Dislocation following total hip replacement
- PMID: 25597367
- PMCID: PMC4298240
- DOI: 10.3238/arztebl.2014.0884
Dislocation following total hip replacement
Abstract
Background: Hip replacement ranks among the more successful operations on the musculoskeletal system, but it can have serious complications. A common one is dislocation of the total hip endoprosthesis, an event that arises in about 2% of patients within 1 year of the operation. Physicians should be aware of how this problem can be prevented and, if necessary, treated, so that the degree of trauma due to hip dislocation after hip replacement surgery can be kept to a minimum.
Methods: The authors searched Medline selectively for pertinent publications and analyzed the annual reports of international endoprosthesis registries.
Results: The rate of dislocation of primary hip replacements ranges from 0.2% to 10% per year, while that of artificial hip joints that have already been surgically revised can be as high as 28%, depending on the patient population, the follow-up interval, and the type of prosthesis. Patient-specific risk factors for displacement of a hip endoprosthesis include advanced age, accompanying neurologic disease, and impaired compliance. Patients should scrupulously avoid hip movements such as bending far forward from a standing position, or internal rotation of the flexed hip. Operation-specific risk factors include suboptimal implant position, insufficient soft-tissue tension, and inadequate experience of the surgeon. Conservative treatment is justified the first time dislocation occurs without any identifiable cause. If a mechanical cause of instability is found, then operative revision should be performed as recommended in a standardized treatment algorithm, because, otherwise, dislocation is likely to recur.
Conclusion: The dislocation of a total hip endoprosthesis is an emotionally traumatizing event that should be prevented if possible. Preoperative risk assessment should be performed and the operation should be performed with optimal technique, including the best possible physical configuration of implant components, soft-tissue balance, and an adequately experienced orthopedic surgeon.
Figures
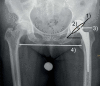


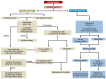

Similar articles
-
[Ways of surgical technique optimization and prevention of hip endoprosthesis dislocation following total hip arthroplasty].Vestn Ross Akad Med Nauk. 2005;(5):32-6. Vestn Ross Akad Med Nauk. 2005. PMID: 15960202 Russian.
-
[Dislocation of total hip prostheses; risk factors and treatment].Ned Tijdschr Geneeskd. 2003 Feb 15;147(7):286-90. Ned Tijdschr Geneeskd. 2003. PMID: 12622005 Review. Dutch.
-
[Emergencies in total hip replacement].Lijec Vjesn. 2005 Jul-Aug;127(7-8):189-93. Lijec Vjesn. 2005. PMID: 16485834 Review. Croatian.
-
[Diagnostics and therapy of luxation after total hip arthroplasty].Orthopade. 2014 Jan;43(1):54-63. doi: 10.1007/s00132-013-2125-x. Orthopade. 2014. PMID: 24384890 German.
-
[Evaluation and treatment of prosthetic hip dislocation].Acta Ortop Mex. 2014 Mar-Apr;28(2):137-44. Acta Ortop Mex. 2014. PMID: 26040158 Review. Spanish.
Cited by
-
Patient-Reported Outcome on Quality of Life and Pain after Revision Arthroplasty for Periprosthetic Joint Infection: A Cross-Sectional Study.J Clin Med. 2022 Dec 2;11(23):7182. doi: 10.3390/jcm11237182. J Clin Med. 2022. PMID: 36498756 Free PMC article.
-
Femoral Head and Liner Exchange in Patients with Atraumatic Dislocation. Results of a Retrospective Study with 6 Years Follow-Up.Medicina (Kaunas). 2021 Nov 1;57(11):1188. doi: 10.3390/medicina57111188. Medicina (Kaunas). 2021. PMID: 34833405 Free PMC article.
-
A novel efficient and precise technique for removing acetabular osteophytes in patients undergoing total hip arthroplasty: the SH-9Hospital acetabular edge file.Ann Transl Med. 2021 Sep;9(17):1366. doi: 10.21037/atm-21-2400. Ann Transl Med. 2021. PMID: 34733918 Free PMC article.
-
Spinopelvic Alignment and Its Use in Total Hip Replacement Preoperative Planning-Decision Making Guide and Literature Review.J Clin Med. 2021 Aug 11;10(16):3528. doi: 10.3390/jcm10163528. J Clin Med. 2021. PMID: 34441824 Free PMC article. Review.
-
Safety and Efficacy of Latitud™ Hip Replacement in Total Hip Arthroplasty: An Observational Study in Kazakhstan.Cureus. 2025 Apr 24;17(4):e82911. doi: 10.7759/cureus.82911. eCollection 2025 Apr. Cureus. 2025. PMID: 40416243 Free PMC article.
References
-
- Learmonth ID, Young C, Rorabeck C. The operation of the century: total hip replacement. Lancet. 2007;370:1508–1519. - PubMed
-
- Iorio R, Robb WJ, Healy WL, et al. Orthopaedic surgeon workforce and volume assessment for total hip and knee replacement in the United States: preparing for an epidemic. J Bone Joint Surg. 2008;90:1598–1605. - PubMed
-
- Kurtz S, Ong K, Lau E, Mowat F, Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg. 2007;89:780–785. - PubMed
-
- Garellick G, Kärrholm J, Rogmark C, Rolfson O, Herberts P. Swedish Hip Arthroplasty Register. Annual Report. 2011 www.shpr.se/en/Publications/DocumentsReports.aspx (last accessed 2 May 2014)
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

