Prophylactic use of macrolide antibiotics for the prevention of chronic obstructive pulmonary disease exacerbation: a meta-analysis
- PMID: 25812085
- PMCID: PMC4374882
- DOI: 10.1371/journal.pone.0121257
Prophylactic use of macrolide antibiotics for the prevention of chronic obstructive pulmonary disease exacerbation: a meta-analysis
Abstract
Background: Acute exacerbations of chronic obstructive pulmonary disease (AECOPDs) can lead to high frequencies and rates of hospitalization and mortality. Macrolides are a class of antibiotics that possess both antimicrobial and anti-inflammatory properties. Since the occurrence of AECOPDs is associated with aggravation of airway inflammation and bacterial infections, prophylactic macrolide treatment may be an effective approach towards the prevention of AECOPDs.
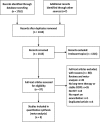
Methods: We systemically searched the PubMed, Embase and Cochrane Library databases to identify randomized controlled trials (RCTs) that evaluated the effect of prophylactic macrolide therapy on the prevention of AECOPDs. The primary outcomes were the total number of patients with one or more exacerbations as well as the rate of exacerbations per patient per year.
Results: Nine RCTs comprising 1666 patients met the inclusion criteria. Pooled evidence showed macrolides could reduce the frequency of exacerbations in patients with COPD by both unweighted (RR = 0.70; 95% CI: 0.56-0.87; P < 0.01) and weighted approaches (RR = 0.58, 95% CI: 0.43-0.78, P < 0.01). Subgroup analysis showed only 6-12 months of erythromycin or azithromycin therapy could be effective. Moreover, among studies with 6-12 months of azithromycin therapy, both the daily dosing regimen and the intermittent regimen significantly reduced exacerbation rates. The overall number of hospitalizations and the all-cause rate of death were not significantly different between the treatment and control groups. A tendency for more adverse events was found in the treatment groups (OR = 1.55, 95%CI: 1.003-2.39, P = 0.049).
Conclusions: Our results suggest 6-12 months erythromycin or azithromycin therapy could effectively reduce the frequency of exacerbations in patients with COPD. However, Long-term treatment may bring increased adverse events and the emergence of macrolide-resistance. A recommendation for the prophylactic use of macrolide therapy should weigh both the advantages and disadvantages.
Conflict of interest statement
Figures





References
-
- Mannino DM, Buist AS. Global burden of COPD: risk factors, prevalence, and future trends. Lancet. 2007;370: 765–773. - PubMed
-
- World Health Organization. Chronic obstructive pulmonary disease. Available: http://www.who.int/respiratory/copd/en/.
-
- Celli BR, MacNee W; ATS/ERS Task Force. Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS/ERS position paper. Eur Respir J. 2004;23: 932–946. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

