Functional capacity of reconstituted blood in 1:1:1 versus 3:1:1 ratios: a thrombelastometry study
- PMID: 25571924
- PMCID: PMC4296528
- DOI: 10.1186/s13049-014-0080-0
Functional capacity of reconstituted blood in 1:1:1 versus 3:1:1 ratios: a thrombelastometry study
Abstract
Introduction: Different transfusion ratio concepts of packed red blood cells (pRBCs), fresh frozen plasma (FFP) and platelets (PLTs) have been implemented in trauma care, but the optimal ratios are still discussed. In this study the hemostatic potential of two predefined ratios was assessed by using an in vitro thrombelastometric approach. Furthermore, age effects of reconstituted blood were analyzed.
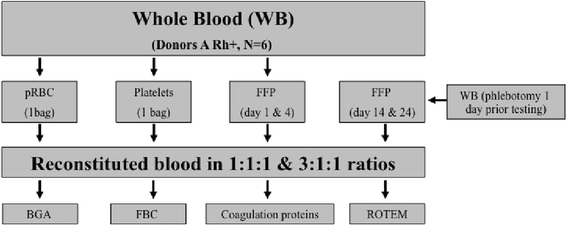
Methods: Whole blood (WB) of voluntary donors was separated into pRBCs, FFP and PLTs and reconstituted into the ratios 1:1:1 and 3:1:1 at day 1, 4, 14, and 24. Standard blood count, electrolytes and coagulation proteins were quantified. The functional coagulation in ratio- and age-specific groups was evaluated using rotational thromboelastometry (ROTEM).
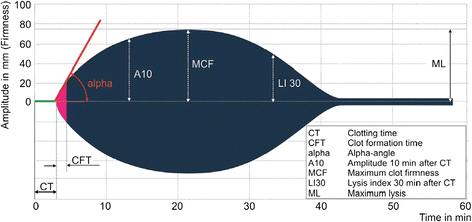
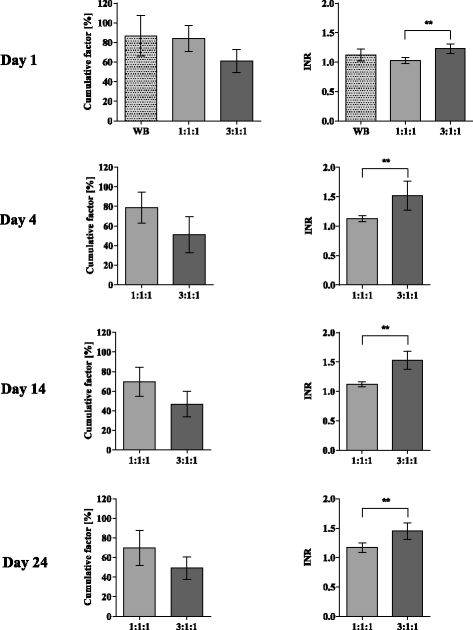
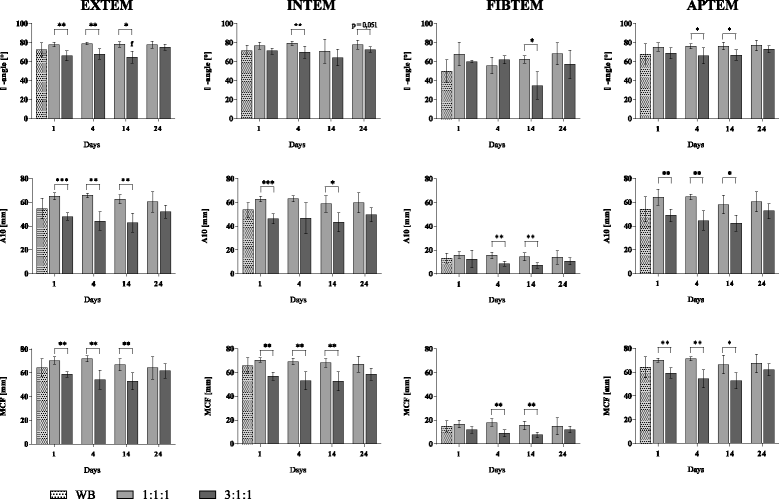
Results: Several coagulation factors reduced significantly in the 3:1:1 ratio and were consistent with increased INR, decelerated clot formation times and A10 (amplitude 10 minutes after clotting time (CT)), flattened α-angle during the EXTEM and diminished MCF for distinct time points during the INTEM, FIBTEM and APTEM assays. With rising age of pRBCs the pH, sodium and potassium reached non-physiological levels.
Conclusion: Under standardized in vitro conditions the higher amount of pRBCs in the 3:1:1 ratio diluted coagulation factors significantly on the expense of its functional coagulation capacity as revealed by ROTEM results. Thus, the coagulation functionality of the 1:1:1 ratio predominated.
Figures
Similar articles
-
The influence of laboratory coagulation tests and clotting factor levels on Rotation Thromboelastometry (ROTEM(R)) during major surgery with hemorrhage.Anesth Analg. 2013 Aug;117(2):314-21. doi: 10.1213/ANE.0b013e31829569ac. Epub 2013 Jun 18. Anesth Analg. 2013. PMID: 23780419
-
The whole is greater than the sum of its parts: hemostatic profiles of whole blood variants.J Trauma Acute Care Surg. 2014 Dec;77(6):818-27. doi: 10.1097/TA.0000000000000354. J Trauma Acute Care Surg. 2014. PMID: 25051379
-
Rotational thromboelastometry-guided blood product management in major spine surgery.J Neurosurg Spine. 2015 Aug;23(2):239-49. doi: 10.3171/2014.12.SPINE14620. Epub 2015 May 22. J Neurosurg Spine. 2015. PMID: 26053893
-
Rapid and correct prediction of thrombocytopenia and hypofibrinogenemia with rotational thromboelastometry in cardiac surgery.J Cardiothorac Vasc Anesth. 2014 Apr;28(2):210-6. doi: 10.1053/j.jvca.2013.12.004. J Cardiothorac Vasc Anesth. 2014. PMID: 24630470
-
Roles of thrombelastography and thromboelastometry for patient blood management in cardiac surgery.Transfus Med Rev. 2013 Oct;27(4):213-20. doi: 10.1016/j.tmrv.2013.08.004. Epub 2013 Sep 26. Transfus Med Rev. 2013. PMID: 24075802 Review.
Cited by
-
The adhesion of clots in wounds contributes to hemostasis and can be enhanced by coagulation factor XIII.Sci Rep. 2020 Nov 18;10(1):20116. doi: 10.1038/s41598-020-76782-z. Sci Rep. 2020. PMID: 33208779 Free PMC article.
-
Prehospital volume resuscitation--Did evidence defeat the crystalloid dogma? An analysis of the TraumaRegister DGU® 2002-2012.Scand J Trauma Resusc Emerg Med. 2016 Apr 6;24:42. doi: 10.1186/s13049-016-0233-4. Scand J Trauma Resusc Emerg Med. 2016. PMID: 27048395 Free PMC article.
References
-
- Borgman MA, Spinella PC, Perkins JG, Grathwohl KW, Repine T, Beekley AC, Sebesta J, Jenkins D, Wade CE, Holcomb JB. The ratio of blood products transfused affects mortality in patients receiving massive transfusions at a combat support hospital. J Trauma. 2007;63:805–813. doi: 10.1097/TA.0b013e3181271ba3. - DOI - PubMed
-
- Hoyt DB, Dutton RP, Hauser CJ, Hess JR, Holcomb JB, Kluger Y, Mackway-Jones K, Parr MJ, Rizoli SB, Yukioka T, Bouillon B. Management of coagulopathy in the patients with multiple injuries: results from an international survey of clinical practice. J Trauma. 2008;65:755–764. doi: 10.1097/TA.0b013e318185fa9f. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

