Association between respiratory syncytial virus activity and pneumococcal disease in infants: a time series analysis of US hospitalization data
- PMID: 25562317
- PMCID: PMC4285401
- DOI: 10.1371/journal.pmed.1001776
Association between respiratory syncytial virus activity and pneumococcal disease in infants: a time series analysis of US hospitalization data
Abstract
Background: The importance of bacterial infections following respiratory syncytial virus (RSV) remains unclear. We evaluated whether variations in RSV epidemic timing and magnitude are associated with variations in pneumococcal disease epidemics and whether changes in pneumococcal disease following the introduction of seven-valent pneumococcal conjugate vaccine (PCV7) were associated with changes in the rate of hospitalizations coded as RSV.
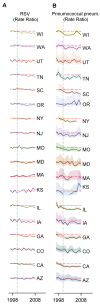
Methods and findings: We used data from the State Inpatient Databases (Agency for Healthcare Research and Quality), including >700,000 RSV hospitalizations and >16,000 pneumococcal pneumonia hospitalizations in 36 states (1992/1993-2008/2009). Harmonic regression was used to estimate the timing of the average seasonal peak of RSV, pneumococcal pneumonia, and pneumococcal septicemia. We then estimated the association between the incidence of pneumococcal disease in children and the activity of RSV and influenza (where there is a well-established association) using Poisson regression models that controlled for shared seasonal variations. Finally, we estimated changes in the rate of hospitalizations coded as RSV following the introduction of PCV7. RSV and pneumococcal pneumonia shared a distinctive spatiotemporal pattern (correlation of peak timing: ρ = 0.70, 95% CI: 0.45, 0.84). RSV was associated with a significant increase in the incidence of pneumococcal pneumonia in children aged <1 y (attributable percent [AP]: 20.3%, 95% CI: 17.4%, 25.1%) and among children aged 1-2 y (AP: 10.1%, 95% CI: 7.6%, 13.9%). Influenza was also associated with an increase in pneumococcal pneumonia among children aged 1-2 y (AP: 3.2%, 95% CI: 1.7%, 4.7%). Finally, we observed a significant decline in RSV-coded hospitalizations in children aged <1 y following PCV7 introduction (-18.0%, 95% CI: -22.6%, -13.1%, for 2004/2005-2008/2009 versus 1997/1998-1999/2000). This study used aggregated hospitalization data, and studies with individual-level, laboratory-confirmed data could help to confirm these findings.
Conclusions: These analyses provide evidence for an interaction between RSV and pneumococcal pneumonia. Future work should evaluate whether treatment for secondary bacterial infections could be considered for pneumonia cases even if a child tests positive for RSV. Please see later in the article for the Editors' Summary.
Conflict of interest statement
DMW has received research support for other projects from an investigator initiated research grant from Pfizer to Yale University. LS and KPK have previously received research support from Pfizer. DMW has received consulting fees from Merck. KPK is a member of the Editorial Board of
Figures




References
-
- Madhi S, Petersen K, Madhi A, Wasas A, Klugman K (2000) Impact of human immunodeficiency virus type 1 on the disease spectrum of Streptococcus pneumoniae in South African children. Pediatr Infect Dis J 19: 1141–1147. - PubMed
-
- Diavatopoulos DA, Short KR, Price JT, Wilksch JJ, Brown LE, et al. (2010) Influenza A virus facilitates Streptococcus pneumoniae transmission and disease. FASEB J 24: 1789–1798. - PubMed
-
- Talbot T, Poehling K, Hartert T, Arbogast P, Halasa N, et al. (2005) Seasonality of invasive pneumococcal disease: temporal relation to documented influenza and respiratory syncytial viral circulation. Am J Med 118: 285–291. - PubMed
-
- Techasaensiri B, Techasaensiri C, Mejías A, McCracken GH Jr, Ramilo O (2010) Viral coinfections in children with invasive pneumococcal disease. Pediatr Infect Dis J 29: 519–523. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

