Randomized, double-blind, dose-escalation trial of triptorelin for ovary protection in childhood-onset systemic lupus erythematosus
- PMID: 25676588
- PMCID: PMC4414812
- DOI: 10.1002/art.39024
Randomized, double-blind, dose-escalation trial of triptorelin for ovary protection in childhood-onset systemic lupus erythematosus
Abstract
Objective: To determine the dose of triptorelin that is sufficient to maintain complete ovarian suppression in female patients with childhood-onset systemic lupus erythematosus (SLE) who require cyclophosphamide therapy, to determine the length of time needed to achieve ovarian suppression after initiation of triptorelin treatment, and to investigate the safety of triptorelin.
Methods: In this randomized, double-blind, placebo-controlled, dose-escalation study, female patients ages <21 years were randomized 4:1 to receive triptorelin (n = 25) or placebo (n = 6). The starting doses of triptorelin were 25, 50, 75, and 100 μg/kg, and the dose was escalated until complete ovarian suppression was maintained. The primary outcome was the weight-adjusted dose of triptorelin that provided complete ovarian suppression in at least 90% of the patients, as determined by gonadotropin-releasing hormone agonist stimulation testing. The secondary outcome was the period of time required to achieve ovarian suppression, as measured by unstimulated follicle-stimulating hormone and luteinizing hormone levels after the initiation of triptorelin treatment.
Results: Treatment with triptorelin at a weight-adjusted dose of 120 μg/kg body weight provided sustained complete ovarian suppression in 90% of the patients. After administration of the initial dose of triptorelin, 22 days were required to achieve complete ovarian suppression. The rates of adverse events (AEs) and serious adverse events (SAEs) per 100 patient-months of followup were not higher in the triptorelin group compared with the placebo group (for AEs, 189 versus 362; for SAEs, 2.1 versus 8.5).
Conclusion: High doses of triptorelin are needed to achieve and maintain complete ovarian suppression, but such doses appear to be well tolerated in adolescent female patients with childhood-onset SLE. Our data suggest that a lag time of 22 days after initiation of triptorelin treatment is required before cyclophosphamide therapy is started or continued.
Trial registration: ClinicalTrials.gov NCT00124514.
© 2015, American College of Rheumatology.
Conflict of interest statement
None of the authors perceive to have a conflict of interest relevant to the conduct of this study.
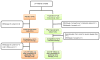
Figures

Similar articles
-
Effect of the gonadotropin-releasing hormone analogue triptorelin on the occurrence of chemotherapy-induced early menopause in premenopausal women with breast cancer: a randomized trial.JAMA. 2011 Jul 20;306(3):269-76. doi: 10.1001/jama.2011.991. JAMA. 2011. PMID: 21771987 Clinical Trial.
-
Effect of a gonadotropin-releasing hormone analogue on cyclophosphamide-induced ovarian toxicity in adult mice.Arch Gynecol Obstet. 2013 May;287(5):1023-9. doi: 10.1007/s00404-012-2658-y. Epub 2012 Dec 7. Arch Gynecol Obstet. 2013. PMID: 23224696
-
Short term pituitary desensitization: effects of different doses of the gonadotrophin-releasing hormone agonist triptorelin.Hum Reprod. 1996 Jan;11(1):55-60. doi: 10.1093/oxfordjournals.humrep.a019034. Hum Reprod. 1996. PMID: 8671156 Clinical Trial.
-
Ovarian protection with gonadotropin-releasing hormone agonists during cyclophosphamide therapy in systemic lupus erythematosus.Best Pract Res Clin Obstet Gynaecol. 2020 Apr;64:97-106. doi: 10.1016/j.bpobgyn.2019.10.008. Epub 2019 Nov 13. Best Pract Res Clin Obstet Gynaecol. 2020. PMID: 31866283 Review.
-
Ovarian failure in systemic lupus erythematosus patients treated with pulsed intravenous cyclophosphamide.Lupus. 2004;13(9):673-8. doi: 10.1191/0961203304lu2012oa. Lupus. 2004. PMID: 15485101 Review.
Cited by
-
Menopause and Rheumatic Disease.Rheum Dis Clin North Am. 2017 May;43(2):287-302. doi: 10.1016/j.rdc.2016.12.011. Rheum Dis Clin North Am. 2017. PMID: 28390570 Free PMC article. Review.
-
Gonadotropin-Releasing Hormone Analogs for Gonadal Protection During Gonadotoxic Chemotherapy: A Systematic Review and Meta-Analysis.Reprod Sci. 2019 Jul;26(7):939-953. doi: 10.1177/1933719118799203. Epub 2018 Oct 1. Reprod Sci. 2019. PMID: 30270741
-
Gonadotropin ratio affects the in vitro growth of rhesus ovarian preantral follicles.J Investig Med. 2016 Apr;64(4):888-93. doi: 10.1136/jim-2015-000001. Epub 2016 Mar 15. J Investig Med. 2016. PMID: 26980777 Free PMC article.
-
Unveiling the Effects of Triptorelin on Endocrine Profiles: Insights From Healthy, Polycystic Ovary Syndrome, and Hypothalamic Amenorrhea Women.Cureus. 2023 Sep 5;15(9):e44752. doi: 10.7759/cureus.44752. eCollection 2023 Sep. Cureus. 2023. PMID: 37809244 Free PMC article. Review.
-
Treatment of Juvenile Dermatomyositis: An Update.Paediatr Drugs. 2017 Oct;19(5):423-434. doi: 10.1007/s40272-017-0240-6. Paediatr Drugs. 2017. PMID: 28550457 Review.
References
-
- Koo HS, Kim YC, Lee SW, Kim DK, Oh KH, Joo KW, et al. The effects of cyclophosphamide and mycophenolate on end-stage renal disease and death of lupus nephritis. Lupus. 2011;20(13):1442–1449. - PubMed
-
- Ioannidis JP, Katsifis GE, Tzioufas AG, Moutsopoulos HM. Predictors of sustained amenorrhea from pulsed intravenous cyclophosphamide in premenopausal women with systemic lupus erythematosus. J Rheumatol. 2002;29(10):2129–2135. - PubMed
-
- Manger K, Wildt L, Kalden JR, Manger B. Prevention of gonadal toxicity and preservation of gonadal function and fertility in young women with systemic lupus erythematosus treated by cyclophosphamide: the PREGO-Study. Autoimmunity reviews. 2006;5(4):269–272. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

