Regulation of coronary blood flow in health and ischemic heart disease
- PMID: 25475073
- PMCID: PMC5856234
- DOI: 10.1016/j.pcad.2014.12.002
Regulation of coronary blood flow in health and ischemic heart disease
Abstract
The major factors determining myocardial perfusion and oxygen delivery have been elucidated over the past several decades, and this knowledge has been incorporated into the management of patients with ischemic heart disease (IHD). The basic understanding of the fluid mechanical behavior of coronary stenoses has also been translated to the cardiac catheterization laboratory where measurements of coronary pressure distal to a stenosis and coronary flow are routinely obtained. However, the role of perturbations in coronary microvascular structure and function, due to myocardial hypertrophy or coronary microvascular dysfunction, in IHD is becoming increasingly recognized. Future studies should therefore be aimed at further improving our understanding of the integrated coronary microvascular mechanisms that control coronary blood flow, and of the underlying causes and mechanisms of coronary microvascular dysfunction. This knowledge will be essential to further improve the treatment of patients with IHD.
Keywords: Coronary artery disease; Coronary blood flow; Hypertrophy; Ischemic heart disease; Microvascular dysfunction.
Copyright © 2014 Elsevier Inc. All rights reserved.
Conflict of interest statement
Statement of Conflict of Interest: There are no conflicts of interest to declare for any of the authors.
Figures
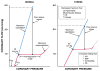
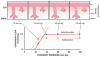

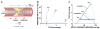

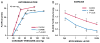

References
-
- Hoffman JIE. Transmural myocardial perfusion. Prog Cardiovasc Dis. 1987;29:429–464. - PubMed
-
- Tomanek RJ. Coronary Vasculature: Development, Structure-Function, and Adaptations. New York: Springer; 2013.
-
- Tune JD. Morgan & Claypool Life Sciences. 2014. Coronary circulation.
-
- Duncker DJ, Bache RJ. Regulation of coronary vasomotor tone under normal conditions and during acute myocardial hypoperfusion. Pharmacol Ther. 2000;86:87–110. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

