Contemporary surgical management of rectovaginal fistula in Crohn's disease
- PMID: 25400993
- PMCID: PMC4231514
- DOI: 10.4291/wjgp.v5.i4.487
Contemporary surgical management of rectovaginal fistula in Crohn's disease
Abstract
Rectovaginal fistula is a disastrous complication of Crohn's disease (CD) that is exceedingly difficult to treat. It is a disabling condition that negatively impacts a women's quality of life. Successful management is possible only after accurate and complete assessment of the entire gastrointestinal tract has been performed. Current treatment algorithms range from observation to medical management to the need for surgical intervention. A wide variety of success rates have been reported for all management options. The choice of surgical repair methods depends on various fistula and patient characteristics. Before treatment is undertaken, establishing reasonable goals and expectations of therapy is essential for both the patient and surgeon. This article aims to highlight the various surgical techniques and their outcomes for repair of CD associated rectovaginal fistula.
Keywords: Advancement flap; Crohn’s disease; Episioproctotomy; Fistula; Rectovaginal fistula; Sleeve advancement.
Figures


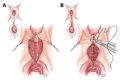
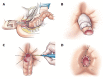
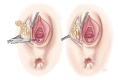
References
-
- Crohn BB, Ginzburg L, Oppenheimer GD. Landmark article Oct 15, 1932. Regional ileitis. A pathological and clinical entity. By Burril B. Crohn, Leon Ginzburg, and Gordon D. Oppenheimer. JAMA. 1984;251:73–79. - PubMed
-
- Hannaway CD, Hull TL. Current considerations in the management of rectovaginal fistula from Crohn’s disease. Colorectal Dis. 2008;10:747–755; discussion 755-756. - PubMed
-
- Radcliffe AG, Ritchie JK, Hawley PR, Lennard-Jones JE, Northover JM. Anovaginal and rectovaginal fistulas in Crohn’s disease. Dis Colon Rectum. 1988;31:94–99. - PubMed
-
- Heyen F, Winslet MC, Andrews H, Alexander-Williams J, Keighley MR. Vaginal fistulas in Crohn’s disease. Dis Colon Rectum. 1989;32:379–383. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

