Microsurgical management of aneurysms of the superior cerebellar artery - lessons learnt: An experience of 14 consecutive cases and review of the literature
- PMID: 25767580
- PMCID: PMC4352632
- DOI: 10.4103/1793-5482.151513
Microsurgical management of aneurysms of the superior cerebellar artery - lessons learnt: An experience of 14 consecutive cases and review of the literature
Abstract
Objective: This is a retrospective study from January 2002 to December 2012 analyzing the results of microsurgical clipping for aneurysms arising from the superior cerebellar artery (SCA).
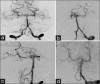
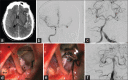
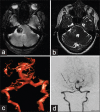
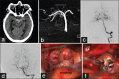
Materials and methods: All patients with SCA were evaluated with computerized tomography angiography and/or digital subtraction angiography (DSA) prior to surgery. All patients in our series underwent microsurgical clipping and postoperative DSA to assess the extent of aneurysm occlusion. The Glasgow outcome scale (GOS) and the modified Rankin's scale (mRS) were used to grade their postoperative neurological status at discharge and 6 months, respectively.
Results: Fourteen patients had SCA aneurysms (ruptured-9, unruptured-5). There were 10 females and 4 males with the mean age of 47.2 years (median - 46 years, range = 24-66 years). Subarachnoid hemorrhage (SAH) was seen in 11 patients. The mean duration of symptoms was 2.5 days (range = 1-7 days). The WFNS score at presentation was as follows: Grade 1 in 10 cases, II in 2 cases, III in 1 case and IV in 1 case. In the 9 cases with ruptured SCA aneurysm, average size of the ruptured aneurysms was 7.3 mm (range = 2.5-27 mm, median = 4.9 mm). The subtemporal approach was used in the first 7 cases. The extradural temporopolar (EDTP) approach was used in the last 5 cases. Complications include vasospasm (n = 6), third nerve palsy (n = 5) and hydrocephalus (n = 3). Two patients died following surgery. At mean follow-up 33.8 months (median - 25 months, range = 19-96 months), no patient had a rebleed. At discharge 9 (64%), had a GOS of 4 or 5 and 3 (21%) had a GOS of 3. At 6 months follow-up, 10/14 (71%) patients had mRS of 0-2, and 2 (14%) had mRS of 5.
Conclusions: Aneurysms of the SCA are uncommon and tend to rupture even when the aneurysm size is small (<7 mm). They commonly present with SAH. The EDTP approach avoids complication caused by temporal lobe retraction and injury to the vein of Labbe.
Keywords: Accessory superior cerebellar artery; aneurysm; extradural temporopolar approach; subarachnoid hemorrhage; superior cerebellar artery.
Conflict of interest statement
Figures
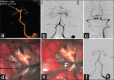

References
LinkOut - more resources
Full Text Sources
Other Literature Sources

