Diagnosis and management of choledocholithiasis in the golden age of imaging, endoscopy and laparoscopy
- PMID: 25309071
- PMCID: PMC4188892
- DOI: 10.3748/wjg.v20.i37.13382
Diagnosis and management of choledocholithiasis in the golden age of imaging, endoscopy and laparoscopy
Abstract
Biliary lithiasis is an endemic condition in both Western and Eastern countries, in some studies affecting 20% of the general population. In up to 20% of cases, gallbladder stones are associated with common bile duct stones (CBDS), which are asymptomatic in up to one half of cases. Despite the wide variety of examinations and techniques available nowadays, two main open issues remain without a clear answer: how to cost-effectively diagnose CBDS and, when they are finally found, how to deal with them. CBDS diagnosis and management has radically changed over the last 30 years, following the dramatic diffusion of imaging, including endoscopic ultrasound (EUS) and magnetic resonance cholangiography (MRC), endoscopy and laparoscopy. Since accuracy, invasiveness, potential therapeutic use and cost-effectiveness of imaging techniques used to identify CBDS increase together in a parallel way, the concept of "risk of carrying CBDS" has become pivotal to identifying the most appropriate management of a specific patient in order to avoid the risk of "under-studying" by poor diagnostic work up or "over-studying" by excessively invasive examinations. The risk of carrying CBDS is deduced by symptoms, liver/pancreas serology and ultrasound. "Low risk" patients do not require further examination before laparoscopic cholecystectomy. Two main "philosophical approaches" face each other for patients with an "intermediate to high risk" of carrying CBDS: on one hand, the "laparoscopy-first" approach, which mainly relies on intraoperative cholangiography for diagnosis and laparoscopic common bile duct exploration for treatment, and, on the other hand, the "endoscopy-first" attitude, variously referring to MRC, EUS and/or endoscopic retrograde cholangiography for diagnosis and endoscopic sphincterotomy for management. Concerning CBDS diagnosis, intraoperative cholangiography, EUS and MRC are reported to have similar results. Regarding management, the recent literature seems to show better short and long term outcome of surgery in terms of retained stones and need for further procedures. Nevertheless, open surgery is invasive, whereas the laparoscopic common bile duct clearance is time consuming, technically demanding and involves dedicated instruments. Thus, although no consensus has been achieved and CBDS management seems more conditioned by the availability of instrumentation, personnel and skills than cost-effectiveness, endoscopic treatment is largely preferred worldwide.
Keywords: Biliary lithiasis; Choledocholithiasis; Diagnosis; Endoscopy; Laparoscopy; Management.
Figures



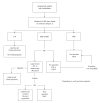
References
-
- Everhart JE, Khare M, Hill M, Maurer KR. Prevalence and ethnic differences in gallbladder disease in the United States. Gastroenterology. 1999;117:632–639. - PubMed
-
- Aerts R, Penninckx F. The burden of gallstone disease in Europe. Aliment Pharmacol Ther. 2003;18 Suppl 3:49–53. - PubMed
-
- Menezes N, Marson LP, debeaux AC, Muir IM, Auld CD. Prospective analysis of a scoring system to predict choledocholithiasis. Br J Surg. 2000;87:1176–1181. - PubMed
-
- Videhult P, Sandblom G, Rasmussen IC. How reliable is intraoperative cholangiography as a method for detecting common bile duct stones? : A prospective population-based study on 1171 patients. Surg Endosc. 2009;23:304–312. - PubMed
-
- Borzellino G, Rodella L, Saladino E, Catalano F, Politi L, Minicozzi A, Cordiano C. Treatment for retained [corrected] common bile duct stones during laparoscopic cholecystectomy: the rendezvous technique. Arch Surg. 2010;145:1145–1149. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

