Lobectomy, sublobar resection, and stereotactic ablative radiotherapy for early-stage non-small cell lung cancers in the elderly
- PMID: 25321323
- PMCID: PMC4401470
- DOI: 10.1001/jamasurg.2014.556
Lobectomy, sublobar resection, and stereotactic ablative radiotherapy for early-stage non-small cell lung cancers in the elderly
Abstract
Importance: The incidence of early-stage non-small cell lung cancer (NSCLC) among the elderly is expected to rise dramatically owing to demographic trends and increased computed tomographic screening. However, to our knowledge, no modern trials have compared the most common treatments for NSCLC.
Objective: To determine clinical characteristics and survival outcomes associated with the 3 most commonly used definitive therapies for early-stage NSCLC in the elderly.
Design, setting, and participants: The Surveillance, Epidemiology, and End Results database linked to Medicare was used to determine the baseline characteristics and outcomes of 9093 patients with early-stage, node-negative NSCLC who underwent definitive treatment consisting of lobectomy, sublobar resection, or stereotactic ablative radiotherapy (SABR) from January 1, 2003, through December 31, 2009.
Main outcomes and measures: Overall and lung cancer-specific survival were compared using Medicare claims through December 31, 2012. We used proportional hazards regression and propensity score matching to adjust outcomes for key patient, tumor, and practice environment factors.
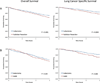
Results: The median age was 75 years, and treatment distribution was 79.3% for lobectomy, 16.5% for sublobar resection, and 4.2% for SABR. Unadjusted 90-day mortality was highest for lobectomy (4.0%) followed by sublobar resection (3.7%; P = .79) and SABR (1.3%; P = .008). At 3 years, unadjusted mortality was lowest for lobectomy (25.0%), followed by sublobar resection (35.3%; P < .001) and SABR (45.1%; P < .001). Proportional hazards regression demonstrated that sublobar resection was associated with worse overall survival (adjusted hazard ratio [AHR], 1.32 [95% CI, 1.20-1.44]; P < .001) and lung cancer-specific survival (AHR, 1.50 [95% CI, 1.29-1.75]; P < .001) compared with lobectomy. Propensity score-matching analysis reiterated these findings for overall survival (AHR, 1.36 [95% CI, 1.17-1.58]; P < .001) and lung cancer-specific survival (AHR, 1.46 [95% CI, 1.13-1.90]; P = .004). In proportional hazards regression, SABR was associated with better overall survival than lobectomy in the first 6 months after diagnosis (AHR, 0.45 [95% CI, 0.27-0.75]; P < .001) but worse survival thereafter (AHR, 1.66 [95% CI, 1.39-1.99]; P < .001). Propensity score-matching analysis of well-matched SABR and lobectomy cohorts demonstrated similar overall survival in both groups (AHR, 1.01 [95% CI, 0.74-1.38]; P = .94).
Conclusions and relevance: Lobectomy was associated with better outcomes than sublobar resection in elderly patients with early-stage NSCLC. Propensity score matching suggests that SABR may be a good option among patients with very advanced age and multiple comorbidities.
Conflict of interest statement
There are no other conflicts of interest to report.
Figures
References
-
- Smith BD, Smith GL, Hurria A, Hortobagyi GN, Buchholz TA. Future of cancer incidence in the United States: burdens upon an aging, changing nation. J Clin Oncol. 2009 Jun 10;27(17):2758–2765. - PubMed
-
- Ginsberg R, Rubinstein L. Randomized trial of lobectomy versus limited resection for T1 N0 non-small cell lung cancer. Lung Cancer Study Group. The Annals of Thoracic Surgery. 1995;60:615–622. - PubMed
-
- Martin-Ucar AE, Nakas A, Pilling JE, West KJ, Waller DA. A case-matched study of anatomical segmentectomy versus lobectomy for stage I lung cancer in high-risk patients. European journal of cardio-thoracic surgery : official journal of the European Association for Cardio-thoracic Surgery. 2005 Apr;27(4):675–679. - PubMed
-
- Schuchert MJ, Pettiford BL, Keeley S, et al. Anatomic segmentectomy in the treatment of stage I non-small cell lung cancer. Ann Thorac Surg. 2007 Sep;84(3):926–932. discussion 932-923. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical