Hospital course and discharge criteria for children hospitalized with bronchiolitis
- PMID: 25627657
- PMCID: PMC4390446
- DOI: 10.1002/jhm.2318
Hospital course and discharge criteria for children hospitalized with bronchiolitis
Abstract
Background: For children hospitalized with bronchiolitis, there is uncertainty about the expected inpatient clinical course and when children are safe for discharge.
Objectives: Examine the time to clinical improvement, risk of clinical worsening after improvement, and develop discharge criteria.
Design: Prospective multiyear cohort study.
Setting: Sixteen US hospitals.
Participants: Consecutive hospitalized children age <2 years with bronchiolitis.
Measurement: We defined clinical improvement using: (1) retraction severity, (2) respiratory rate, (3) room air oxygen saturation, and (4) hydration status. After meeting improvement criteria, children were considered clinically worse based on the inverse of ≥1 of these criteria or need for intensive care.
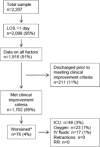
Results: Among 1916 children, the median number of days from onset of difficulty breathing until clinical improvement was 4 (interquartile range, 3-7.5 days). Of the total, 1702 (88%) met clinical improvement criteria, with 4% worsening (3% required intensive care). Children who worsened were age <2 months (adjusted odds ratio [AOR]: 3.51; 95% confidence interval [CI]: 2.07-5.94), gestational age <37 weeks (AOR: 1.94; 95% CI: 1.13-3.32), and presented with severe retractions (AOR: 5.55; 95% CI: 2.12-14.50), inadequate oral intake (AOR: 2.54; 95% CI: 1.39-4.62), or apnea (AOR: 2.87; 95% CI: 1.45-5.68). Readmissions were similar for children who did and did not worsen.
Conclusions: Although children hospitalized with bronchiolitis had wide-ranging recovery times, only 4% worsened after initial improvement. Children who worsened were more likely to be younger, premature infants presenting in more severe distress. For children hospitalized with bronchiolitis, these data may help establish more evidence-based discharge criteria, reduce practice variability, and safely shorten hospital length-of-stay.
© 2015 Society of Hospital Medicine.
Figures
Comment in
-
Safe and efficient discharge in bronchiolitis: how do we get there?J Hosp Med. 2015 Apr;10(4):271-2. doi: 10.1002/jhm.2323. Epub 2015 Jan 28. J Hosp Med. 2015. PMID: 25627958 Free PMC article. No abstract available.
References
-
- Yorita KL, Holman RC, Sejvar JJ, Steiner CA, Schonberger LB. Infectious disease hospitalizations among infants in the United States. Pediatrics. 2008;121(2):244–252. - PubMed
-
- Cunningham S. “A hospital is no place to be sick” Samuel Goldwyn (1882–1974). Arch Dis Child. 2009;94(8):565–566. - PubMed
-
- Christakis D.A, Cowan C.A, Garrison MM, Molteni R, Marcuse E, Zerr DM. Variation in inpatient diagnostic testing and management of bronchiolitis. Pediatrics. 2005;115(4):878–884. - PubMed
-
- Behrendt CE, Decker MD, Burch DJ, Watson PH International variation in the management of infants hospitalized with respiratory syncytial virus. International RSV Study Group. Eur J Pediatr. 1998;157(3):215–220. - PubMed
-
- Cheung CR, Smith H, Thurland K, Duncan H, Semple MG. Population variation in admission rates and duration of inpatient stay for bronchiolitis in England. Arch Dis Child. 2013;98(1):57–59. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous