Is Self-Referral Associated with Higher Quality Care?
- PMID: 25759002
- PMCID: PMC4600357
- DOI: 10.1111/1475-6773.12289
Is Self-Referral Associated with Higher Quality Care?
Abstract
Objective: To assess the extent to which patients self-refer to cancer specialists and whether self-referral is associated with better experiences and quality of care.
Data sources: Data from surveys and medical record abstraction collected through the Cancer Care Outcomes Research and Surveillance Consortium.
Study design: Observational study of patients with lung and colorectal cancer diagnosed from 2003 through 2005 in five geographically defined regions and five integrated health care delivery systems.
Methods: Multivariable logistic regression models used to assess factors associated with self-referral and propensity score-weighted doubly robust models to test the association between self-referral and experiences/quality of care.
Principal findings: Among 5,882 patients, 9.7 percent of lung cancer patients and 14.9 percent of colorectal cancer patients self-referred to at least one cancer specialist. Black patients were less likely to self-refer than white patients (odds ratio: 0.48, 95 percent confidence interval: 0.35, 0.64); patients with high incomes (vs. low) and with a college degree (vs. non-high school graduates) were significantly more likely to self-refer. Self-referral was associated with lower ratings of overall physician communication for patients with lung cancer but, conversely, higher odds of curative surgery among patients with stage I/II lung cancer.
Conclusions: A small but significant proportion of patients self-referred to their cancer specialists; rates varied by patient race and socioeconomic status. To the extent that self-referral is associated with quality, it may reinforce disparities in care.
Keywords: Self-referral; colorectal cancer; lung cancer; referral.
© Health Research and Educational Trust.
Figures

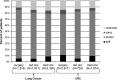

Note: Doubly robust models adjust for propensity weights and sociodemographic, clinical, insurance, and health care delivery-related factors. Due to collinearity, the following variables were removed: from the overall quality of care, we omitted whether the patient had a PCP; for adjuvant chemotherapy for stage III colon cancer, we omitted age, insurance, education, income, marital status, PCP status, and number of different providers referred to; for adjuvant chemotherapy and radiation for rectal cancer, we omitted age, insurance, education, income, marital status, comorbidity, PCP status, number of different providers referred to, and CanCORs site; for curative surgery for early-stage lung cancer, we omitted age, comorbidity, and PCP status.
References
-
- Ayanian JZ, Chrischilles EA, Wallace RB, Fletcher RH, Fouad MN, Kiefe CI, Harrington DP, Weeks JC, Kahn KL, Malin JL, Lipscomb J, Potosky AL, Provenzale DT, Sandler RS, van Ryn M. West DW. Understanding Cancer Treatment and Outcomes: The Cancer Care Outcomes Research and Surveillance Consortium. Journal of Clinical Oncology. 2004;22(15):2992–6. - PubMed
-
- Ayanian JZ, Zaslavsky AM, Arora NK, Kahn KL, Malin JL, Ganz PA, van Ryn M, Hornbrook MC, Kiefe CI, He Y, Urmie JM, Weeks JC. Harrington DP. Patients' Experiences with Care for Lung Cancer and Colorectal Cancer: Findings from the Cancer Care Outcomes Research and Surveillance Consortium. Journal of Clinical Oncology. 2010;28(27):4154–61. - PMC - PubMed
-
- Ayanian JZ, Zaslavsky AM, Guadagnoli E, Fuchs CS, Yost KJ, Creech CM, Cress RD, O'Connor LC, West DW. Wright WE. Patients' Perceptions of Quality of Care for Colorectal Cancer by Race, Ethnicity, and Language. Journal of Clinical Oncology. 2005;23(27):6576–86. - PubMed
Publication types
MeSH terms
Grants and funding
- U01CA093339/CA/NCI NIH HHS/United States
- U01CA093329/CA/NCI NIH HHS/United States
- U01 CA093329/CA/NCI NIH HHS/United States
- U01 CA093348/CA/NCI NIH HHS/United States
- U01 CA093324/CA/NCI NIH HHS/United States
- U01CA093324/CA/NCI NIH HHS/United States
- U01CA093344/CA/NCI NIH HHS/United States
- U01CA093332/CA/NCI NIH HHS/United States
- U01 CA093339/CA/NCI NIH HHS/United States
- K07CA151910/CA/NCI NIH HHS/United States
- U01 CA093344/CA/NCI NIH HHS/United States
- K07 CA151910/CA/NCI NIH HHS/United States
- U01 CA093326/CA/NCI NIH HHS/United States
- U01 CA093332/CA/NCI NIH HHS/United States
- U01CA093348/CA/NCI NIH HHS/United States
- U01CA093326/CA/NCI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

