Conducting Retrospective Ontological Clinical Trials in ICD-9-CM in the Age of ICD-10-CM
- PMID: 25452683
- PMCID: PMC4226400
- DOI: 10.4137/CIN.S14032
Conducting Retrospective Ontological Clinical Trials in ICD-9-CM in the Age of ICD-10-CM
Abstract
Objective: To quantify the impact of International Classification of Disease 10th Revision Clinical Modification (ICD-10-CM) transition in cancer clinical trials by comparing coding accuracy and data discontinuity in backward ICD-10-CM to ICD-9-CM mapping via two tools, and to develop a standard ICD-9-CM and ICD-10-CM bridging methodology for retrospective analyses.
Background: While the transition to ICD-10-CM has been delayed until October 2015, its impact on cancer-related studies utilizing ICD-9-CM diagnoses has been inadequately explored.
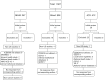
Materials and methods: Three high impact journals with broad national and international readerships were reviewed for cancer-related studies utilizing ICD-9-CM diagnoses codes in study design, methods, or results. Forward ICD-9-CM to ICD-10-CM mapping was performing using a translational methodology with the Motif web portal ICD-9-CM conversion tool. Backward mapping from ICD-10-CM to ICD-9-CM was performed using both Centers for Medicare and Medicaid Services (CMS) general equivalence mappings (GEMs) files and the Motif web portal tool. Generated ICD-9-CM codes were compared with the original ICD-9-CM codes to assess data accuracy and discontinuity.
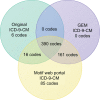
Results: While both methods yielded additional ICD-9-CM codes, the CMS GEMs method provided incomplete coverage with 16 of the original ICD-9-CM codes missing, whereas the Motif web portal method provided complete coverage. Of these 16 codes, 12 ICD-9-CM codes were present in 2010 Illinois Medicaid data, and accounted for 0.52% of patient encounters and 0.35% of total Medicaid reimbursements. Extraneous ICD-9-CM codes from both methods (Centers for Medicare and Medicaid Services general equivalent mapping [CMS GEMs, n = 161; Motif web portal, n = 246]) in excess of original ICD-9-CM codes accounted for 2.1% and 2.3% of total patient encounters and 3.4% and 4.1% of total Medicaid reimbursements from the 2010 Illinois Medicare database.
Discussion: Longitudinal data analyses post-ICD-10-CM transition will require backward ICD-10-CM to ICD-9-CM coding, and data comparison for accuracy. Researchers must be aware that all methods for backward coding are not comparable in yielding original ICD-9-CM codes.
Conclusions: The mandated delay is an opportunity for organizations to better understand areas of financial risk with regards to data management via backward coding. Our methodology is relevant for all healthcare-related coding data, and can be replicated by organizations as a strategy to mitigate financial risk.
Keywords: ICD-9-CM; cancer informatics infrastructure; cancer research; clinical trials.
Figures
References
-
- Office of the Secretary HHS Administrative simplification: adoption of a standard for a unique health plan identifier; addition to the National Provider Identifier requirements; and a change to the compliance date for the International Classification of Diseases, 10th Edition (ICD-10-CM and ICD-10-PCS) medical data code sets. Final rule. Fed Regist. 2012;77:54663–720. - PubMed
-
- Official CMS Industry Resources for the ICD-10 Transition. 2014. [Accessed May 18, 2014]. Available at http://www.cms.gov/Medicare/Coding/ICD10/index.html?redirect=/icd10.
-
- Carlson J, Conn J, Robeznieks A. Bruised by ICD-10 delay, healthcare execs huddle over what to do next. Mod Healthc. 2014;44:8–9. - PubMed
-
- Behavioral Healthcare . ICD- 10: The Good, the Bad, and the Advice. Behavioral Healthcare; May 15, 2014. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

