Tissue Reinforcement in Implant-based Breast Reconstruction
- PMID: 25426375
- PMCID: PMC4236353
- DOI: 10.1097/GOX.0000000000000140
Tissue Reinforcement in Implant-based Breast Reconstruction
Abstract
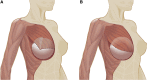
Background: Tissue reinforcement with allogeneic or xenogeneic acellular dermal matrices (ADMs) is increasingly used in single-stage (direct-to-implant) and 2-stage implant-based breast reconstruction following mastectomy. ADMs allow surgeons to control implant position and obviate the need for submuscular implant placement. Here, we review the benefits and risks of using ADMs in implant-based breast reconstruction based on available data.
Methods: A comprehensive analysis of the literature with focus on recent publications was performed. Additional information regarding the proper use of ADMs was based on our institutional experience.
Results: ADM use may improve definition of the lateral confines of the breast and lower pole projection. It may facilitate direct-to-implant procedures and improve aesthetic outcomes. The effect of ADMs on complication rates remains controversial. Known patient risk factors such as obesity, smoking, and radiotherapy should be considered during patient selection. For patients with healthy, well-vascularized skin envelopes, ADM-assisted direct-to- implant reconstruction is a safe and cost-effective alternative to 2-stage implant reconstruction, with low complication rates. ADMs may be used to treat capsular contracture, and limited available data further suggest the possibility that ADMs may reduce the risk of capsular contracture. Novel synthetic or biosynthetic tissue reinforcement devices with different physical and ease-of-use properties than ADMs are emerging options for reconstructive surgeons and patients who seek to avoid tissue products from human or mammalian cadavers.
Conclusions: ADM-assisted implant-based breast reconstruction may improve aesthetic outcomes. However, appropriate patient selection, surgical technique, and postoperative management are critical for its success, including minimizing the risk of complications.
Conflict of interest statement
Disclosure: Medical writing support for this manuscript was funded by Allergan, Inc. Dr. Scheflan serves as a consultant for Allergan, Inc., and a clinical investigator for TEI Biosciences Inc. Dr. Colwell is a consultant for Allergan, Inc. and LifeCell Corp. The Article Processing Charge was paid for by Allergan, Inc.
Figures

References
-
- Atisha D, Alderman AK, Lowery JC, et al. Prospective analysis of long-term psychosocial outcomes in breast reconstruction: two-year postoperative results from the Michigan Breast Reconstruction Outcomes Study. Ann Surg. 2008;247:1019–1028. - PubMed
-
- Roostaeian J, Crisera C. Current options in breast reconstruction with or without radiotherapy. Curr Opin Obstet Gynecol. 2011;23:44–50. - PubMed
-
- Yueh JH, Slavin SA, Adesiyun T, et al. Patient satisfaction in postmastectomy breast reconstruction: a comparative evaluation of DIEP, TRAM, latissimus flap, and implant techniques. Plast Reconstr Surg. 2010;125:1585–1595. - PubMed
-
- Christensen BO, Overgaard J, Kettner LO, et al. Long-term evaluation of postmastectomy breast reconstruction. Acta Oncol. 2011;50:1053–1061. - PubMed
-
- American Society of Plastic Surgeons. 2012 Plastic Surgery Statistics Report. Available at: http://www.plasticsurgery.org/Documents/news-resources/statistics/2012-P.... Accessed October 31, 2013.
LinkOut - more resources
Full Text Sources
Other Literature Sources
