Acute nicotine administration increases BOLD fMRI signal in brain regions involved in reward signaling and compulsive drug intake in rats
- PMID: 25552431
- PMCID: PMC4368882
- DOI: 10.1093/ijnp/pyu011
Acute nicotine administration increases BOLD fMRI signal in brain regions involved in reward signaling and compulsive drug intake in rats
Erratum in
-
Erratum.Int J Neuropsychopharmacol. 2016 Apr 27;19(10):pyw031. doi: 10.1093/ijnp/pyw031. Int J Neuropsychopharmacol. 2016. PMID: 27207904 Free PMC article. No abstract available.
Abstract
Background: Acute nicotine administration potentiates brain reward function and enhances motor and cognitive function. These studies investigated which brain areas are being activated by a wide range of doses of nicotine, and if this is diminished by pretreatment with the nonselective nicotinic receptor antagonist mecamylamine.
Methods: Drug-induced changes in brain activity were assessed by measuring changes in the blood oxygen level dependent (BOLD) signal using an 11.1-Tesla magnetic resonance scanner. In the first experiment, nicotine naïve rats were mildly anesthetized and the effect of nicotine (0.03-0.6 mg/kg) on the BOLD signal was investigated for 10 min. In the second experiment, the effect of mecamylamine on nicotine-induced brain activity was investigated.
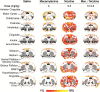
Results: A high dose of nicotine increased the BOLD signal in brain areas implicated in reward signaling, such as the nucleus accumbens shell and the prelimbic area. Nicotine also induced a dose-dependent increase in the BOLD signal in the striato-thalamo-orbitofrontal circuit, which plays a role in compulsive drug intake, and in the insular cortex, which contributes to nicotine craving and relapse. In addition, nicotine induced a large increase in the BOLD signal in motor and somatosensory cortices. Mecamylamine alone did not affect the BOLD signal in most brain areas, but induced a negative BOLD response in cortical areas, including insular, motor, and somatosensory cortices. Pretreatment with mecamylamine completely blocked the nicotine-induced increase in the BOLD signal.
Conclusions: These studies demonstrate that acute nicotine administration activates brain areas that play a role in reward signaling, compulsive behavior, and motor and cognitive function.
Keywords: addiction; compulsive behavior; nicotine; pharmacological fMRI; rats; reward..
© The Author 2014. Published by Oxford University Press on behalf of CINP.
Figures




Similar articles
-
Brain nicotinic acetylcholine receptors are involved in stress-induced potentiation of nicotine reward in rats.J Psychopharmacol. 2017 Jul;31(7):945-955. doi: 10.1177/0269881117707745. Epub 2017 May 25. J Psychopharmacol. 2017. PMID: 28541827
-
Blockade of CRF1 receptors in the central nucleus of the amygdala attenuates the dysphoria associated with nicotine withdrawal in rats.Pharmacol Biochem Behav. 2012 Mar;101(1):62-8. doi: 10.1016/j.pbb.2011.12.001. Epub 2011 Dec 9. Pharmacol Biochem Behav. 2012. PMID: 22182462 Free PMC article.
-
Nicotinic receptor modulation of the default mode network.Psychopharmacology (Berl). 2021 Feb;238(2):589-597. doi: 10.1007/s00213-020-05711-9. Epub 2020 Nov 20. Psychopharmacology (Berl). 2021. PMID: 33216167 Free PMC article.
-
Functional brain imaging of nicotinic effects on higher cognitive processes.Biochem Pharmacol. 2011 Oct 15;82(8):943-51. doi: 10.1016/j.bcp.2011.06.008. Epub 2011 Jun 13. Biochem Pharmacol. 2011. PMID: 21684262 Free PMC article. Review.
-
Targeting neuronal dysfunction in schizophrenia with nicotine: Evidence from neurophysiology to neuroimaging.J Psychopharmacol. 2017 Jul;31(7):801-811. doi: 10.1177/0269881117705071. Epub 2017 Apr 26. J Psychopharmacol. 2017. PMID: 28441884 Free PMC article. Review.
Cited by
-
Acute nicotine treatment enhances compulsive-like remifentanil self-administration that persists despite contextual punishment.Addict Biol. 2022 May;27(3):e13170. doi: 10.1111/adb.13170. Addict Biol. 2022. PMID: 35470562 Free PMC article.
-
Neural and behavioural changes in male periadolescent mice after prolonged nicotine-MDMA treatment.Metab Brain Dis. 2016 Feb;31(1):93-107. doi: 10.1007/s11011-015-9691-z. Epub 2015 Jun 20. Metab Brain Dis. 2016. PMID: 26088184
-
Relationship between carotid intima-media thickness (cIMT) and dual-system imbalance in tobacco dependence: An rs-fMRI research.Brain Behav. 2023 Jul;13(7):e3059. doi: 10.1002/brb3.3059. Epub 2023 Jun 12. Brain Behav. 2023. PMID: 37309087 Free PMC article.
-
The acute and repeated effects of cigarette smoking and smoking-related cues on impulsivity.Drug Alcohol Rev. 2021 Jul;40(5):864-868. doi: 10.1111/dar.13206. Epub 2020 Nov 2. Drug Alcohol Rev. 2021. PMID: 33140460 Free PMC article.
-
Addiction-related brain networks identification via Graph Diffusion Reconstruction Network.Brain Inform. 2024 Jan 8;11(1):1. doi: 10.1186/s40708-023-00216-5. Brain Inform. 2024. PMID: 38190053 Free PMC article.
References
-
- Balleine BW, Killcross S. (2006). Parallel incentive processing: an integrated view of amygdala function. Trends Neurosci 29:272–279. - PubMed
-
- Baxter LR, Jr., Phelps ME, Mazziotta JC, Guze BH, Schwartz JM, Selin CE. (1987). Local cerebral glucose metabolic rates in obsessive-compulsive disorder. A comparison with rates in unipolar depression and in normal controls. Arch Gen Psychiatry 44:211–218. - PubMed
-
- Benowitz NL. (1988). Drug therapy. Pharmacologic aspects of cigarette smoking and nicotine addition. N Engl J Med 319:1318–1330. - PubMed
-
- Bruijnzeel AW, Zislis G, Wilson C, Gold MS. (2007). Antagonism of CRF receptors prevents the deficit in brain reward function associated with precipitated nicotine withdrawal in rats. Neuropsychopharmacology 32:955–963. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

