Full-root aortic valve replacement with stentless xenograft achieves superior regression of left ventricular hypertrophy compared to pericardial stented aortic valves
- PMID: 25643748
- PMCID: PMC4322600
- DOI: 10.1186/s13019-015-0219-8
Full-root aortic valve replacement with stentless xenograft achieves superior regression of left ventricular hypertrophy compared to pericardial stented aortic valves
Abstract
Background: Full-root aortic valve replacement with stentless xenografts has potentially superior hemodynamic performance compared to stented valves. However, a number of cardiac surgeons are reluctant to transform a classical stented aortic valve replacement into a technically more demanding full-root stentless aortic valve replacement. Here we describe our technique of full-root stentless aortic xenograft implantation and compare the early clinical and midterm hemodynamic outcomes to those after aortic valve replacement with stented valves.
Methods: We retrospectively compared the pre-operative characteristics of 180 consecutive patients who underwent full-root replacement with stentless aortic xenografts with those of 80 patients undergoing aortic valve replacement with stented valves. In subgroups presenting with aortic stenosis, we further analyzed the intra-operative data, early postoperative outcomes and mid-term regression of left ventricular mass index.
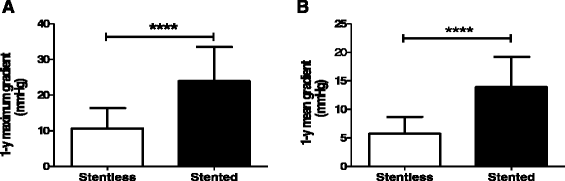
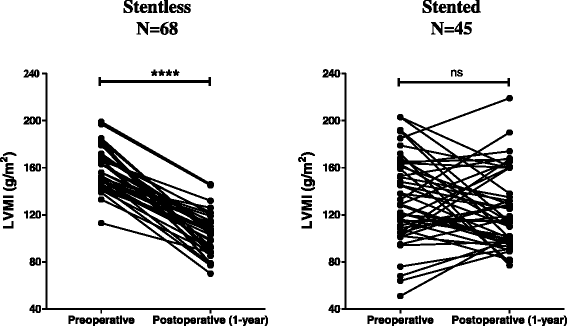
Results: Patients in the stentless group were younger (62.6 ± 13 vs. 70.3 ± 11.8 years, p < 0.0001) but had a higher Euroscore (9.14 ± 3.39 vs.6.83 ± 2.54, p < 0.0001) than those in the stented group. In the subgroups operated for aortic stenosis, the ischemic (84.3 ± 9.8 vs. 62.3 ± 9.4 min, p < 0.0001) and operative times (246.3 ± 53.6 vs. 191.7 ± 53.2 min, p < 0.0001) were longer for stentless versus stented valve implantation. Nevertheless, early mortality (0% vs. 3%, p < 0.25), re-exploration for bleeding (0% vs. 3%, p < 0.25) and stroke (1.8% vs. 3%, p < 0.77) did not differ between stentless and stented groups. One year after the operation, the mean transvalvular gradient was lower in the stentless versus stented group (5.8 ± 2.9 vs. 13.9 ± 5.3 mmHg, p < 0.0001), associated with a significant regression of the left ventricular mass index in the stentless (p < 0.0001) but not in the stented group (p = 0.2).
Conclusion: Our data support that full-root stentless aortic valve replacement can be performed without adversely affecting the early morbidity or mortality in patients operated on for aortic valve stenosis provided that the coronary ostia are not heavily calcified. The additional time necessary for the full-root stentless compared to the classical stented aortic valve replacement is therefore not detrimental to the early clinical outcomes and is largely rewarded in patients with aortic stenosis by lower transvalvular gradients at mid-term and a better regression of their left ventricular mass index.
Figures


References
-
- Bonow RO, Carabello BA, Chatterjee K, de Leon AC, Jr, Faxon DP, Freed MD, et al. 2008 Focused Update Incorporated Into the ACC/AHA 2006 Guidelines for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons 2006 WRITING COMMITTEE MEMBERS. Circulation. 2008;118:e523–661. doi: 10.1161/CIRCULATIONAHA.108.190748. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

