Decreased bacterial diversity characterizes the altered gut microbiota in patients with psoriatic arthritis, resembling dysbiosis in inflammatory bowel disease
- PMID: 25319745
- PMCID: PMC4280348
- DOI: 10.1002/art.38892
Decreased bacterial diversity characterizes the altered gut microbiota in patients with psoriatic arthritis, resembling dysbiosis in inflammatory bowel disease
Abstract
Objective: To characterize the diversity and taxonomic relative abundance of the gut microbiota in patients with never-treated, recent-onset psoriatic arthritis (PsA).
Methods: High-throughput 16S ribosomal RNA pyrosequencing was utilized to compare the community composition of gut microbiota in patients with PsA (n = 16), patients with psoriasis of the skin (n = 15), and healthy, matched control subjects (n = 17). Samples were further assessed for the presence and levels of fecal and serum secretory IgA (sIgA), proinflammatory proteins, and fatty acids.
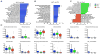
Results: The gut microbiota observed in patients with PsA and patients with skin psoriasis was less diverse when compared to that in healthy controls. This could be attributed to the reduced presence of several taxa. Samples from both patient groups showed a relative decrease in abundance of Coprococcus species, while samples from PsA patients were also characterized by a significant reduction in Akkermansia, Ruminococcus, and Pseudobutyrivibrio. Supernatants of fecal samples from PsA patients revealed an increase in sIgA levels and decrease in RANKL levels. Analysis of fatty acids revealed low fecal quantities of hexanoate and heptanoate in both patients with PsA and patients with psoriasis.
Conclusion: Patients with PsA and patients with skin psoriasis had a lower relative abundance of multiple intestinal bacteria. Although some genera were concomitantly decreased in both conditions, PsA samples had a lower abundance of reportedly beneficial taxa. This gut microbiota profile in PsA was similar to that previously described in patients with inflammatory bowel disease and was associated with changes in specific inflammatory proteins unique to this group, and distinct from that in patients with skin psoriasis and healthy controls. Thus, the role of the gut microbiome in the continuum of psoriasis-PsA pathogenesis and the associated immune response merits further study.
Copyright © 2015 by the American College of Rheumatology.
Figures


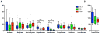

Comment in
-
Reply: To PMID 25319745.Arthritis Rheumatol. 2015 May;67(8):2280-2. doi: 10.1002/art.39152. Arthritis Rheumatol. 2015. PMID: 25891517 Free PMC article. No abstract available.
-
Gut-brain axis dysfunction may be associated with psoriatic arthritis: comment on the article by Scher et al.Arthritis Rheumatol. 2015 May;67(8):2280. doi: 10.1002/art.39151. Arthritis Rheumatol. 2015. PMID: 25919422 No abstract available.
References
-
- Eder L, Chandran V, Pellet F, Shanmugarajah S, Rosen CF, Bull SB, et al. Human leucocyte antigen risk alleles for psoriatic arthritis among patients with psoriasis. Ann Rheum Dis. 2012;71:50–5. - PubMed
-
- Winchester R, Minevich G, Steshenko V, Kirby B, Kane D, Greenberg DA, et al. HLA associations reveal genetic heterogeneity in psoriatic arthritis and in the psoriasis phenotype. Arthritis Rheum. 2012;64:1134–44. - PubMed
-
- Cua DJ, Sherlock JP. Autoimmunity’s collateral damage: Gut microbiota strikes ‘back’. Nat Med. 2011;17:1055–6. - PubMed
-
- Van Praet L, Van den Bosch F, Mielants H, Elewaut D. Mucosal inflammation in spondylarthritides: past, present, and future. Curr Rheumatol Rep. 2011;13:409–15. - PubMed
-
- Sherlock JP, Joyce-Shaikh B, Turner SP, Chao CC, Sathe M, Grein J, et al. IL-23 induces spondyloarthropathy by acting on ROR-gammat+ CD3+CD4-CD8- entheseal resident T cells. Nat Med. 2012;18:1069–76. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

