Psychological interventions for parents of children and adolescents with chronic illness
- PMID: 25874881
- PMCID: PMC4838404
- DOI: 10.1002/14651858.CD009660.pub3
Psychological interventions for parents of children and adolescents with chronic illness
Update in
-
Psychological interventions for parents of children and adolescents with chronic illness.Cochrane Database Syst Rev. 2019 Mar 18;3(3):CD009660. doi: 10.1002/14651858.CD009660.pub4. Cochrane Database Syst Rev. 2019. PMID: 30883665 Free PMC article.
Abstract
Background: Psychological therapies have been developed for parents of children and adolescents with a chronic illness. Such therapies include interventions directed at the parent only or at parent and child/adolescent, and are designed to improve parent, child, and family outcomes. This is an updated version of the original Cochrane review published in Issue 8, 2012, (Psychological interventions for parents of children and adolescents with chronic illness).
Objectives: To evaluate the efficacy of psychological therapies that include parents of children and adolescents with chronic illnesses including painful conditions, cancer, diabetes mellitus, asthma, traumatic brain injury (TBI), inflammatory bowel diseases (IBD), skin diseases, or gynaecological disorders. We also aimed to evaluate the adverse events related to implementation of psychological therapies for this population. Secondly, we aimed to evaluate the risk of bias of included studies and the quality of outcomes using the GRADE assessment.
Search methods: We searched the Cochrane Central Register of Controlled Trials (CENTRAL), MEDLINE, EMBASE and PsycINFO for randomised controlled trials (RCTs) of psychological interventions that included parents of children and adolescents with a chronic illness. Databases were searched to July 2014.
Selection criteria: Included studies were RCTs of psychological interventions that delivered treatment to parents of children and adolescents with a chronic illness compared to an active control, waiting list, or treatment as usual control group.
Data collection and analysis: Study characteristics and outcomes were extracted from included studies. We analysed data using two categories. First, we analysed data by each individual medical condition collapsing across all treatment classes at two time points. Second, we analysed data by each individual treatment class; cognitive behavioural therapy (CBT), family therapy (FT), problem solving therapy (PST) and multisystemic therapy (MST) collapsing across all medical conditions. For both sets of analyses we looked immediately post-treatment and at the first available follow-up. We assessed treatment effectiveness for two primary outcomes: parent behaviour and parent mental health. Five secondary outcomes were extracted; child behaviour/disability, child mental health, child symptoms, family functioning, and adverse events. Risk of bias and quality of evidence were assessed.
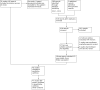
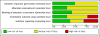
Main results: Thirteen studies were added in this update, giving a total of 47 RCTs. The total number of participants included in the data analyses was 2985, 804 of whom were added to the analyses in the update. The mean age of the children was 14.6 years. Of the 47 RCTs, the studies focused on the following paediatric conditions: n = 14 painful conditions, n = 13 diabetes, n =10 cancer, n = 5 asthma, n = 4 TBI, and n = 1 atopic eczema. We did not identify any studies treating parents of children with gynaecological disorders or IBD. Risk of bias assessments of included studies were predominantly unclear. Evidence quality, assessed using the GRADE criteria, was judged to be of low or very low quality.Analyses of separate medical conditions, across all treatment types, revealed two beneficial effects of psychological therapies for our primary outcomes. First, psychological therapies led to improved adaptive parenting behaviour in parents of children with cancer post-treatment (standardised mean difference (SMD) -0.20, 95% confidence interval (CI) -0.36 to -0.04, Z = 2.44, p = 0.01). In addition, therapies also improved parent mental health at follow-up in this group (SMD = -0.18, 95% CI -0.32 to -0.04, Z = 2.58, p = 0.01). We did not find any effect of therapies for parent behaviour for parents of children with a painful condition post-treatment or at follow-up, or for parent mental health for parents of children with cancer, diabetes, asthma, or TBI post-treatment. For all other primary outcomes, no analysis could be conducted due to lack of data.Across all medical conditions, three effects were found for the primary outcomes of psychological therapies. PST had a beneficial effect on parent adaptive behaviour (SMD = -0.25, 95% CI -0.39 to -0.11, Z = 3.59, p < 0.01) and parent mental health (SMD= -0.24, 95% CI -0.42 to -0.05, Z = 2.50, p = 0.01) immediately post-treatment and this effect was maintained at follow-up for parent mental health (SMD= -0.19, 95% CI -0.34 to -0.04, Z = 2.55, p = 0.01). The remaining analysis for PST on parent behaviour found no effect. No effects were found for CBT post-treatment or at follow-up for either parent outcome. For FT, only one analysis could be run on parent mental health and no effect was found. Due to lack of data, the remaining analyses of primary outcomes could not be run. For MST, no parent outcomes could be analysed due to lack of data.Secondary outcome analyses are presented in the Results section. Five studies reported that there were no adverse events during the trial. The remaining 42 studies did not report adverse events.
Authors' conclusions: This update includes 13 additional studies, although our conclusions have not changed from the original version. There is little evidence for the efficacy of psychological therapies that include parents on most outcome domains of functioning, for a large number of common chronic illnesses in children. However, psychological therapies are efficacious for some outcomes. CBT that includes parents is beneficial for reducing children's primary symptoms, and PST that includes parents improved parent adaptive behaviour and parent mental health. There is evidence that the beneficial effects can be maintained at follow-up for diabetes-related symptoms in children, and for the mental health of parents of children with cancer and parents who received PST.
Conflict of interest statement
CE, EF, EL, JB, and TP have no relevant declarations of interest.
For transparency we declare that we have received research support from charity, government, and industry sources at various times, but none relate to this review.
Figures




















































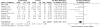
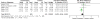
Update of
-
Psychological interventions for parents of children and adolescents with chronic illness.Cochrane Database Syst Rev. 2012 Aug 15;8(8):CD009660. doi: 10.1002/14651858.CD009660.pub2. Cochrane Database Syst Rev. 2012. Update in: Cochrane Database Syst Rev. 2015 Apr 15;(4):CD009660. doi: 10.1002/14651858.CD009660.pub3. PMID: 22895990 Free PMC article. Updated.
References
References to studies included in this review
-
- Allen KD, Shriver MD. Role of parent-mediated pain behavior management strategies in biofeedback treatment of childhood migraines. Behaviour Therapy. 1998;29:477–90.
-
- Antonini TN, Raj SP, Oberjohn KS, Cassedy A, Makoroff KL, Fouladi M, et al. Pilot randomized trial of an online parenting skills program for pediatric traumatic brain injury: improvements in parenting and child behavior. Behavior Therapy. 2014;45(4):455–68. - PubMed
-
- Askins MA, Sahler OJ, Sherman SA, Fairclough DL, Butler RW, Katz ER, et al. Report from a multi-institutional randomized clinical trial examining computer-assisted problem-solving skills training for English- and Spanish-speaking mothers of children with newly diagnosed cancer. Journal of Pediatric Psychology. 2008;34(5):551–63. - PMC - PubMed
References to studies excluded from this review
-
- Aleman Mendez S, Palacios AS. An integrated approach to the psychological features of the asthmatic child [Un adordaje integral de los aspectos psicologicos del niño asmatico] Allergologia et Immunopathologia. 1992;20(6):240–5. - PubMed
-
- Anderson BJ, Ho J, Brackett J, Laffel LMB. An office-based intervention to maintain parent-adolescent teamwork in diabetes management: impact on parent involvement, family conflict, and subsequent glycemic control. Diabetes Care. 1999;22(7):713–21. - PubMed
-
- Betancourt GP, Gutierrez de Pineres Scarpetta C. Psychological intervention pre-postsurgical program for cardiovascular pediatric patients. Saludarte. 2004;3(11):19–34.
Additional references
-
- American Psychological Association. Publication Manual of the American Psychological Association. Washington: American Psychological Association; 2011.
-
- Armour TA, Norris SL, Jack L, Jr, Zhang X, Fisher L. The effectiveness of family interventions in people with diabetes mellitus: a systematic review. Diabetic Medicine. 2005;22(10):1295–305. - PubMed
-
- Ashby FG, Isen AM, Turken AU. A neuropsychological theory of positive affect and its influence on cognition. Psychological Review. 1999;106(3):529–50. - PubMed
-
- Bandura A. Social Learning Theory. New Jersey: Prentice-Hall; 1977.
References to other published versions of this review
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

