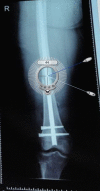
Treatment With the SIGN Nail in Closed Diaphyseal Femur Fractures Results in Acceptable Radiographic Alignment
- PMID: 25894807
- PMCID: PMC4457748
- DOI: 10.1007/s11999-015-4290-1
Treatment With the SIGN Nail in Closed Diaphyseal Femur Fractures Results in Acceptable Radiographic Alignment
Abstract
Background: The burden of orthopaedic trauma in the developing world is substantial and disproportionate. SIGN Fracture Care International is a nonprofit organization that has developed and made available to surgeons in resource-limited settings an intramedullary interlocking nail for use in the treatment of femoral and tibial fractures. Instrumentation also is donated with the nail. A prospectively populated database collects information on all procedures performed using this nail. Given the challenging settings and numerous surgeons with varied experience, it is important to document adequate alignment and union using the device.
Questions/purposes: The primary aim of this research was to assess the adequacy of operative reduction of closed diaphyseal femur fractures using the SIGN interlocking intramedullary nail based on radiographic images available in the SIGN database. The secondary aims were to assess correlations between postoperative alignment and several associated variables, including fracture location in the diaphysis, degree of fracture site comminution, and time to surgery. The tertiary aim was to assess the functionality of the SIGN database for radiographic analyses.
Methods: A review of the prospectively populated SIGN database was performed for patients with a diaphyseal femur fracture treated with the SIGN nail, which at the time of the study totaled 32,362 patients. After study size calculations, a random number generator was used to select 500 femur fractures for analysis. Exclusion criteria included open fractures and those without radiographs during the early postoperative period. The following information was recorded: location of the fracture in the diaphysis; fracture classification (AO/Orthopaedic Trauma Association [OTA] classification); degree of comminution (Winquist and Hansen classification); time from injury to surgery; and patient demographics. Measurements of alignment were obtained from the AP and lateral radiographs with malalignment defined as deformity in either the sagittal or coronal plane greater than 5°. Measurements were made manually by the four study authors using on-screen protractor software and interobserver reliability was assessed.
Results: The frequency of malalignment greater than 5° observed on postoperative radiographs was 51 of 501 (10%; 95% CI, 6.5-11.5), and malalignment greater than 10° occurred in eight of 501 (1.6%) of the femurs treated with this nail. Fracture location in the proximal or distal diaphysis was strongly correlated with risk of malalignment, with an odds ratio (OR) of 3.7 (95% CI, 1.5-9.3) for distal versus middle diaphyseal fractures and an OR of 4.7 (95% CI, 1.9-11.5) for proximal versus middle fractures (p < 0.001). Time from injury to surgery greater than 4 weeks also was strongly correlated with risk of malalignment (p < 0.001). Inherent fracture stability, based on fracture site comminution as per the Winquist and Hansen classification (Class 0-1 stable versus 2-4 unstable) showed an OR of 2.3 (95% CI, 1.2-4.3) for malalignment in unstable fractures. Interobserver reliability showed agreement of 88% (95% CI, 83-93) and mean kappa of 0.81 (95% CI, 0.65-0.87). The SIGN database of radiographic images was found to be an excellent source for research purposes with 92% of reviewed radiographs of acceptable quality.
Conclusions: The frequency of malalignment in closed diaphyseal femoral fractures treated with the SIGN nail closely approximated the incidence reported in the literature for North American trauma centers. Increased time from injury to surgery was correlated with increased frequency of malalignment; as humanitarian distribution of the SIGN nail increases, local barriers to timely care should be assessed and improved as possible. Prospective clinical study with followup, despite its inherent challenges in the developing world, would be of great benefit in the future.
Level of evidence: Level III, therapeutic study.
Figures
References
-
- Beveridge M, Howard A. The burden of orthopaedic disease in developing countries. J Bone Joint Surg Am. 2004;86:1819–1822. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials