Significant risk and associated factors of active tuberculosis infection in Korean patients with inflammatory bowel disease using anti-TNF agents
- PMID: 25805938
- PMCID: PMC4363761
- DOI: 10.3748/wjg.v21.i11.3308
Significant risk and associated factors of active tuberculosis infection in Korean patients with inflammatory bowel disease using anti-TNF agents
Abstract
Aim: To evaluate the incidence and risk factors of Korean tuberculosis (TB) infection in patients with inflammatory bowel disease (IBD) undergoing anti-TNF treatment.
Methods: The data of IBD patients treated with anti-TNFs in 13 tertiary referral hospitals located in the southeastern region of Korea were collected retrospectively. They failed to show response or were intolerant to conventional treatments, including steroids or immunomodulators. Screening measures for latent TB infection (LTBI) and the incidence and risk factors of active TB infection after treatment with anti-TNFs were identified.
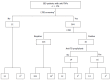
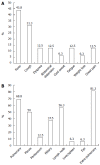
Results: Overall, 376 IBD patients treated with anti-TNF agents were recruited (male 255, mean age of anti-TNF therapy 32.5 ± 13.0 years); 277 had Crohn's disease, 99 had ulcerative colitis, 294 used infliximab, and 82 used adalimumab. Before anti-TNF treatment, screening tests for LTBI including an interferon gamma release assay or a tuberculin skin test were performed in 82.2% of patients. Thirty patients (8%) had LTBI. Sixteen cases of active TB infection including one TB-related mortality occurred during 801 person-years (PY) follow-up (1997.4 cases per 100000 PY) after anti-TNF treatment. LTBI (OR = 5.76, 95%CI: 1.57-21.20, P = 0.008) and WBC count < 5000 mm(3) (OR = 4.5, 95%CI: 1.51-13.44, P = 0.007) during follow-up were identified as independently associated risk factors.
Conclusion: Anti-TNFs significantly increase the risk of TB infection in Korean patients with IBD. The considerable burden of TB and marked immunosuppression might be attributed to this risk.
Keywords: Anti-TNF; Inflammatory bowel disease; Korea; Latent tuberculosis infection; Risk factor; Tuberculosis.
Figures
Similar articles
-
Latent tuberculosis infection detection and active tuberculosis prevention in patients receiving anti-TNF therapy: an Italian nationwide survey.Int J Rheum Dis. 2016 Aug;19(8):799-805. doi: 10.1111/1756-185X.12708. Epub 2015 Jul 14. Int J Rheum Dis. 2016. PMID: 26172207
-
Negative Screening Does Not Rule Out the Risk of Tuberculosis in Patients with Inflammatory Bowel Disease Undergoing Anti-TNF Treatment: A Descriptive Study on the GETAID Cohort.J Crohns Colitis. 2016 Oct;10(10):1179-85. doi: 10.1093/ecco-jcc/jjw129. Epub 2016 Jul 11. J Crohns Colitis. 2016. PMID: 27402916
-
Serious infections in patients with inflammatory bowel disease receiving anti-tumor-necrosis-factor-alpha therapy: an Australian and New Zealand experience.J Gastroenterol Hepatol. 2010 Nov;25(11):1732-8. doi: 10.1111/j.1440-1746.2010.06407.x. J Gastroenterol Hepatol. 2010. PMID: 21039834
-
Management of inflammatory bowel disease with infliximab and other anti-tumor necrosis factor alpha therapies.BioDrugs. 2010 Dec 14;24 Suppl 1:3-14. doi: 10.2165/11586290-000000000-00000. BioDrugs. 2010. PMID: 21175228 Review.
-
Asian Organization for Crohn's and Colitis and Asian Pacific Association of Gastroenterology consensus on tuberculosis infection in patients with inflammatory bowel disease receiving anti-tumor necrosis factor treatment. Part 1: Risk assessment.J Gastroenterol Hepatol. 2018 Jan;33(1):20-29. doi: 10.1111/jgh.14019. J Gastroenterol Hepatol. 2018. PMID: 29023903 Review.
Cited by
-
The Impact of Korean Medicine Treatment on the Incidence of Parkinson's Disease in Patients with Inflammatory Bowel Disease: A Nationwide Population-Based Cohort Study in South Korea.J Clin Med. 2020 Jul 28;9(8):2422. doi: 10.3390/jcm9082422. J Clin Med. 2020. PMID: 32731605 Free PMC article.
-
Clinical features of active tuberculosis that developed during anti-tumor necrosis factor therapy in patients with inflammatory bowel disease.Intest Res. 2016 Apr;14(2):146-51. doi: 10.5217/ir.2016.14.2.146. Epub 2016 Apr 27. Intest Res. 2016. PMID: 27175115 Free PMC article.
-
QuantiFERON-TB Gold Test Conversion Is Associated with Active Tuberculosis Development in Inflammatory Bowel Disease Patients Treated with Biological Agents: An Experience of a Medical Center in Taiwan.Gastroenterol Res Pract. 2019 Nov 3;2019:7132875. doi: 10.1155/2019/7132875. eCollection 2019. Gastroenterol Res Pract. 2019. PMID: 31781198 Free PMC article.
-
Risk and characteristics of tuberculosis after anti-tumor necrosis factor therapy for inflammatory bowel disease: a hospital-based cohort study from Korea.BMC Gastroenterol. 2021 Oct 20;21(1):390. doi: 10.1186/s12876-021-01973-5. BMC Gastroenterol. 2021. PMID: 34670529 Free PMC article.
-
Active tuberculosis in inflammatory bowel disease patients under treatment from an endemic area in Latin America.World J Gastroenterol. 2020 Nov 28;26(44):6993-7004. doi: 10.3748/wjg.v26.i44.6993. World J Gastroenterol. 2020. PMID: 33311945 Free PMC article.
References
-
- van Assche G, Vermeire S, Rutgeerts P. Mucosal healing and anti TNFs in IBD. Curr Drug Targets. 2010;11:227–233. - PubMed
-
- Yang SK, Yun S, Kim JH, Park JY, Kim HY, Kim YH, Chang DK, Kim JS, Song IS, Park JB, et al. Epidemiology of inflammatory bowel disease in the Songpa-Kangdong district, Seoul, Korea, 1986-2005: a KASID study. Inflamm Bowel Dis. 2008;14:542–549. - PubMed
-
- Lee KM, Jeen YT, Cho JY, Lee CK, Koo JS, Park DI, Im JP, Park SJ, Kim YS, Kim TO, et al. Efficacy, safety, and predictors of response to infliximab therapy for ulcerative colitis: a Korean multicenter retrospective study. J Gastroenterol Hepatol. 2013;28:1829–1833. - PubMed
-
- Ye BD, Yang SK, Shin SJ, Lee KM, Jang BI, Cheon JH, Choi CH, Kim YH, Lee H. [Guidelines for the management of Crohn’s disease] Korean J Gastroenterol. 2012;59:141–179. - PubMed
-
- Choi CH, Kim YH, Kim YS, Ye BD, Lee KM, Lee BI, Jung SA, Kim WH, Lee H. [Guidelines for the management of ulcerative colitis] Korean J Gastroenterol. 2012;59:118–140. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

