Dietary restrictions in dialysis patients: is there anything left to eat?
- PMID: 25649719
- PMCID: PMC4385746
- DOI: 10.1111/sdi.12348
Dietary restrictions in dialysis patients: is there anything left to eat?
Abstract
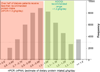
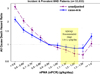
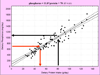
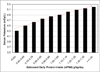
A significant number of dietary restrictions are imposed traditionally and uniformly on maintenance dialysis patients, whereas there is very little data to support their benefits. Recent studies indicate that dietary restrictions of phosphorus may lead to worse survival and poorer nutritional status. Restricting dietary potassium may deprive dialysis patients of heart-healthy diets and lead to intake of more atherogenic diets. There is little data about the survival benefits of dietary sodium restriction, and limiting fluid intake may inherently lead to lower protein and calorie consumption, when in fact dialysis patients often need higher protein intake to prevent and correct protein-energy wasting. Restricting dietary carbohydrates in diabetic dialysis patients may not be beneficial in those with burnt-out diabetes. Dietary fat including omega-3 fatty acids may be important caloric sources and should not be restricted. Data to justify other dietary restrictions related to calcium, vitamins, and trace elements are scarce and often contradictory. The restriction of eating during hemodialysis treatment is likely another incorrect practice that may worsen hemodialysis induced hypoglycemia and nutritional derangements. We suggest careful relaxation of most dietary restrictions and adoption of a more balanced and individualized approach, thereby easing some of these overzealous restrictions that have not been proven to offer major advantages to patients and their outcomes and which may in fact worsen patients' quality of life and satisfaction. This manuscript critically reviews the current paradigms and practices of recommended dietary regimens in dialysis patients including those related to dietary protein, carbohydrate, fat, phosphorus, potassium, sodium, and calcium, and discusses the feasibility and implications of adherence to ardent dietary restrictions and future research.
© 2015 Wiley Periodicals, Inc.
Conflict of interest statement
KKZ has received honoraria from Abbott, Abbvie, Fresenius, Keryx, Shire, Vifor, and other manufacturers of phosphorus binders, nutritional supplements, or medications and items related to dialysis patients.
Figures

References
-
- Ikizler TA, Franch HA, Kalantar-Zadeh K, ter Wee PM, Wanner C. Time to revisit the role of renal dietitian in the dialysis unit. Journal of renal nutrition : the official journal of the Council on Renal Nutrition of the National Kidney Foundation. 2014;24:58–60. - PubMed
-
- Streja E, Molnar MZ, Kovesdy CP, Bunnapradist S, Jing J, Nissenson AR, Mucsi I, Danovitch GM, Kalantar-Zadeh K. Associations of pretransplant weight and muscle mass with mortality in renal transplant recipients. Clinical journal of the American Society of Nephrology : CJASN. 2011;6:1463–1473. - PMC - PubMed
-
- Khoueiry G, Waked A, Goldman M, El-Charabaty E, Dunne E, Smith M, Kleiner M, Lafferty J, Kalantar-Zadeh K, El-Sayegh S. Dietary intake in hemodialysis patients does not reflect a heart healthy diet. Journal of renal nutrition : the official journal of the Council on Renal Nutrition of the National Kidney Foundation. 2011;21:438–447. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

