Interventions for managing asthma in pregnancy
- PMID: 25331331
- PMCID: PMC6599853
- DOI: 10.1002/14651858.CD010660.pub2
Interventions for managing asthma in pregnancy
Abstract
Background: Asthma is the most common respiratory disorder complicating pregnancy, and is associated with a range of adverse maternal and perinatal outcomes. There is strong evidence however, that the adequate control of asthma can improve health outcomes for mothers and their babies. Despite known risks of poorly controlled asthma during pregnancy, a large proportion of women have sub-optimal asthma control, due to concerns surrounding risks of pharmacological agents, and uncertainties regarding the effectiveness and safety of different management strategies.
Objectives: To assess the effects of interventions (pharmacologic and non-pharmacologic) for managing women's asthma in pregnancy on maternal and fetal/infant outcomes.
Search methods: We searched the Cochrane Pregnancy and Childbirth Group's Trials Register (2 June 2014) and the Cochrane Airways Group's Trials Register (4 June 2014).
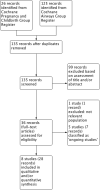
Selection criteria: Randomised and quasi-randomised controlled trials comparing any intervention used to manage asthma in pregnancy, with placebo, no intervention, or an alternative intervention. We included pharmacological and non-pharmacological interventions (including combined interventions). Cluster-randomised trials were eligible for inclusion (but none were identified). Cross-over trials were not eligible for inclusion.We included multi-armed trials along with two-armed trials. We also included studies published as abstracts only.
Data collection and analysis: At least two review authors independently assessed trial eligibility and quality and extracted data. Data were checked for accuracy.
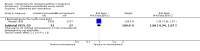
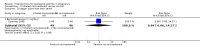
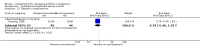
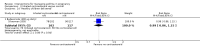
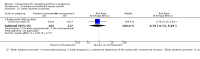
Main results: We included eight trials in this review, involving 1181 women and their babies. Overall we judged two trials to be at low risk of bias, two to be of unclear risk of bias, and four to be at moderate risk of bias.Five trials assessed pharmacological agents, including inhaled corticosteroids (beclomethasone or budesonide), inhaled magnesium sulphate, intravenous theophylline, and inhaled beclomethasone verus oral theophylline. Three trials assessed non-pharmacological interventions, including a fractional exhaled nitric oxide (FENO)-based algorithm versus a clinical guideline-based algorithm to adjust inhaled corticosteroid therapy, a pharmacist-led multi-disciplinary approach to management versus standard care, and progressive muscle relaxation (PMR) versus sham training.The eight included trials were assessed under seven separate comparisons. Pharmacological interventionsPrimary outcomes: one trial suggested that inhaled magnesium sulphate in addition to usual treatment could reduce exacerbation frequency in acute asthma (mean difference (MD) -2.80; 95% confidence interval (CI) -3.21 to -2.39; 60 women). One trial assessing the addition of intravenous theophylline to standard care in acute asthma did not report on exacerbations (65 women). No clear difference was shown in the risk of exacerbations with the use of inhaled beclomethasone in addition to usual treatment for maintenance therapy in one trial (risk ratio (RR) 0.36; 95% CI 0.13 to 1.05; 60 women); a second trial also showed no difference, however data were not clearly reported to allow inclusion in a meta-analysis. No difference was shown when inhaled beclomethasone was compared with oral theophylline for maintenance therapy (RR 0.88; 95% CI 0.59 to 1.33; one trial, 385 women). None of these trials reported on neonatal intensive care admissions.
Secondary outcomes: inhaled magnesium sulphate in acute asthma was shown to improve lung function measures (one trial, 60 women); intravenous theophylline in acute asthma was not associated with benefits (one trial, 65 women). No clear differences were seen with the addition of inhaled corticosteroids to routine treatment in three trials (374 women). While inhaled beclomethasone, compared with oral theophylline, significantly reduced treatment discontinuation due to adverse effects in one trial (384 women), no other differences were observed, except for higher treatment adherence with theophylline. Four of the five trials did not report on adverse effects. Non-pharmacological interventionsPrimary outcomes: in one trial, the use of a FENO-based algorithm was shown to significantly reduce asthma exacerbations (RR 0.61; 95% CI 0.41 to 0.90; 220 women); and a trend towards fewer neonatal hospitalisations was observed (RR 0.46; 95% CI 0.21 to 1.02; 214 infants). No exacerbations occurred in one trial assessing pharmacist-led management; this approach did not reduce neonatal intensive care admissions (RR 1.50; 95% CI 0.27 to 8.32; 58 infants). One trial (64 women) assessing PMR did not report on exacerbations or neonatal intensive care admissions.
Secondary outcomes: the use of a FENO-based algorithm to adjust therapy led to some improvements in quality of life scores, as well as more frequent use of inhaled corticosteroids and long-acting β-agonists, and less frequent use of short-acting β-agonists (one trial, 220 women). The FENO-based algorithm was associated with fewer infants with recurrent episodes of bronchiolitis in their first year of life, and a trend towards fewer episodes of croup for infants. Pharmacist-led management improved asthma control scores at six months (one trial, 60 women); PMR improved lung function and quality of life measures (one trial, 64 women). No other differences between comparisons were observed.
Authors' conclusions: Based on eight included trials, of moderate quality overall, no firm conclusions about optimal interventions for managing asthma in pregnancy can be made. Five trials assessing pharmacological interventions did not provide clear evidence of benefits or harms to support or refute current practice. While inhaled magnesium sulphate for acute asthma was shown to reduce exacerbations, this was in one small trial of unclear quality, and thus this finding should be interpreted with caution. Three trials assessing non-pharmacological interventions provided some support for the use of such strategies, however were not powered to detect differences in important maternal and infant outcomes. While a FENO-based algorithm reduced exacerbations, the effects on perinatal outcomes were less certain, and thus widespread implementation is not yet appropriate. Similarly, though positive effects on asthma control were shown with PMR and pharmacist-led management, the evidence to date is insufficient to draw definitive conclusions.In view of the limited evidence base, further randomised trials are required to determine the most effective and safe interventions for asthma in pregnancy. Future trials must be sufficiently powered, and well-designed, to allow differences in important outcomes for mothers and babies to be detected. The impact on health services requires evaluation. Any further trials assessing pharmacological interventions should assess novel agents or those used in current practice. Encouragingly, at least five trials have been identified as planned or underway.
Conflict of interest statement
Vicki Clifton was an investigator on the 'Managing Asthma in Pregnancy (MAP)' Study (Powell 2011). All tasks relating to this study (assessment of eligibility for inclusion, assessment of risk of bias, data extraction) were carried out by other members of the review team who were not directly involved in the trial. Vicki Clifton is also an investigator on two of the ongoing trials (ACTRN12613000244707; ACTRN12613000301763), and Philippa Middleton is an investigator on one of these trial (ACTRN12613000244707). Therefore, in future updates of this review, all tasks relating to these studies (assessment of eligibility for inclusion; and if included, assessment of risk of bias, data extraction etc.) will be carried out by other members of the review team who are not directly involved in the trials.
None known for other authors.
Figures



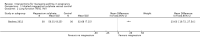



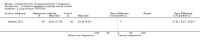
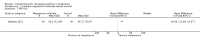




























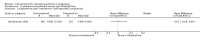



















































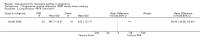


Update of
References
References to studies included in this review
Badawy 2012 {published data only}
-
- Badawy M, Hasannen I. The value of magnesium sulfate nebulization in treatment of acute bronchial asthma during pregnancy. European Respiratory Journal: European Respiratory Society Annual Congress, Vienna, Austria, September 1‐5 2012. 2012; Vol. 40:311s [P1789].
-
- Badawy MSH, Hassanin IMA. The value of magnesium sulfate nebulization in treatment of acute bronchial asthma during pregnancy. Egyptian Journal of Chest Diseases and Tuberculosis 2014;63:285‐9.
Caramez 1998 {published data only}
-
- Caramez MPR, Grunauer MA, Boueri FMV, Cotrin D, Perez AM, Zuccato APA, et al. Effect of continuous inhaled beclomethasone for asthmatic pregnant patients on asthma control and perinatal outcome: a randomized controlled study [abstract]. American Journal of Respiratory and Critical Care Medicine 1998;157(3 Suppl):A621.
Dombrowski 2004 {published data only}
-
- Dombrowski M, NICHD, MFMU Network and, NHLBI. Randomized trial of inhaled beclomethasone versus theophylline for asthma during pregnancy [abstract]. American Journal of Obstetrics and Gynecology 2001;184(1):S2. - PubMed
-
- Dombrowski M, Thom E, McNellis D. Maternal‐fetal medicine units (mfmu) studies of inhaled corticosteroids during pregnancy. Journal of Allergy and Clinical Immunology 1999;103(2 Pt 2):S356‐9. - PubMed
-
- Dombrowski MP, Schatz M, Wise R, Thom EA, Landon M, Mabie W, et al. Randomized trial of inhaled beclomethasone dipropionate versus theophylline for moderate asthma during pregnancy. American Journal of Obstetrics and Gynecology 2004;190:737‐44. - PubMed
-
- Schatz M. The relationship of asthma‐specific quality of life during pregnancy to asthma morbidity and perinatal outcomes. American Thoracic Society International Conference; 2007 May 18‐23; San Francisco, California, USA. 2007.
Lim 2012 {published data only}
-
- Lim A, Stewart K, Abramson M, Walker S, George J. A multidisciplinary approach to management of maternal asthma (MAMMA). How can we help?. Respirology 2013;18(Suppl 2):45 [P029].
-
- Lim A, Stewart K, Abramson M, Walker S, George J. Testing a multidisciplinary approach to management of maternal asthma (MAMMA©) using a randomised controlled trial – how can we help?. Allergy 2013;68(Suppl 97):164‐5 [P352].
-
- Lim AS, Stewart K, Abramson MJ, Walker SP, Smith CL, George J. Multidisciplinary approach to management of maternal asthma (MAMMA): a randomized controlled trial. Chest 2014;145(5):1046‐54. - PubMed
Nickel 2006 {published data only}
-
- Nickel C, Lahmann C, Muehlbacher M, Gill FP, Kaplan P, Buschmann W, et al. Pregnant women with bronchial asthma benefit from progressive muscle relaxation: a randomized, prospective, controlled trial. Psychotherapy and Psychosomatics 2006;75:237‐43. - PubMed
Powell 2011 {published data only}
-
- Gibson P. A double‐blind randomised controlled trial of FENO guided asthma therapy and clinical guideline asthma therapy in pregnant women with asthma to reduce asthma exacerbations. Australian New Zealand Clinical Trials Registry (www.anzctr.org.au) (accessed 19 February 2008).
-
- Gibson P, Powell H, Giles W, Clifton V, Hensley MJ, Taylor DR, et al. Asthma exacerbations during pregnancy are reduced by inflammometry (FENO) guided asthma management: a randomised controlled trial [abstract]. American Journal of Respiratory and Critical Care Medicine 2011;183:A6414.
-
- Mattes J, Murphy V, Powell H, Gibson P. The effect of better asthma control in pregnancy on wheezy illnesses in infancy [Abstract]. Respirology (Carlton, Vic.) 2013;18(Suppl 2):29 [O078].
-
- Powell H, McCaffery K, Murphy VE, Giles W, Clifton VL, Hensley MJ, et al. Psychosocial outcomes are related to future exacerbation risk and perinatal outcomes in pregnant women with asthma. Respirology 2012;17(Suppl 1):49. - PubMed
Silverman 2005 {published data only}
-
- Silverman M, Sheffer A, Diaz P, Lindmark B, Radner F, Broddene M. Prospective pregnancy outcome data in patients with newly diagnosed, mild persistent asthma treated with once‐daily budesonide: 5‐year results from the START study [Abstract]. American Thoracic Society 100th International Conference, May 21‐26, 2004, Orlando. 2004:A37 Poster J108.
-
- Silverman M, Sheffer A, Diaz PV, Lindmark B, Radner F, Broddene M, et al. Outcome of pregnancy in a randomized controlled study of patients with asthma exposed to budesonide. Annals of Allergy, Asthma, & Immunology 2005;95(6):566‐70. - PubMed
-
- Silverman M, Sheffer A, Woolcock AJ, Diaz Amor P, Lindmark B, Radner F, et al. Prospective pregnancy outcome data from the START study. On behalf of the START safety committee. European Respiratory Journal 2002;20(Suppl 38):53s.
Wendel 1996 {published data only}
-
- Wendel PJ, Ramin SM, Barnett‐Hamm C, Rowe TF, Cunningham FG. Asthma treatment in pregnancy: A randomized controlled study. American Journal of Obstetrics and Gynecology 1996;175:150‐4. - PubMed
-
- Wendel PJ, Ramin SM, Hamm CB, Rowe TF, Cummingham FG. A randomized controlled study of the management of asthma complicating pregnancy. American Journal of Obstetrics and Gynecology 1995;172:253.
References to studies excluded from this review
Schonberger 2004 {published data only}
-
- Schonberger HJ, Maas T, Dompeling E, Knottnerus JA, Weel C, Schayck CP. Compliance of asthmatic families with a primary prevention programme of asthma and effectiveness of measures to reduce inhalant allergens‐‐a randomized trial. Clinical & Experimental Allergy 2004;34(7):1024‐31. - PubMed
References to ongoing studies
ACTRN12613000202763 {published data only}
-
- ACTRN12613000202763. The Breathing for Life Trial: A multi‐centre randomised controlled trial of fractional exhaled nitric oxide based management of asthma during pregnancy and its impact on perinatal outcomes and infant and childhood respiratory health. https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?id=363154 (accessed 16 October 2013). - PMC - PubMed
ACTRN12613000244707 {published data only}
-
- ACTRN12613000244707. A randomised controlled trial to assess the clinical and cost effectiveness of a nurse‐led Antenatal Asthma Management Service (AAMS) for reducing asthma exacerbations during pregnancy. https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?ACTRN=1261... (accessed 16 October 2013).
ACTRN12613000301763 {published data only}
-
- ACTRN12613000301763. Dietary modification for asthma control in pregnancy. https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?ACTRN=1261... (accessed 16 October 2013).
ACTRN12613000800729 {published data only}
-
- ACTRN12613000800729. Management of asthma with supportive telehealth of respiratory function in pregnancy (MASTERY). https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?ACTRN=1261... (accessed 16 October 2013).
NCT01345396 {published data only}
-
- NCT01345396. Influence of an asthma education programme on asthma control during pregnancy. http://clinicaltrials.gov/ct2/show/NCT01345396. NCT01345396 (accessed 16 October 2013).
Additional references
Abramson 2001
-
- Abramson M, Bailey M, Couper F, Driver J, Drummer OH, Forbes A, et al. Are asthma medications and management related to deaths from asthma?. American Journal of Respiratory and Critical Care Medicine 2001;163:12‐8. - PubMed
ACOG 2002
-
- American College of Obstetricians and Gynecologists (ACOG) Committee Obstetric Practice. ACOG Committee opinion: exercise during pregnancy and the postpartum period No 267. Obstetrics and Gynecology 2002;99(1):171‐3. - PubMed
Adams 1999
-
- Adams NP, Bestall JC, Jones P. Budesonide versus placebo for chronic asthma in children and adults. Cochrane Database of Systematic Reviews 1999, Issue 4. [DOI: 10.1002/14651858.CD003274] - DOI
Adams 2005
Allam 2004
Arnold 2008
Bahna 1972
-
- Bahna SL, Bjerkedal T. The course and outcome of pregnancy in women with bronchial asthma. Acta Allergologica 1972;27(5):397‐406. - PubMed
Bailey 2009
Basheti 2007
-
- Basheti IA, Reddel HK, Armour CL, Bosnic‐Anticevich SZ. Improved asthma outcomes with a simple inhaler technique intervention by community pharmacists. Journal of Allergy and Clinical Immunology 2007;119(6):1537‐8. - PubMed
Blais 2009
-
- Blais L, Beauchesne MF, Lemière C, Elftouh N. High doses of inhaled corticosteroids during the first trimester of pregnancy and congenital malformations. Journal of Allergy and Clinical Immunology 2009;124(6):1229‐34. - PubMed
Bracken 2003
-
- Bracken MB, Triche EW, Belanger K, Saftlas A, Beckett WS, Leaderer BP. Asthma symptoms, severity, and drug therapy: a prospective study of effects on 2205 pregnancies. Obstetrics and Gynecology 2003;102(4):739‐52. - PubMed
Breton 2009
-
- Breton M‐C, Beauchesne M‐F, Lemière C, Rey É, Forget A, Blais L. Risk of perinatal mortality associated with asthma during pregnancy. Thorax 2009;64(2):101‐6. - PubMed
Campbell 2000
Carmichael 2007
-
- Carmichael SL, Shaw GM, Ma C, Werler MM, Rasmussen SA, Lammer EJ, et al. Maternal corticosteroid use and orofacial clefts. American Journal of Obstetrics and Gynecology 2007;197(6):e1–7. - PubMed
Chandratilleke 2012
Cheng 2003
Clifton 2009
-
- Clifton VL, Engel P, Smith R, Gibson P, Brinsmead M, Giles W. Maternal and neonatal outcomes of pregnancies complicated by asthma in an Australian population. Australian and New Zealand Journal of Obstetrics and Gynaecology 2009;49:619‐26. - PubMed
Dalziel 2005
-
- Dalziel SR, Walker NK, Parag V, Mantell C, Rea HH, Rodgers A, et al. Cardiovascular risk factors after antenatal exposure to betamethasone: 30‐year follow‐up of a randomised controlled trial. Lancet 2005;365(9474):1856‐62. - PubMed
Demissie 1998
-
- Demissie K, Breckenridge M, Rhoads G. Infant and maternal outcomes in the pregnancies of asthmatic women. American Journal of Respiratory and Critical Care Medicine 1998;158(4):1091‐5. - PubMed
Dombrowski 2004a
-
- Dombrowski MPMD, Schatz MMD, Wise RMD, Momirova VMS, Landon MMD, Mabie WMD, et al. Asthma during pregnancy. Obstetrics and Gynecology 2004;103(1):5‐12. - PubMed
Dombrowski 2006
-
- Dombrowski MP. Asthma and pregnancy. Obstetrics and Gynecology 2006;108(3 Pt 1):667‐81. - PubMed
Dombrowski 2008
-
- Dombrowski MP, Schatz M, ACOG Committee on Practice Bulletins‐Obstetrics. ACOG practice bulletin: clinical management guidelines for obstetrician‐gynecologists number 90, February 2008: asthma in pregnancy. Obstetrics and Gynecology 2008;111:457‐64. - PubMed
Enriquez 2007
-
- Enriquez R, Griffin MR, Carroll KN, Wu P, Cooper WO, Gebretsadik T, et al. Effect of maternal asthma and asthma control on pregnancy and perinatal outcomes. Journal of Allergy and Clinical Immunology 2007;120(3):625‐30. - PubMed
Gates 2004
-
- Gates S, Brocklehurst P. How should trials recruiting women with multiple pregnancies be analysed?. British Journal of Obstetrics and Gynaecology 2004;111:213‐9. - PubMed
George 2012
-
- George J, Abramson MJ, Walker SP. Asthma in pregnancy: are inhaled corticosteroids safe?. American Journal of Respiratory and Critical Care Medicine 2012;185(5):476‐8. - PubMed
Gibson 2002
Gibson 2004
Giles 2013
GINA 2001
-
- Global Initiative for Asthma (GINA). Asthma management and prevention: a practical guide for public health officials and health care professionals. Imperial College. London: GINA, 2001.
Gluck 2004
-
- Gluck J. The change of asthma course during pregnancy. Clinical Reviews in Allergy and Immunology 2004;26(3):171‐80. - PubMed
Gøtzsche 2008
Higgins 2011
-
- Higgins JPT, Green S, editors. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration, 2011. Available from www.cochrane‐handbook.org.
Hodyl 2011
-
- Hodyl NA, Stark MJ, Osei‐Kumah A, Bowman M, Gibson P, Clifton VL. Fetal glucocorticoid‐regulated pathways are not affected by inhaled corticosteroid use for asthma during pregnancy. American Journal of Respiratory and Critical Care Medicine 2011;183(6):716‐22. - PubMed
Hodyl 2014
-
- Hodyl NA, Stark MJ, Scheil W, Grzeskowiak LE, Clifton VL. Perinatal outcomes following maternal asthma and cigarette smoking during pregnancy. European Respiratory Journal 2014;43(3):704‐16. - PubMed
Holloway 2004
Holst 2009
-
- Holst L, Wright D, Nordeng H, Haavik S. Use of herbal preparations during pregnancy: Focus group discussion among expectant mothers attending a hospital antenatal clinic in Norwich, UK. Complementary Therapies in Clinical Practice 2009;15:225‐9. - PubMed
Hondras 2005
Huntley 2002
Jones 2000
Juniper 1993
-
- Juniper E, Newhouse M. Effect of pregnancy on asthma: a systematic review and meta‐analysis. In: Schatz M, Zaiger RS, Claman HC editor(s). Asthma and Immunological Diseases in Pregnancy and Early Infancy. New York: Marcel Dekker, 1993:401‐27.
Katz 2008
-
- Katz O, Sheiner E. Asthma and pregnancy: a review of two decades. Expert Review of Respiratory Medicine 2008;2(1):97‐107. - PubMed
Kaur 2009
Kilburn 2001
Kwon 2003
-
- Kwon HL, Belanger K, Bracken MB. Asthma prevalence among pregnant and childbearing‐aged women in the united states: estimates from national health surveys. Annals of Epidemiology 2003;13(5):317‐24. - PubMed
Kwon 2006
-
- Kwon HL, Triche EW, Belanger K, Bracken MB. The epidemiology of asthma during pregnancy: prevalence, diagnosis, and symptoms. Immunology and Allergy Clinics of North America 2006;26(1):29‐62. - PubMed
Källén 2000
-
- Källén B, Rydhstroem H, Åberg A. Asthma during pregnancy: a population based study. European Journal of Epidemiology 2000;16(2):167‐71. - PubMed
Källén 2007
-
- Källén B, Otterblad Olausson P. Use of anti‐asthmatic drugs during pregnancy. 3. Congenital malformations in the infants. European Journal of Clinical Pharmacology 2007;63:383‐8. - PubMed
Lawn 2013
Liccardi 2003
-
- Liccardi G, Cazzola M, Canonica GW, D'Amato M, D'Amato G, Passalacqua G. General strategy for the management of bronchial asthma in pregnancy. Respiratory Medicine 2003;97:778‐89. - PubMed
Lim 2011a
Lim 2011b
-
- Lim A, Stewart K, König K, George J. Systematic review of the safety of regular preventive asthma medications during pregnancy. Annals of Pharmacotherapy 2011;45(7‐8):931‐45. - PubMed
Lim 2012a
-
- Lim AS, Stewart K, Abramson MJ, Ryan K, George J. Asthma during pregnancy: the experiences, concerns and views of pregnant women with asthma. Journal of Asthma 2012;49(5):474‐9. - PubMed
Lin 2008
Liu 2001
-
- Liu S, Wen SW, Demissie K, Marcoux S, Kramer MS. Maternal asthma and pregnancy outcomes: a retrospective cohort study. American Journal of Obstetrics and Gynecology 2001;184(2):90‐6. - PubMed
McCarney 2004
McCarney 2009
McCusker 2011
-
- McCusker C, Hamid Q. Managing asthma during pregnancy. American Journal of Respiratory and Critical Care Medicine 2011;183(6):687‐8. - PubMed
Mehuys 2008
-
- Mehuys E, Bortel L, Bolle L, Tongelen I, Annemans L, Remon JP, et al. Effectiveness of pharmacist intervention for asthma control improvement. European Respiratory Journal 2009;31(4):790‐9. - PubMed
Mendola 2014
Mildenhall 2006
Murphy 2005a
-
- Murphy VE, Gibson PG, Talbot PI, Kessell CG, Clifton VE. Asthma self‐management skills and the use of asthma education during pregnancy. European Respiratory Journal 2005;26(3):435‐41. - PubMed
Murphy 2005b
-
- Murphy VE, Gibson P, Talbot P, Clifton VL. Severe asthma exacerbations during pregnancy. Obstetrics and Gynecology 2005;106(5):1046‐54. - PubMed
Murphy 2006
Murphy 2010
-
- Murphy VE, Clifton VL, Gibson PG. The effect of cigarette smoking on asthma control during exacerbations in pregnant women. Thorax 2010;65(8):739‐44. - PubMed
Murphy 2011
-
- Murphy VE, Namazy JA, Powell H, Schatz M, Chambers C, Attia J, et al. A meta‐analysis of adverse perinatal outcomes in women with asthma. British Journal of Obstetrics and Gynaecology 2011;118:1314‐23. - PubMed
NACA 2006
-
- National Asthma Council Australia. Asthma Management Handbook. Melbourne: NACA, 2006.
NAEPP 2005
-
- National Asthma Education and Prevention Program Working Group (NAEPP). Report on Managing Asthma During Pregnancy: Recommendations for Pharmacologic Treatment. Update 2004. National Institutes of Health, National Heart, Lung, and Blood Institute, 2005.
Nair 2012
Park‐Wyllie 2000
-
- Park‐Wyllie L, Mazzotta P, Pastuszak A, Moretti ME, Beique L, Hunnisett L, et al. Birth defects after maternal exposure to corticosteroids: prospective cohort study and meta‐analysis of epidemiological studies. Tetratology 2000;62(6):385‐92. - PubMed
Petsky 2007
Petsky 2009
Pogson 2011
Posadzki 2011
-
- Posadzki P, Ernst E. Yoga for asthma? A systematic review of randomized clinical trials. Journal of Asthma 2011;48:632‐9. - PubMed
Powell 2012
Ram 2003
RevMan 2014 [Computer program]
-
- The Nordic Cochrane Centre, The Cochrane Collaboration. Review Manager (RevMan). Version 5.3. Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2014.
Rodríguez‐Pinilla 1998
-
- Rodríguez‐Pinilla E, Martínez‐Frías ML. Corticosteroids during pregnancy and oral clefts: a case control study. Teratology 1998;58(1):2‐5. - PubMed
Ruffin 2001
-
- Ruffin R, Wilson D, Southcott A, Adams R. Prevalence, morbidity and management of adult asthma in South Australia. Immunology and Cell Biology 2001;79:191‐4. - PubMed
Ryan 2013
-
- Ryan C, McCullough A, Elborn S, Hughes C. Pharmacist‐led interventions for adults with asthma or COPD. Cochrane Database of Systematic Reviews 2013, Issue 4. [DOI: 10.1002/14651858.CD010418] - DOI
Saigal 2008
-
- Saigal S, Doyle LW. An overview of mortality and sequelae of preterm birth from infancy to adulthood. Lancet 2008;371:261‐9. - PubMed
Sawicki 2012
-
- Sawicki E, Steward K, Wong S, Paul E, Leung L, George J. Management of asthma by pregnant women attending an Australian Maternity Hospital. Australian and New Zealand Journal of Obstetrics and Gynaecology 2012;52:183‐8. - PubMed
Schatz 1995
-
- Schatz M, Zeiger RS, Hoffman CP, Harden K, Forsythe A, Chilingar L, et al. Perinatal outcomes in the pregnancies of asthmatic women: a prospective controlled analysis. Obstetrical and Gynecological Survey 1995;50(11):763‐4. - PubMed
Schatz 1999
-
- Schatz M. Interrelationships between asthma and pregnancy: a literature review. Journal of Allergy and Clinical Immunology 1999;103(2):S330‐6. - PubMed
Schatz 2006
-
- Schatz M, Dombrowski, MP, Wise R, Momirova V, Landon M, Mabie W, et al. Spirometry is related to perinatal outcomes in pregnant women with asthma. American Journal of Obstetrics and Gynaecology 2006;194(1):120‐6. - PubMed
Schatz 2009
-
- Schatz M, Dombrowski MP. Clinical practice. Asthma in pregnancy. New England Journal of Medicine 2009;360:1862‐9. - PubMed
Seddon 2006
Singh 2002
Tapp 2007
Tee 2007
Thien 2002
Westfall 2003
-
- Westfall RE. Herbal healing in pregnancy women's experiences. Journal of Herbal Pharmacotherapy 2003;3(4):17‐39. - PubMed
Yorke 2006
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

