Fundus autofluorescence characteristics of nascent geographic atrophy in age-related macular degeneration
- PMID: 25678689
- PMCID: PMC4349109
- DOI: 10.1167/iovs.14-16211
Fundus autofluorescence characteristics of nascent geographic atrophy in age-related macular degeneration
Abstract
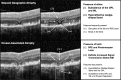
Purpose: We examined the fundus autofluorescence (FAF) characteristics of nascent geographic atrophy (nGA), pathological features preceding the development of drusen-associated atrophy in eyes with age-related macular degeneration (AMD) that can be visualized using high-resolution optical coherence tomography (OCT).
Methods: Spectral-domain OCT (SD-OCT) and FAF imaging were performed longitudinally in 221 eyes with intermediate AMD (having at least drusen >125 μm), and seven areas that developed drusen-associated atrophy in five eyes were examined and categorized with respect to FAF characteristics. These categories then were used to characterize 49 areas of nGA or drusen-associated atrophy on SD-OCT identified in a cross-sectional study with 230 participants with bilateral intermediate AMD.
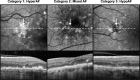
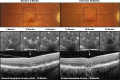
Results: Sequential imaging revealed that FAF characteristics in the atrophic areas could be grouped into three categories: predominantly hyperautofluorescent (hyperAF), presence of both hyper- and hypoautofluorescence (mixed AF), or predominantly hypoautofluorescent (hypoAF). In the cross-sectional study, the FAF characteristics were significantly dependent on the type of atrophic area (P = 0.002), where areas of nGA appeared most commonly as being mixed AF (63%), while areas of drusen-associated atrophy most commonly as hypoAF (86%).
Conclusions: Fundus autofluorescence imaging revealed that areas of nGA were most commonly characterized by both hyper- and hypoautofluorescent changes, which differs from areas of drusen-associated atrophy that most often appeared hypoautofluorescent. These findings provide important insights into the FAF characteristics of areas undergoing atrophic changes in eyes still considered to be in the early stages of AMD by current methods, and thus assist in the characterization of disease severity in these early stages.
Keywords: age-related macular degeneration; drusen; fundus autofluorescence; geographic atrophy; spectral-domain optical coherence tomography.
Copyright 2015 The Association for Research in Vision and Ophthalmology, Inc.
Figures
References
-
- Bindewald A, Bird AC, Dandekar SS, et al. Classification of fundus autofluorescence patterns in early age-related macular disease. Invest Ophthalmol Vis Sci. 2005; 46: 3309–3314. - PubMed
-
- Hogg RE, Chakravarthy U. Visual function and dysfunction in early and late age-related maculopathy. Prog Retin Eye Res. 2006; 25: 249–276. - PubMed
-
- Neelam K, Nolan J, Chakravarthy U, Beatty S. Psychophysical function in age-related maculopathy. Surv Ophthalmol. 2009; 54: 167–210. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

