Emerging clinical applications of selected biomarkers in melanoma
- PMID: 25674009
- PMCID: PMC4321413
- DOI: 10.2147/CCID.S49578
Emerging clinical applications of selected biomarkers in melanoma
Abstract
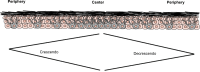
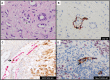
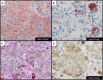
Melanoma is a lethal skin disease with a mostly predictable clinical course according to a known constellation of clinical and pathologic features. The distinction of melanoma from benign melanocytic nevus is typically unequivocol; however, there is a subset of tumors known for its diagnostic challenges, development of late metastases, and difficulties in treatment. Several melanocytic tissue biomarkers are available that can facilitate the histopathologic interpretation of melanoma as well as provide insight into the biologic potential and mutational status of this disease. This review describes the clinical application of some of these established and emerging tissue biomarkers available to assess melanocytic differentiation, vascular invasion, mitotic capacity, and mutation status. The selected tissue biomarkers in this review include MiTF, Sox10, D2-40, PHH3, H3KT (anti-H3K79me3T80ph), anti-BRAFV600E, and anti-BAP-1.
Keywords: BRAFV600E; histone marks; immunohistochemistry; melanocytic differentiation.
Figures




Similar articles
-
BAP1 and BRAFV600E expression in benign and malignant melanocytic proliferations.Hum Pathol. 2015 Feb;46(2):239-45. doi: 10.1016/j.humpath.2014.10.015. Epub 2014 Nov 4. Hum Pathol. 2015. PMID: 25479927
-
Comparison of pHH3, Ki-67, and survivin immunoreactivity in benign and malignant melanocytic lesions.Am J Dermatopathol. 2008 Apr;30(2):117-22. doi: 10.1097/DAD.0b013e3181624054. Am J Dermatopathol. 2008. PMID: 18360113
-
Detection of mitotic figures and G2+ tumor nuclei with histone markers correlates with worse overall survival in patients with Merkel cell carcinoma.J Cutan Pathol. 2014 Nov;41(11):846-52. doi: 10.1111/cup.12383. Epub 2014 Oct 28. J Cutan Pathol. 2014. PMID: 25263506 Free PMC article.
-
Common and not so Common Melanocytic Lesions in Children and Adolescents.Pediatr Dev Pathol. 2018 Mar-Apr;21(2):252-270. doi: 10.1177/1093526617751720. Pediatr Dev Pathol. 2018. PMID: 29607755 Review.
-
Immunohistochemistry in melanocytic lesions: Updates with a practical review for pathologists.Semin Diagn Pathol. 2022 Jul;39(4):239-247. doi: 10.1053/j.semdp.2021.12.003. Epub 2022 Jan 1. Semin Diagn Pathol. 2022. PMID: 35016807 Review.
Cited by
-
Atypical Melanocytic Proliferations: A Review of the Literature.Dermatol Surg. 2018 Feb;44(2):159-174. doi: 10.1097/DSS.0000000000001367. Dermatol Surg. 2018. PMID: 29059147 Free PMC article. Review.
-
Deciphering the Role of BRAFV600E Immunohistochemistry in Breast Lesions: A Comprehensive Review.Cureus. 2024 Jul 18;16(7):e64872. doi: 10.7759/cureus.64872. eCollection 2024 Jul. Cureus. 2024. PMID: 39156294 Free PMC article. Review.
-
Diagnosis and management of lentigo maligna: a review.Drugs Context. 2015 May 29;4:212281. doi: 10.7573/dic.212281. eCollection 2015. Drugs Context. 2015. PMID: 26082796 Free PMC article. Review.
-
Identification of transcription factors (TFs) and targets involved in the cholangiocarcinoma (CCA) by integrated analysis.Cancer Gene Ther. 2016 Dec;23(12):439-445. doi: 10.1038/cgt.2016.64. Epub 2016 Nov 18. Cancer Gene Ther. 2016. PMID: 27857060
-
Identification of key candidate genes involved in melanoma metastasis.Mol Med Rep. 2019 Aug;20(2):903-914. doi: 10.3892/mmr.2019.10314. Epub 2019 May 30. Mol Med Rep. 2019. PMID: 31173190 Free PMC article.
References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

