Cortisol levels in former preterm children at school age are predicted by neonatal procedural pain-related stress
- PMID: 25313535
- PMCID: PMC4268136
- DOI: 10.1016/j.psyneuen.2014.09.018
Cortisol levels in former preterm children at school age are predicted by neonatal procedural pain-related stress
Abstract
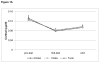
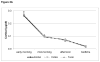
Early life stress can alter hypothalamic pituitary adrenal (HPA) axis function. Differences in cortisol levels have been found in preterm infants exposed to substantial procedural stress during neonatal intensive care, compared to infants born full-term, but only a few studies investigated whether altered programming of the HPA axis persists past toddler age. Further, there is a dearth of knowledge of what may contribute to these changes in cortisol. This prospective cohort study examined the cortisol profiles in response to the stress of cognitive assessment, as well as the diurnal rhythm of cortisol, in children (n=129) born at varying levels of prematurity (24-32 weeks gestation) and at full-term (38-41 weeks gestation), at age 7 years. Further, we investigated the relationships among cortisol levels and neonatal procedural pain-related stress (controlling for multiple medical confounders), concurrent maternal factors (parenting stress, depressive and anxiety symptoms) and children's behavioral problems. For each aim we investigate acute cortisol response profiles to a cognitive challenge as well as diurnal cortisol patterns at home. We hypothesized that children born very preterm will differ in their pattern of cortisol secretion from children born full-term, possibly depended on concurrent child and maternal factors, and that exposure to neonatal pain-related stress would be associated with altered cortisol secretion in children born very preterm, possibly in a sex-dependent way. Saliva samples were collected from 7-year old children three times during a laboratory visit for assessment of cognitive and executive functions (pretest, mid-test, end-study day acute stress profile) and at four times over two consecutive non-school days at home (i.e. morning, mid-morning, afternoon and bedtime-diurnal rhythm profile). We found that cortisol profiles were similar in preterm and full-term children, albeit preterms had slightly higher cortisol at bedtime compared to full-term children. Importantly, in the preterm group, greater neonatal procedural pain-related stress (adjusted for morphine) was associated with lower cortisol levels on the study day (p=.044) and lower diurnal cortisol at home (p=.023), with effects found primarily in boys. In addition, child attention problems were negatively, and thought problems were positively, associated with the cortisol response during cognitive assessment on the study day in preterm children. Our findings suggest that neonatal pain/stress contributes to altered HPA axis function up to school-age in children born very preterm, and that sex may be an important factor.
Keywords: Child; Cortisol; HPA axis; Internalizing behavior; Low birth weight; Maternal interaction; Pain; Preterm; Sex; Stress.
Copyright © 2014 Elsevier Ltd. All rights reserved.
Conflict of interest statement
Conflict of Interest
All authors declare that they have no conflict of interest.
Figures


References
-
- Aarnoudse-Moens CS, Weisglas-Kuperus N, van Goudoever JB, Oosterlaan J. Meta-analysis of neurobehavioral outcomes in very preterm and/or very low birth weight children. Pediatrics. 2009;124:717–728. - PubMed
-
- Abidin RR. Parenting Stress Index. Psychology Resources; Odessa, FL: 1995.
-
- Achenbach TM, Ruffle TM. The Child Behavior Checklist and related forms for assessing behavioral/emotional problems and competencies. Pediatr Rev. 2000;21:265–271. - PubMed
-
- Auerbach SM, Spielberger CD. The assessment of state and trait anxiety with the Rorschach test. J Pers Assess. 1972;36:314–335. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

