Non-union rate with stand-alone lateral lumbar interbody fusion
- PMID: 25546670
- PMCID: PMC4602616
- DOI: 10.1097/MD.0000000000000275
Non-union rate with stand-alone lateral lumbar interbody fusion
Abstract
Retrospective radiographic analysis.To determine the fusion rate of stand-alone lateral lumbar interbody fusion (LLIF). Biomechanical studies have indicated that LLIF may be more stable than anterior or transforaminal lumbar interbody fusion. Early clinical reports of stand-alone LLIF have shown success in obtaining fusion and indirectly decompressing nerve roots. A consecutive case series of stand-alone LLIF was analyzed with chart and radiographic review. Non-union was determined by symptomatology consistent with non-union and absence of bridging bone on the CT scan. Thirty-nine levels of stand alone LLIF were performed in 23 patients. Eleven patients received 1-level surgery, 7 patients received 2-level surgery, 3 patients received 3-level surgery, and 1 patient received 4-level surgery. Excluding 1 infected case, we analyzed 37 levels of stand alone LLIF in 22 patients. Non-union incidence was 7 levels in 6 patients. Non-union rate was 7/37 (19%) per level and 6/22 (27%) per patient. While our study population was relatively low, a non-union rate of 19% to 27% is concerning for modern spine surgery. Currently in our practice, we occasionally still perform stand-alone LLIF utilizing 22 mm wide grafts in low-demand levels in non-smoking and non-osteoporotic patients. However, in a majority of patients, we provide supplemental fixation: bilateral pedicle screws in most patients and unilateral pedicle screws or spinous process plates in some patients.
Conflict of interest statement
Author A is a paid consultant for RTI, Medtronic, Aesculap, Brainlab, and Amedica; he has development/royalty agreements with RTI and Amedica; is a paid director of the Marina Spine Center. Author C is a paid consultant for RTI, Aesculap, and Amedica; he has development/royalty agreements with RTI, Medtronic, and Amedica; is a paid director of the Marina Spine Center. Author B has no possible conflicts of interest.
Figures
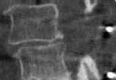
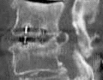
Similar articles
-
Biomechanical evaluation of lateral lumbar interbody fusion with secondary augmentation.J Neurosurg Spine. 2016 Dec;25(6):720-726. doi: 10.3171/2016.4.SPINE151386. Epub 2016 Jul 8. J Neurosurg Spine. 2016. PMID: 27391398
-
Biomechanical Stability Afforded by Unilateral Versus Bilateral Pedicle Screw Fixation with and without Interbody Support Using Lateral Lumbar Interbody Fusion.World Neurosurg. 2018 May;113:e439-e445. doi: 10.1016/j.wneu.2018.02.053. Epub 2018 Feb 17. World Neurosurg. 2018. PMID: 29462730
-
Biomechanical analysis of an expandable lateral cage and a static transforaminal lumbar interbody fusion cage with posterior instrumentation in an in vitro spondylolisthesis model.J Neurosurg Spine. 2016 Jan;24(1):32-8. doi: 10.3171/2015.4.SPINE14636. Epub 2015 Sep 18. J Neurosurg Spine. 2016. PMID: 26384133
-
Is instrumented lateral lumbar interbody fusion superior to stand-alone lateral lumbar interbody fusion for the treatment of lumbar degenerative disease? A meta-analysis.J Clin Neurosci. 2021 Oct;92:136-146. doi: 10.1016/j.jocn.2021.08.002. Epub 2021 Aug 14. J Clin Neurosci. 2021. PMID: 34509241 Review.
-
Fusion rate for stand-alone lateral lumbar interbody fusion: a systematic review.Spine J. 2020 Nov;20(11):1816-1825. doi: 10.1016/j.spinee.2020.06.006. Epub 2020 Jun 11. Spine J. 2020. PMID: 32535072
Cited by
-
Three- and 4-Level Lumbar Arthrodesis Using Adjunctive Pulsed Electromagnetic Field Stimulation: A Multicenter Retrospective Evaluation of Fusion Rates and a Review of the Literature.Int J Spine Surg. 2021 Apr;15(2):228-233. doi: 10.14444/8031. Epub 2021 Mar 23. Int J Spine Surg. 2021. PMID: 33900979 Free PMC article.
-
When to Consider Stand-Alone Lateral Lumbar Interbody Fusion: Is There a Role for a Comeback With New Implants?Int J Spine Surg. 2022 Apr;16(S1):S69-S75. doi: 10.14444/8238. Int J Spine Surg. 2022. PMID: 35387891 Free PMC article.
-
Textile Design of an Intervertebral Disc Replacement Device from Silk Yarn.Biomimetics (Basel). 2023 Apr 12;8(2):152. doi: 10.3390/biomimetics8020152. Biomimetics (Basel). 2023. PMID: 37092404 Free PMC article.
-
Lateral Lumbar Interbody Fusion and in Situ Screw Fixation for Rostral Adjacent Segment Stenosis of the Lumbar Spine.J Korean Neurosurg Soc. 2017 Nov;60(6):755-762. doi: 10.3340/jkns.2017.0606.003. Epub 2017 Oct 25. J Korean Neurosurg Soc. 2017. PMID: 29142637 Free PMC article.
-
Inhibition of the extracellular signal-regulated kinase pathway reduces the inflammatory component in nucleus pulposus cells.J Orthop Res. 2022 Oct;40(10):2362-2371. doi: 10.1002/jor.25273. Epub 2022 Feb 1. J Orthop Res. 2022. PMID: 35106811 Free PMC article.
References
-
- Hsieh P, Koski T, O'Shaughnessy B, et al. Anterior lumbar interbody fusion in comparison with transforaminal lumber interbody fusion: implications for the restoration of foraminal height, local disc angle, lumbar lordosis, and sagittal balance. J Neurosurg Spine 2007; 7:379–386. - PubMed
-
- Watkins RG, IV, Hanna R, Chang D, Watkins RG., III Sagital alignment after lumbar interbody fusions: comparing anterior, lateral and transforaminal approaches. J Spinal Disord Tech 2014; 27:253–256. - PubMed
-
- Simmonds MC, Brown JV, Heirs MK, et al. Safety and effectiveness of recombinant human bone morphogenetic protein-2 for spinal fusion: a meta-analysis of individual-participant data. Ann Intern Med 2013; 158:877–889. - PubMed
-
- Kepler CK, Sharma AK, Huang RC, et al. Indirect foraminal decompression after lateral transpsoas interbody fusion. J Neurosurg Spine 2012; 16:329–333. - PubMed
-
- Elowitz EH, Yanni DS, Chwajol M, et al. Evaluation of indirect decompression of the lumbar spinal canal following minimally invasive lateral transpsoas interbody fusion: radiographic and outcome analysis. Minim Invas Neurosurg 2011; 54:201–206. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

