12-month outcomes of community engagement versus technical assistance to implement depression collaborative care: a partnered, cluster, randomized, comparative effectiveness trial
- PMID: 25402400
- PMCID: PMC4235578
- DOI: 10.7326/M13-3011
12-month outcomes of community engagement versus technical assistance to implement depression collaborative care: a partnered, cluster, randomized, comparative effectiveness trial
Abstract
Background: Depression collaborative care implementation using community engagement and planning (CEP) across programs improves 6-month client outcomes in minority communities, compared with technical assistance to individual programs (resources for services [RS]). However, 12-month outcomes are unknown.
Objective: To compare effects of CEP and RS on mental health-related quality of life (MHRQL) and use of services among depressed clients at 12 months.
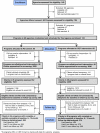
Design: Matched health and community programs (n = 93) in 2 communities randomly assigned to receive CEP or RS. (ClinicalTrials.gov: NCT01699789).
Measurements: Self-reported MHRQL and services use at baseline, 6 months, and 12 months.
Setting: Los Angeles, California.
Patients: 1018 adults with depressive symptoms (8-item Patient Health Questionnaire score ≥10), 88% of whom were an ethnic minority.
Intervention: CEP and RS to implement depression collaborative care.
Measurements: The primary outcome was poor MHRQL (12-item mental health composite score ≤40) at baseline, 6 months, and 12 months; the secondary outcome was use of services at 12 months.
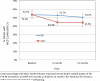
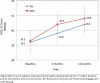
Results: At 6 months, the finding that CEP outperformed RS to reduce poor MHRQL was significant but sensitive to underlying statistical assumptions. At 12 months, some analyses suggested that CEP was advantageous to MHRQL, whereas others did not confirm a significant difference favoring CEP. The finding that CEP reduced behavioral health hospitalizations at 6 months was less evident at 12 months and was sensitive to underlying statistical assumptions. Other services use did not significantly differ between interventions at 12 months.
Limitation: Data are self-reported, and findings are sensitive to modeling assumptions.
Conclusion: In contrast to 6-month results, no consistent effects of CEP on reducing the likelihood of poor MHRQL and behavioral health hospitalizations were found at 12 months. Still, given the needs of underresourced communities, the favorable profile of CEP, and the lack of evidence-based alternatives, CEP remains a viable strategy for policymakers and communities to consider.
Primary funding source: National Institute of Mental Health, Robert Wood Johnson Foundation, California Community Foundation, National Library of Medicine, and National Institutes of Health/National Center for Advancing Translational Science for the UCLA Clinical and Translational Science Institute.
Figures

References
-
- Insel TR, Charney DS. Research on major depression. JAMA. 2003;289(23):3167–3168. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
