Safety and pharmacokinetics of isavuconazole as antifungal prophylaxis in acute myeloid leukemia patients with neutropenia: results of a phase 2, dose escalation study
- PMID: 25624327
- PMCID: PMC4356760
- DOI: 10.1128/AAC.04569-14
Safety and pharmacokinetics of isavuconazole as antifungal prophylaxis in acute myeloid leukemia patients with neutropenia: results of a phase 2, dose escalation study
Abstract
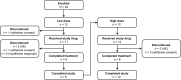
Isavuconazole is a novel broad-spectrum triazole antifungal agent. This open-label dose escalation study assessed the safety and pharmacokinetics of intravenous isavuconazole prophylaxis in patients with acute myeloid leukemia who had undergone chemotherapy and had preexisting/expected neutropenia. Twenty-four patients were enrolled, and 20 patients completed the study. The patients in the low-dose cohort (n = 11) received isavuconazole loading doses on day 1 (400/200/200 mg, 6 h apart) and day 2 (200/200 mg, 12 h apart), followed by once-daily maintenance dosing (200 mg) on days 3 to 28. The loading and maintenance doses were doubled in the high-dose cohort (n = 12). The mean ± standard deviation plasma isavuconazole areas under the concentration-time curves for the dosing period on day 7 were 60.1 ± 22.3 μg · h/ml and 113.1 ± 19.6 μg · h/ml for the patients in the low-dose and high-dose cohorts, respectively. The adverse events in five patients in the low-dose cohort and in eight patients in the high-dose cohort were considered to be drug related. Most were mild to moderate in severity, and the most common adverse events were headache and rash (n = 3 each). One patient in the high-dose cohort experienced a serious adverse event (unrelated to isavuconazole treatment), and two patients each in the low-dose and high-dose cohorts discontinued the study due to adverse events. Of the 20 patients who completed the study, 18 were classified as a treatment success. In summary, the results of this analysis support the safety and tolerability of isavuconazole administered at 200 mg and 400 mg once-daily as prophylaxis in immunosuppressed patients at high risk of fungal infections. (This study is registered at ClinicalTrials.gov under registration number NCT00413439.).
Copyright © 2015, American Society for Microbiology. All Rights Reserved.
Figures

References
-
- Pagano L, Caira M, Candoni A, Offidani M, Fianchi L, Martino B, Pastore D, Picardi M, Bonini A, Chierichini A, Fanci R, Caramatti C, Invernizzi R, Mattei D, Mitra ME, Melillo L, Aversa F, Van Lint MT, Falcucci P, Valentini CG, Girmenia C, Nosari A. 2006. The epidemiology of fungal infections in patients with hematologic malignancies: the SEIFEM-2004 study. Haematologica 91:1068–1075. - PubMed
-
- Caira M, Girmenia C, Fadda RM, Mitra ME, Picardi M, Van Lint MT, Nosari A, Candoni A, Bonini A, Mattei D, de Waure C, Fianchi L, Valentini CG, Aversa F, Leone G, Pagano L. 2008. Invasive fungal infections in patients with acute myeloid leukemia and in those submitted to allogeneic hemopoietic stem cell transplant: who is at highest risk? Eur J Haematol 81:242–243. doi: 10.1111/j.1600-0609.2008.01096.x. - DOI - PubMed
-
- Candoni A, Caira M, Cesaro S, Busca A, Giacchino M, Fanci R, Delia M, Nosari A, Bonini A, Cattaneo C, Melillo L, Caramatti C, Milone G, Scime R, Picardi M, Fanin R, Pagano L. 2013. Multicentre surveillance study on feasibility, safety and efficacy of antifungal combination therapy for proven or probable invasive fungal diseases in haematological patients: the SEIFEM real-life combo study. Mycoses 57:342–350. doi: 10.1111/myc.12161. - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical

