Percutaneous and surgical tracheostomy in critically ill adult patients: a meta-analysis
- PMID: 25526983
- PMCID: PMC4293819
- DOI: 10.1186/s13054-014-0544-7
Percutaneous and surgical tracheostomy in critically ill adult patients: a meta-analysis
Abstract
Introduction: The aim of this study was to conduct a meta-analysis to determine whether percutaneous tracheostomy (PT) techniques are advantageous over surgical tracheostomy (ST), and if one PT technique is superior to the others.
Methods: Computerized databases (1966 to 2013) were searched for randomized controlled trials (RCTs) reporting complications as predefined endpoints and comparing PT and ST and among the different PT techniques in mechanically ventilated adult critically ill patients. Odds ratios (OR) and mean differences (MD) with 95% confidence interval (CI), and I(2) values were estimated.
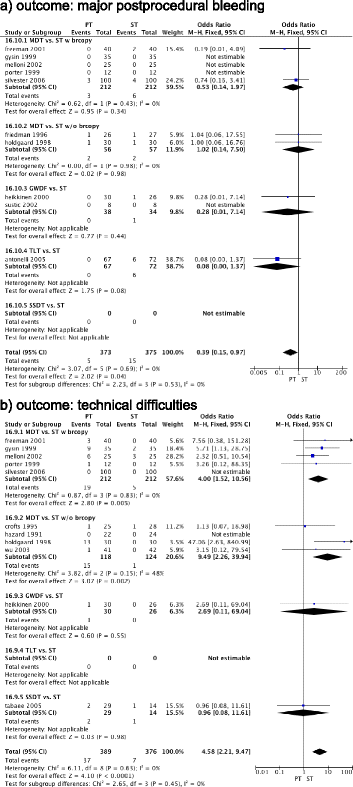
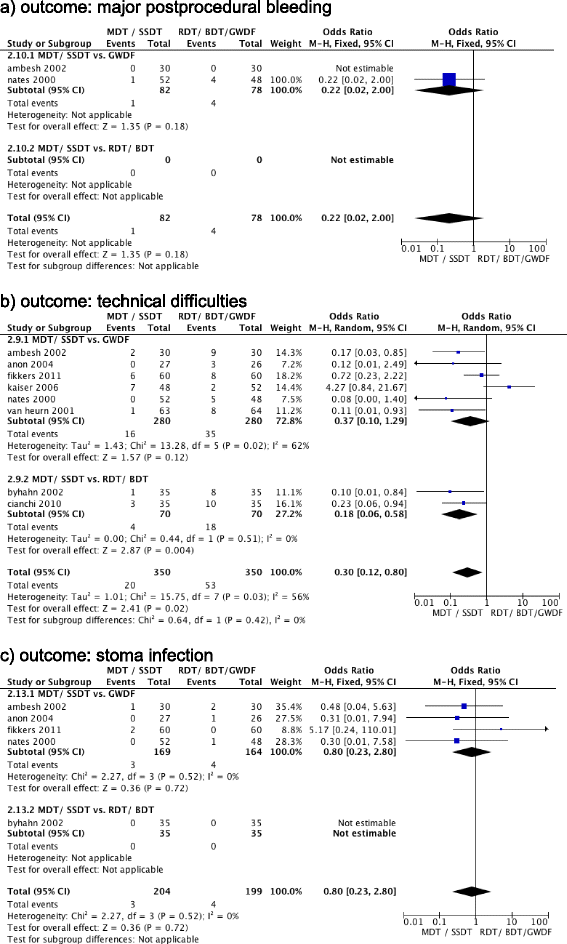
Results: Fourteen RCTs tested PT techniques versus ST in 973 patients. PT techniques were performed faster (MD, -13.06 minutes (95% CI, -19.37 to -6.76 (P < 0.0001)); I(2) = 97% (P < 0.00001)) and reduced odds for stoma inflammation (OR, 0.38 (95% CI, 0.19 to 0.76 (P = 0.006)); I(2) = 2% (P = 0.36)), and infection (OR, 0.22 (95% CI, 0.11 to 0.41 (P < 0.00001)); I(2) = 0% (P = 0.54)), but increased odds for procedural technical difficulties (OR, 4.58 (95% CI, 2.21 to 9.47 (P < 0.0001)); I(2) = 0% (P = 0.63)). PT techniques reduced odds for postprocedural major bleeding (OR, 0.39 (95% CI, 0.15 to 0.97 (P = 0.04)); I(2) = 0% (P = 0.69)), but not when a single RCT using translaryngeal tracheostomy was excluded (OR, 0.58 (95% CI, 0.21 to 1.63 (P = 0.30)); I(2) = 0% (P = 0.89)). Eight RCTs compared different PT techniques in 700 patients. Multiple (MDT) and single step (SSDT) dilatator techniques are associated with the lowest odds for difficult dilatation or cannula insertion (OR, 0.30 (95% CI, 0.12 to 0.80 (P = .02)); I(2) = 56% (P = 0.03)) and major intraprocedural bleeding (OR, 0.29 (95% CI, 0.10 to 0.85 (P = 0.02)); I(2) = 0% (P = 0.72)), compared to the guide wire dilatation forceps technique.
Conclusion: In critically ill adult patients, PT techniques can be performed faster and reduce stoma inflammation and infection but are associated with increased technical difficulties when compared to ST. Among PT techniques, MDT and SSDT were associated with the lowest intraprocedural risks and seem to be preferable.
Figures


References
-
- Carrer S, Basilico S, Rossi S, Bosu A, Bernorio S, Vaghi GM. Outcomes of percutaneous tracheostomy. Minerva Anestesiol. 2009;75:607–615. - PubMed
-
- Guarino A. Percutaneous tracheostomy: patient outcomes. It is always time to improve our care. Minerva Anestesiol. 2009;75:602–603. - PubMed
-
- Arabi YM, Alhashemi JA, Tamim HM, Esteban A, Haddad SH, Dawood A, Shirawi N, Alshimemeri AA. The impact of time to tracheostomy on mechanical ventilation duration, length of stay, and mortality in intensive care unit patients. J Crit Care. 2009;24:435–440. doi: 10.1016/j.jcrc.2008.07.001. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

