Interventional treatment for unresectable hepatocellular carcinoma
- PMID: 25309076
- PMCID: PMC4188897
- DOI: 10.3748/wjg.v20.i37.13453
Interventional treatment for unresectable hepatocellular carcinoma
Abstract
Hepatocellular carcinoma (HCC) is the sixth most common cancer and third leading cause of cancer-related death in the world. The Barcelona clinic liver cancer classification is the current standard classification system for the clinical management of patients with HCC and suggests that patients with intermediate-stage HCC benefit from transcatheter arterial chemoembolization (TACE). Interventional treatments such as TACE, balloon-occluded TACE, drug-eluting bead embolization, radioembolization, and combined therapies including TACE and radiofrequency ablation, continue to evolve, resulting in improved patient prognosis. However, patients with advanced-stage HCC typically receive only chemotherapy with sorafenib, a multi-kinase inhibitor, or palliative and conservative therapy. Most patients receive palliative or conservative therapy only, and approximately 50% of patients with HCC are candidates for systemic therapy. However, these patients require therapy that is more effective than sorafenib or conservative treatment. Several researchers try to perform more effective therapies, such as combined therapies (TACE with radiotherapy and sorafenib with TACE), modified TACE for HCC with arterioportal or arteriohepatic vein shunts, TACE based on hepatic hemodynamics, and isolated hepatic perfusion. This review summarizes the published data and data on important ongoing studies concerning interventional treatments for unresectable HCC and discusses the technical improvements in these interventions, particularly for advanced-stage HCC.
Keywords: Advanced-stage; Hepatocellular carcinoma; Intermediate-stage; Interventional; Unresectable.
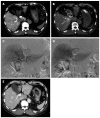
Figures
Similar articles
-
Transarterial radioembolization versus chemoembolization for the treatment of hepatocellular carcinoma (TRACE): study protocol for a randomized controlled trial.Trials. 2012 Aug 23;13:144. doi: 10.1186/1745-6215-13-144. Trials. 2012. PMID: 22913492 Free PMC article. Clinical Trial.
-
Transcatheter arterial chemoembolization based on hepatic hemodynamics for hepatocellular carcinoma.ScientificWorldJournal. 2013 Mar 27;2013:479805. doi: 10.1155/2013/479805. Print 2013. ScientificWorldJournal. 2013. PMID: 23606815 Free PMC article. Review.
-
Transarterial chemoembolization in hepatocellular carcinoma treatment: Barcelona clinic liver cancer staging system.World J Gastroenterol. 2015 Sep 28;21(36):10327-35. doi: 10.3748/wjg.v21.i36.10327. World J Gastroenterol. 2015. PMID: 26420959 Free PMC article. Review.
-
Transcatheter Arterial Chemoembolization With or Without Radiofrequency Ablation: Outcomes in Patients With Barcelona Clinic Liver Cancer Stage B Hepatocellular Carcinoma.AJR Am J Roentgenol. 2018 Apr;210(4):891-898. doi: 10.2214/AJR.17.18177. Epub 2018 Feb 7. AJR Am J Roentgenol. 2018. PMID: 29412017
-
Transarterial chemoembolization and radioembolization.Semin Liver Dis. 2014 Nov;34(4):435-43. doi: 10.1055/s-0034-1394142. Epub 2014 Nov 4. Semin Liver Dis. 2014. PMID: 25369305 Review.
Cited by
-
Clinical features and prognostic factors of patients with inoperable hepatocellular carcinoma treated with chemotherapy: a population-based study.J Gastrointest Oncol. 2024 Jun 30;15(3):1122-1140. doi: 10.21037/jgo-24-298. Epub 2024 Jun 20. J Gastrointest Oncol. 2024. PMID: 38989427 Free PMC article.
-
Landscape of transarterial chemoembolization represented interventional therapy for hepatocellular carcinoma.World J Gastrointest Surg. 2024 Dec 27;16(12):3903-3906. doi: 10.4240/wjgs.v16.i12.3903. World J Gastrointest Surg. 2024. PMID: 39734435 Free PMC article.
-
Autophagy-related cell death by pan-histone deacetylase inhibition in liver cancer.Oncotarget. 2016 May 17;7(20):28998-9010. doi: 10.18632/oncotarget.8585. Oncotarget. 2016. PMID: 27058414 Free PMC article.
-
Overexpression of long non-coding RNAs DUXAP9 and DUXAP10 is associated with prognosis in patients with hepatocellular carcinoma after hepatectomy.Int J Clin Exp Pathol. 2018 Mar 1;11(3):1407-1414. eCollection 2018. Int J Clin Exp Pathol. 2018. PMID: 31938237 Free PMC article.
-
Comparing the long-term efficacy of standard and combined minimally invasive procedures for unresectable HCC: a mixed treatment comparison.Oncotarget. 2017 Feb 28;8(9):15101-15113. doi: 10.18632/oncotarget.13145. Oncotarget. 2017. PMID: 27835871 Free PMC article.
References
-
- Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90. - PubMed
-
- Llovet JM, Brú C, Bruix J. Prognosis of hepatocellular carcinoma: the BCLC staging classification. Semin Liver Dis. 1999;19:329–338. - PubMed
-
- Llovet JM, Burroughs A, Bruix J. Hepatocellular carcinoma. Lancet. 2003;362:1907–1917. - PubMed
-
- Cabrera R, Nelson DR. Review article: the management of hepatocellular carcinoma. Aliment Pharmacol Ther. 2010;31:461–476. - PubMed
-
- Llovet JM, Ricci S, Mazzaferro V, Hilgard P, Gane E, Blanc JF, de Oliveira AC, Santoro A, Raoul JL, Forner A, et al. Sorafenib in advanced hepatocellular carcinoma. N Engl J Med. 2008;359:378–390. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

