Laparoscopic radical prostatectomy with bladder neck preservation: positive surgical margin and urinary continence status
- PMID: 25337159
- PMCID: PMC4198659
- DOI: 10.5114/wiitm.2014.45085
Laparoscopic radical prostatectomy with bladder neck preservation: positive surgical margin and urinary continence status
Abstract
Introduction: Preservation of the bladder neck (BN) has been controversial, as limited excision of the bladder neck may result in incomplete resection of the disease. Moreover, the urinary continence rate may not be improved.
Aim: To evaluate the effect of bladder neck sparing on urinary continence, and surgical margins status in prostate cancer (PCa) patients treated with laparoscopic radical extraperitoneal prostatectomy.
Material and methods: A retrospective analysis of 295 consecutive patients who had undergone laparoscopic radical extraperitoneal prostatectomy for clinically localised prostate cancer in a single institution was performed. Positive surgical margin (SM(+)) and urinary continence status at 3, 6, and 12 months were evaluated.
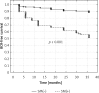
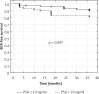
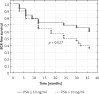
Results: The distribution of SM(+) for pT2, pT3, and pT4a was 15.3% (27/176), 49.1% (58/118), and 100% (1/1), respectively. Overall, there were 55.61%, 80.61%, and 84.69% of men continent at 3, 6, and 12 months, respectively. However, when limiting the analysis to those who did not receive adjuvant radiotherapy within 12 months following surgery, urinary continence rates were 59.23%, 85.86%, and 90.21% at 3, 6, and 12 months, respectively. Preoperative prostate-specific antigen (PSA) and pathological T stage were identified as significant predictors of positive surgical margins.
Conclusions: Laparoscopic radical extraperitoneal prostatectomy with bladder neck preservation has been a safe procedure which has resulted in good functional outcome. We observed a relatively high incidence of positive surgical margins which could be attributed to a large number of extracapsular disease cases.
Keywords: bladder neck preservation; laparoscopic radical prostatectomy; surgical margin; urinary continence.
Figures
Similar articles
-
Bladder neck preservation during classic laparoscopic radical prostatectomy - point of technique and preliminary results.Wideochir Inne Tech Maloinwazyjne. 2012 Jun;7(2):89-95. doi: 10.5114/wiitm.2011.25981. Epub 2011 Nov 30. Wideochir Inne Tech Maloinwazyjne. 2012. PMID: 23256008 Free PMC article.
-
[Urinary continence in laparoscopic radical prostatectomy with bladder neck preservation].Zhejiang Da Xue Xue Bao Yi Xue Ban. 2013 Nov;42(6):680-4. doi: 10.3785/j.issn.1008-9292.2013.06.016. Zhejiang Da Xue Xue Bao Yi Xue Ban. 2013. PMID: 24421237 Chinese.
-
The Impact of Three Different Bladder Neck Reconstruction Techniques on Urinary Continence after Laparoscopic Radical Prostatectomy.J Endourol. 2020 Jun;34(6):663-670. doi: 10.1089/end.2020.0064. Epub 2020 May 5. J Endourol. 2020. PMID: 32228027
-
Minimally Invasive Radical Prostatectomy after Previous Bladder Outlet Surgery: A Systematic Review and Pooled Analysis of Comparative Studies.J Urol. 2019 Sep;202(3):511-517. doi: 10.1097/JU.0000000000000312. Epub 2019 Aug 8. J Urol. 2019. PMID: 31039100
-
Effect of Bladder Neck Preservation on Long-Term Urinary Continence after Robot-Assisted Laparoscopic Prostatectomy: A Systematic Review and Meta-Analysis.J Clin Med. 2019 Nov 24;8(12):2068. doi: 10.3390/jcm8122068. J Clin Med. 2019. PMID: 31771310 Free PMC article. Review.
Cited by
-
Clinicopathological Significances of Positive Surgical Resection Margin after Radical Prostatectomy for Prostatic Cancers: A Meta-Analysis.Medicina (Kaunas). 2022 Sep 9;58(9):1251. doi: 10.3390/medicina58091251. Medicina (Kaunas). 2022. PMID: 36143928 Free PMC article. Review.
-
Anatomical, surgical and technical factors influencing continence after radical prostatectomy.Ther Adv Urol. 2019 Jan 8;11:1756287218813787. doi: 10.1177/1756287218813787. eCollection 2019 Jan-Dec. Ther Adv Urol. 2019. PMID: 30671134 Free PMC article. Review.
-
Effects of bladder neck sparing on continence outcomes of robotic-assisted radical prostatectomy: a systemic review and metaanalysis.Prostate Int. 2024 Dec;12(4):179-185. doi: 10.1016/j.prnil.2024.04.004. Epub 2024 Apr 29. Prostate Int. 2024. PMID: 39735194 Free PMC article. Review.
-
Bladder neck preservation improves time to continence after radical prostatectomy: a systematic review and meta-analysis.Oncotarget. 2016 Oct 11;7(41):67463-67475. doi: 10.18632/oncotarget.11997. Oncotarget. 2016. PMID: 27634899 Free PMC article.
-
Laparoscopic urinary bladder diverticulectomy combined with photoselective vaporisation of the prostate.Wideochir Inne Tech Maloinwazyjne. 2015 Apr;10(1):62-7. doi: 10.5114/wiitm.2015.49671. Epub 2015 Mar 10. Wideochir Inne Tech Maloinwazyjne. 2015. PMID: 25960795 Free PMC article.
References
-
- Heidenreich A, Bastian PJ, Bellmunt J, et al. EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent-update 2013. Eur Urol. 2014;65:124–37. - PubMed
-
- Phillips R. Prostate cancer: post-treatment complications of radiotherapy and prostatectomy. Nat Rev Urol. 2014;11:129. - PubMed
-
- Sacco E, Prayer-Galetti T, Pinto F, et al. Urinary incontinence after radical prostatectomy: incidence by definition, risk factors and temporal trend in a large series with a long-term follow-up. BJU Int. 2006;97:1234–41. - PubMed
-
- Young MD, Weizer AZ, Silverstein AD, et al. Urinary continence and quality of life in the first year after radical perineal prostatectomy. J Urol. 2003;170:2374–8. - PubMed
-
- Froehner M, Koch R, Leike S, et al. Urinary tract-related quality of life after radical prostatectomy: open retropubic versus robot-assisted laparoscopic approach. Urol Int. 2013;90:36–40. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous
