Hospital costs of out-of-hospital cardiac arrest patients treated in intensive care; a single centre evaluation using the national tariff-based system
- PMID: 25838503
- PMCID: PMC4390724
- DOI: 10.1136/bmjopen-2014-005797
Hospital costs of out-of-hospital cardiac arrest patients treated in intensive care; a single centre evaluation using the national tariff-based system
Abstract
Objectives: There is a scarcity of literature reporting hospital costs for treating out of hospital cardiac arrest (OOHCA) survivors, especially within the UK. This is essential for assessment of cost-effectiveness of interventions necessary to allow just allocation of resources within the National Health Service. We set out primarily to calculate costs stratified against hospital survival and neurological outcomes. Secondarily, we estimated cost effectiveness based on estimates of survival and utility from previous studies to calculate costs per quality adjusted life year (QALY).
Setting: We performed a single centre (London) retrospective review of in-hospital costs of patients admitted to the intensive care unit (ICU) following return of spontaneous circulation (ROSC) after OOHCA over 18 months from January 2011 (following widespread introduction of targeted temperature management and primary percutaneous intervention).
Participants: Of 69 successive patients admitted over an 18-month period, survival and cerebral performance category (CPC) outcomes were obtained from review of databases and clinical notes. The Trust finance department supplied ICU and hospital costs using the Payment by Results UK system.
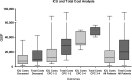
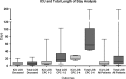
Results: Of those patients with ROSC admitted to ICU, survival to hospital discharge (any CPC) was 33/69 (48%) with 26/33 survivors in CPC 1-2 at hospital discharge. Cost per survivor to hospital discharge (including total cost of survivors and non-survivors) was £50,000, cost per CPC 1-2 survivor was £65,000. Cost and length of stay of CPC 1-2 patients was considerably lower than CPC 3-4 patients. The majority of the costs (69%) related to intensive care. Estimated cost per CPC 1-2 survivor per QALY was £16,000.
Conclusions: The costs of in-hospital patient care for ICU admissions following ROSC after OOHCA are considerable but within a reasonable threshold when assessed from a QALY perspective.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://group.bmj.com/group/rights-licensing/permissions.
Figures
Similar articles
-
Outcomes and healthcare-associated costs one year after intensive care-treated cardiac arrest.Resuscitation. 2018 Oct;131:128-134. doi: 10.1016/j.resuscitation.2018.06.028. Epub 2018 Jun 27. Resuscitation. 2018. PMID: 29958958
-
Neurological recovery after out-of-hospital cardiac arrest: hospital admission predictors and one-year survival in an urban cardiac network experience.Minerva Cardioangiol. 2013 Aug;61(4):451-60. Minerva Cardioangiol. 2013. PMID: 23846011
-
Effects of bystander CPR following out-of-hospital cardiac arrest on hospital costs and long-term survival.Resuscitation. 2017 Jun;115:129-134. doi: 10.1016/j.resuscitation.2017.04.016. Epub 2017 Apr 18. Resuscitation. 2017. PMID: 28427882
-
Economic aspects of severe sepsis: a review of intensive care unit costs, cost of illness and cost effectiveness of therapy.Pharmacoeconomics. 2004;22(12):793-813. doi: 10.2165/00019053-200422120-00003. Pharmacoeconomics. 2004. PMID: 15294012 Review.
-
Beyond return of spontaneous circulation: update on post-cardiac arrest management in the intensive care unit.Singapore Med J. 2021 Aug;62(8):444-451. doi: 10.11622/smedj.2021115. Singapore Med J. 2021. PMID: 35001117 Free PMC article. Review.
Cited by
-
Contemporary Management of Out-of-hospital Cardiac Arrest in the Cardiac Catheterisation Laboratory: Current Status and Future Directions.Interv Cardiol. 2019 Nov 18;14(3):113-123. doi: 10.15420/icr.2019.3.2. eCollection 2019 Nov. Interv Cardiol. 2019. PMID: 31867056 Free PMC article. Review.
-
Location of out-of-hospital cardiac arrests and automated external defibrillators in relation to schools in an English ambulance service region.Resusc Plus. 2022 Jul 26;11:100279. doi: 10.1016/j.resplu.2022.100279. eCollection 2022 Sep. Resusc Plus. 2022. PMID: 35911779 Free PMC article.
-
Role of bispectral index monitoring and burst suppression in prognostication following out-of-hospital cardiac arrest: a systematic review protocol.Syst Rev. 2017 Sep 25;6(1):191. doi: 10.1186/s13643-017-0584-6. Syst Rev. 2017. PMID: 28946920 Free PMC article.
-
Demographics and Clinical Features of Postresuscitation Comorbidities in Long-Term Survivors of Out-of-Hospital Cardiac Arrest: A National Follow-Up Study.Biomed Res Int. 2017;2017:9259182. doi: 10.1155/2017/9259182. Epub 2017 Feb 13. Biomed Res Int. 2017. PMID: 28286775 Free PMC article. Clinical Trial.
-
Cost-effectiveness of a novel smartphone application to mobilize first responders after witnessed OHCA in Belgium.Cost Eff Resour Alloc. 2020 Nov 17;18(1):52. doi: 10.1186/s12962-020-00248-2. Cost Eff Resour Alloc. 2020. PMID: 33292296 Free PMC article.
References
-
- McNally B, Robb R, Mehta M et al. . Out-of-hospital cardiac arrest surveillance- Cardiac Arrest Registry to Enhance Survival (CARES), United States, October 1, 2005-December 31, 2010. MMWR Surveill Summ 2011;60:1–19. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
