Diagnosis of deep vein thrombosis, and prevention of deep vein thrombosis recurrence and the post-thrombotic syndrome in the primary care medicine setting anno 2014
- PMID: 25685720
- PMCID: PMC4326761
- DOI: 10.5492/wjccm.v4.i1.29
Diagnosis of deep vein thrombosis, and prevention of deep vein thrombosis recurrence and the post-thrombotic syndrome in the primary care medicine setting anno 2014
Abstract
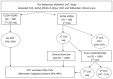
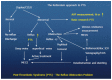
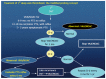
The requirement for a safe diagnostic strategy of deep vein thrombosis (DVT) should be based on an overall objective post incidence of venous thromboembolism (VTE) of less than 1% during 3 mo follow-up. Compression ultrasonography (CUS) of the leg veins has a negative predictive value (NPV) of 97%-98% indicating the need of repeated CUS testing within one week. A negative ELISA VIDAS safely excludes DVT and VTE with a NPV between 99% and 100% at a low clinical score of zero. The combination of low clinical score and a less sensitive D-dimer test (Simplify) is not sensitive enough to exclude DVT and VTE in routine daily practice. From prospective clinical research studies it may be concluded that complete recanalization within 3 mo and no reflux is associated with a low or no risk of PTS obviating the need of MECS 6 mo after DVT. Partial and complete recanalization after 3 to more than 6 mo is usually complicated by reflux due to valve destruction and symptomatic PTS. Reflux seems to be a main determinant for PTS and DVT recurrence, the latter as a main contributing factor in worsening PTS. This hypothesis is supported by the relation between the persistent residual vein thrombosis (RVT = partial recanalization) and the risk of VTE recurrence in prospective studies. Absence of RVT at 3 mo post-DVT and no reflux is predicted to be associated with no recurrence of DVT (1.2%) during follow-up obviating the need of wearing medical elastic stockings and anticoagulation at 6 mo post-DVT. The presence or absence of RVT but with reflux at 3 to 6 mo post-DVT is associated with both symptomatic PTS and an increased risk of VTE recurrence in about one third in the post-DVT period after regular discontinuation of anticoagulant treatment. To test this hypothesis we designed a prospective DVT and postthrombotic syndrome (PTS) Bridging the Gap Study by addressing at least four unanswered questions in the treatment of DVT and PTS. Which DVT patient has a clear indication for long-term compression stocking therapy to prevent PTS after the initial anticoagulant treatment in the acute phase of DVT? Is 3 mo the appropriate point in time to determine candidates at risk to develop DVT recurrence and PTS? Which high risk symptomatic PTS patients need extended anticoagulant treatment?
Keywords: Anticoagulation; Deep Venous thrombosis; ELISA VIDAS D-dimer; Medical elastic stockings; Post-thrombotic syndrome; Ultrasonography.
Figures


Similar articles
-
Duplex ultrasound, clinical score, thrombotic risk, and D-dimer testing for evidence based diagnosis and management of deep vein thrombosis and alternative diagnoses in the primary care setting and outpatient ward.Int Angiol. 2014 Feb;33(1):1-19. Int Angiol. 2014. PMID: 24452081 Review.
-
A critical appraisal of non-invasive diagnosis and exclusion of deep vein thrombosis and pulmonary embolism in outpatients with suspected deep vein thrombosis or pulmonary embolism: how many tests do we need?Int Angiol. 2005 Mar;24(1):27-39. Int Angiol. 2005. PMID: 15876996 Review.
-
Screening for deep vein thrombosis and pulmonary embolism in outpatients with suspected DVT or PE by the sequential use of clinical score: a sensitive quantitative D-dimer test and noninvasive diagnostic tools.Semin Vasc Med. 2005 Nov;5(4):351-64. doi: 10.1055/s-2005-922480. Semin Vasc Med. 2005. PMID: 16302156 Review.
-
Diagnosis of deep vein thrombosis: how many tests do we need?Acta Chir Belg. 2005 Feb;105(1):16-25. Acta Chir Belg. 2005. PMID: 15790198 Review.
-
Different accuracies of rapid enzyme-linked immunosorbent, turbidimetric, and agglutination D-dimer assays for thrombosis exclusion: impact on diagnostic work-ups of outpatients with suspected deep vein thrombosis and pulmonary embolism.Semin Thromb Hemost. 2006 Oct;32(7):678-93. doi: 10.1055/s-2006-951296. Semin Thromb Hemost. 2006. PMID: 17024595 Review.
Cited by
-
Leg Swelling Caused by Heterotopic Ossification Mimicking Deep Vein Thrombosis in a Paraplegic Patient.Korean J Neurotrauma. 2015 Oct;11(2):158-61. doi: 10.13004/kjnt.2015.11.2.158. Epub 2015 Oct 31. Korean J Neurotrauma. 2015. PMID: 27169085 Free PMC article.
-
The Diagnostic Efficacy of Age-Adjusted D-Dimer Cutoff Value and Pretest Probability Scores for Deep Venous Thrombosis.Clin Appl Thromb Hemost. 2019 Jan-Dec;25:1076029619826317. doi: 10.1177/1076029619826317. Clin Appl Thromb Hemost. 2019. PMID: 30754991 Free PMC article.
-
Association between small intestinal bacterial overgrowth and deep vein thrombosis.Gastroenterol Rep (Oxf). 2016 Nov;4(4):299-303. doi: 10.1093/gastro/gow004. Epub 2016 Apr 4. Gastroenterol Rep (Oxf). 2016. PMID: 27044499 Free PMC article.
-
Venous and arterial thromboembolism in patients with inflammatory bowel diseases.World J Gastroenterol. 2021 Oct 28;27(40):6757-6774. doi: 10.3748/wjg.v27.i40.6757. World J Gastroenterol. 2021. PMID: 34790006 Free PMC article. Review.
-
Short-Term Anticoagulant Therapy and Thrombus Location Are Independent Risk Factors for Delayed Recanalization of Deep Vein Thrombosis.Med Sci Monit. 2016 Jan 21;22:219-25. doi: 10.12659/msm.895228. Med Sci Monit. 2016. PMID: 26790571 Free PMC article.
References
-
- Freyburger G, Trillaud H, Labrouche S, Gauthier P, Javorschi S, Bernard P, Grenier N. D-dimer strategy in thrombosis exclusion--a gold standard study in 100 patients suspected of deep venous thrombosis or pulmonary embolism: 8 DD methods compared. Thromb Haemost. 1998;79:32–37. - PubMed
-
- van der Graaf F, van den Borne H, van der Kolk M, de Wild PJ, Janssen GW, van Uum SH. Exclusion of deep venous thrombosis with D-dimer testing--comparison of 13 D-dimer methods in 99 outpatients suspected of deep venous thrombosis using venography as reference standard. Thromb Haemost. 2000;83:191–198. - PubMed
-
- Perrier A, Desmarais S, Miron MJ, de Moerloose P, Lepage R, Slosman D, Didier D, Unger PF, Patenaud JV, Bounameax H. Non-invasive diagnosis of venous thromboembolism in outpatients. Lancet. 1999;353:190–195. - PubMed
-
- Oudega R, Moons KG, Hoes AW. Ruling out deep venous thrombosis in primary care. A simple diagnostic algorithm including D-dimer testing. Thromb Haemost. 2005;94:200–205. - PubMed
-
- Oudega R, Hoes AW, Moons KG. The Wells rule does not adequately rule out deep venous thrombosis in primary care patients. Ann Intern Med. 2005;143:100–107. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

