JF-305, a pancreatic cancer cell line is highly sensitive to the PARP inhibitor olaparib
- PMID: 25621047
- PMCID: PMC4301471
- DOI: 10.3892/ol.2014.2762
JF-305, a pancreatic cancer cell line is highly sensitive to the PARP inhibitor olaparib
Abstract
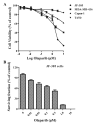
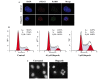
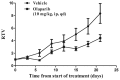
Poly(ADP-ribose) polymerase-1 (PARP-1) is a DNA nick sensor involved in the base excision repair (BER) pathway. Olaparib, a PARP inhibitor, has demonstrated antitumor activity in homologous recombination (HR)-deficient cancers. To extend this specific therapy to other types of carcinomas, a panel of 11 different cancer cells were screened in the present study. JF-305, a pancreatic cancer cell line of Chinese origin, demonstrated sensitivity to the PARP inhibitor 6(5H)-phenanthridinone. In the present study, 3 μM olaparib conferred a cell survival rate of 25% following four days of treatment. The colony formation efficiency was 83% at 10 nM, and dropped to 12% at 1 μM following seven days of treatment. Furthermore, olaparib induced cell cycle arrest in the S and G2/M phases prior to the initiation of apoptosis. Although the incidence of double-strand breaks (DSBs) was increased in the olaparib-treated JF-305 cells, the RAD51 foci were well formed at the sites of γ-H2AX recruitment, indicating an activated HR mechanism. Furthermore, tumor growth was reduced by 49.8% following 22 days of consecutive administration of 10 mg/kg olaparib in the JF-305 xenograft mouse model. In summary, the JF-305 cell line was sensitive to olaparib and provided a prospective model for the preclinical assessment of PARP inhibitors in the therapy of pancreatic cancer.
Keywords: JF-305 cells; cell cycle; homologous recombination repair; olaparib; pancreatic cancer.
Figures

References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous
