by
-
Perioperative application of somatostatin analogs for pancreatic surgery-current status in Germany.Langenbecks Arch Surg. 2016 Nov;401(7):1037-1044. doi: 10.1007/s00423-016-1502-4. Epub 2016 Sep 15. Langenbecks Arch Surg. 2016. PMID: 27628685
-
Innovations in pancreatic anastomosis technique during pancreatoduodenectomies.Langenbecks Arch Surg. 2020 Nov;405(7):1039-1044. doi: 10.1007/s00423-020-01942-8. Epub 2020 Jul 31. Langenbecks Arch Surg. 2020. PMID: 32737588 Free PMC article.
-
Intra-abdominal drainage following pancreatic resection: A systematic review.World J Gastroenterol. 2015 Oct 28;21(40):11458-68. doi: 10.3748/wjg.v21.i40.11458. World J Gastroenterol. 2015. PMID: 26523110 Free PMC article.
-
Polyester Preserves the Highest Breaking Point After Prolonged Incubation in Pancreatic Juice.J Gastrointest Surg. 2018 Mar;22(3):444-450. doi: 10.1007/s11605-017-3558-z. Epub 2017 Aug 31. J Gastrointest Surg. 2018. PMID: 28861698
-
The Choice of the Most Appropriate Suture Threads for Pancreatic Anastomoses on the Basis of Their Mechanical Characteristics.Biomedicines. 2023 Mar 30;11(4):1055. doi: 10.3390/biomedicines11041055. Biomedicines. 2023. PMID: 37189673 Free PMC article.
References
-
- van der Wilt AA, Coolsen MM, de Hingh IH, van der Wilt GJ, Groenewoud H, Dejong CH, van Dam RM. To drain or not to drain: a cumulative meta-analysis of the use of routine abdominal drains after pancreatic resection. HPB. 2013;15(5):337–344. doi: 10.1111/j.1477-2574.2012.00609.x. - DOI - PMC - PubMed
-
- Jeekel J. No abdominal drainage after Whipple’s procedure. Br J Surg. 1992;79(2):182. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

