Mental Health Utilization in a Pediatric Emergency Department
- PMID: 25834957
- PMCID: PMC4526317
- DOI: 10.1097/PEC.0000000000000343
Mental Health Utilization in a Pediatric Emergency Department
Abstract
Objective: Mental health complaints are frequent in the pediatric emergency department (PED). The objective of this study was to describe trends over time in PED utilization for mental health care at in a single pediatric tertiary care hospital. It is our hypothesis that the resources used by this patient population are high and that mental health-related visits have increased over the most recent decade.
Methods: This was a retrospective study of all pediatric mental health presentations to the PED from January 2009 to July 2013 at a single pediatric hospital. All patients aged 1 to 19 years with an International Classification of Diseases, Ninth Revision code of 291, 292, 295 to 309, and 311 to 314 were included. Data collected included demographic data, medications received, restraint use, suicidality, length of stay (LOS), charges incurred, final disposition, and daily PED operation variables. Trends over time in presentation, charges, and LOS were analyzed using multiple mixed effects regression models after adjusting for potential patient and PED level confounding variables and clustering of multiple visits within patients.
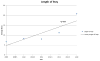
Results: A total of 732 PED visits from 2009 to 2013 were identified representing 646 unique patients. The average age was 13.8 years, and 53% were male. Approximately 25% of the patients expressed suicidal ideation, and 44% of those had attempted suicide before arrival. Behavioral or chemical restraints were used in 33% of patients during their PED visit. There were statistically significant increases in annual visits, LOS, and charges over this period (P < 0.05). Increased charges were significantly associated with longer LOS (P = 0.0062). Charges (P = 0.46) and LOS (P = 0.62) were not significantly different between suicidal and nonsuicidal patients. Approximately 21% of patients were admitted or transferred to another facility.
Conclusions: In this single-center study, we found evidence that the resources required to care for pediatric patients with mental health complaints have increased significantly over time both by increased number of annual visits and an increasing LOS. Further research is necessary to determine if our data are consistent with national trends to further our understanding of the problem and improve resource allocation.
Conflict of interest statement
The authors have no financial disclosures or conflicts of interest
Figures
References
-
- Friedman R, Katz-Leavy J, Manderscheid R, et al. Prevalence of serious emotional disturbance in children and adolescents. In: Manderscheid RW, Sonnenschein MA, editors. Mental Health, United States. Washington, DC: US Government Printing Office; 1996. pp. 77–112.
-
- Dolan MA, Fein JA Committee on Pediatric Emergency Medicine. Pediatric and adolescent mental health emergencies in the emergency medical services system. Pediatrics. 2011 May;127(5):e1356–66. - PubMed
-
- American Academy of Pediatrics; American College of Emergency Physicians. Dolan MA, Mace SE. Pediatric mental health emergencies in the emergency medical services system. American College of Emergency Physicians. Ann Emerg Med. 2006 Oct;48(4):484–6. - PubMed
-
- Sater N, Constantino JN. Pediatric emergencies in children with psychiatric conditions. Pediatr Emerg Care. 1998 Feb;14(1):42–50. - PubMed
-
- Christodulu KV, Lichenstein R, Weist MD, et al. Psychiatric emergencies in children. Pediatr Emerg Care. 2002 Aug;18(4):268–70. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources