Race, Relationship and Renal Diagnoses After Living Kidney Donation
- PMID: 25905980
- PMCID: PMC4663050
- DOI: 10.1097/TP.0000000000000733
Race, Relationship and Renal Diagnoses After Living Kidney Donation
Abstract
Background: In response to recent studies, a better understanding of the risks of renal complications among African American and biologically related living kidney donors is needed.
Methods: We examined a database linking U.S. registry identifiers for living kidney donors (1987-2007) to billing claims from a private health insurer (2000-2007 claims) to identify renal condition diagnoses categorized by International Classification of Diseases 9th Revision coding. Cox regression with left and right censoring was used to estimate cumulative incidence of diagnoses after donation and associations (adjusted hazards ratios, aHR) with donor traits.
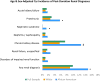
Results: Among 4650 living donors, 13.1% were African American and 76.3% were white; 76.1% were first-degree relatives of their recipient. By 7 years post-donation, after adjustment for age and sex, greater proportions of African American compared with white donors had renal condition diagnoses: chronic kidney disease (12.6% vs 5.6%; aHR, 2.32; 95% confidence interval [95% CI], 1.48-3.62), proteinuria (5.7% vs 2.6%; aHR, 2.27; 95% CI, 1.32-3.89), nephrotic syndrome (1.3% vs 0.1%; aHR, 15.7; 95% CI, 2.97-83.0), and any renal condition (14.9% vs 9.0%; aHR, 1.72; 95% CI, 1.23-2.41). Although first-degree biological relationship to the recipient was not associated with renal risk, associations of African American race persisted for these conditions and included unspecified renal failure and reported disorders of kidney dysfunction after adjustment for biological donor-recipient relationship.
Conclusions: African Americans more commonly develop renal conditions after living kidney donation, independent of donor-recipient relationship. Continued research is needed to improve risk stratification for renal outcomes among African American living donors.
Conflict of interest statement
Disclosures: The authors have no conflicts of interest related to this work.
Figures
Comment in
-
Living Kidney Donor Outcomes--More Pieces to the Jigsaw.Transplantation. 2015 Aug;99(8):1547-8. doi: 10.1097/TP.0000000000000732. Transplantation. 2015. PMID: 26193066 No abstract available.
Similar articles
-
Gout after living kidney donation: correlations with demographic traits and renal complications.Am J Nephrol. 2015;41(3):231-40. doi: 10.1159/000381291. Epub 2015 Apr 17. Am J Nephrol. 2015. PMID: 25896309 Free PMC article.
-
Living Kidney Donor Outcomes--More Pieces to the Jigsaw.Transplantation. 2015 Aug;99(8):1547-8. doi: 10.1097/TP.0000000000000732. Transplantation. 2015. PMID: 26193066 No abstract available.
-
Hospitalizations following living donor nephrectomy in the United States.Clin J Am Soc Nephrol. 2014 Feb;9(2):355-65. doi: 10.2215/CJN.03820413. Epub 2014 Jan 23. Clin J Am Soc Nephrol. 2014. PMID: 24458071 Free PMC article.
-
Health outcomes among non-Caucasian living kidney donors: knowns and unknowns.Transpl Int. 2013 Sep;26(9):853-64. doi: 10.1111/tri.12088. Epub 2013 Mar 27. Transpl Int. 2013. PMID: 23531054 Review.
-
Risks and outcomes of living donation.Adv Chronic Kidney Dis. 2012 Jul;19(4):220-8. doi: 10.1053/j.ackd.2011.09.005. Adv Chronic Kidney Dis. 2012. PMID: 22732041 Free PMC article. Review.
Cited by
-
KDIGO Clinical Practice Guideline on the Evaluation and Care of Living Kidney Donors.Transplantation. 2017 Aug;101(8S Suppl 1):S1-S109. doi: 10.1097/TP.0000000000001769. Transplantation. 2017. PMID: 28742762 Free PMC article.
-
Eliminating Race From eGFR Calculations: Impact on Living Donor Programs.Transpl Int. 2022 Nov 11;35:10787. doi: 10.3389/ti.2022.10787. eCollection 2022. Transpl Int. 2022. PMID: 36438782 Free PMC article. No abstract available.
-
Risks for donors associated with living kidney donation: meta-analysis.Br J Surg. 2022 Jul 15;109(8):671-678. doi: 10.1093/bjs/znac114. Br J Surg. 2022. PMID: 35612960 Free PMC article.
-
One size does not fit all: understanding individual living kidney donor risk.Pediatr Nephrol. 2021 Feb;36(2):259-269. doi: 10.1007/s00467-019-04456-8. Epub 2020 Jan 2. Pediatr Nephrol. 2021. PMID: 31897715 Free PMC article. Review.
-
The Association between Body Composition Measurements and Surgical Complications after Living Kidney Donation.J Clin Med. 2021 Jan 5;10(1):155. doi: 10.3390/jcm10010155. J Clin Med. 2021. PMID: 33466272 Free PMC article.
References
-
- OTPN/HRSA. National Data, Transplants by Donor Type. [Access date: october 7, 2014]; http://optn.transplant.hrsa.gov/converge/latestData/rptData.asp.
-
- OPTN (Organ Procurement and Transplantation Network) and SRTR (Scientific Registry of Transplant Recipients) Department of Health and Human Services, Health Resources and Services Administration, Healthcare Systems Bureau, Division of Transplantation; [Access date: october 7, 2014]. OPTN / SRTR 2012 Annual Data Report. Kidney Chapter/Live Donation. Available at: http://srtr.transplant.hrsa.gov/annual_reports/2012/pdf/01_kidney_13.pdf.
-
- Lentine KL, Segev DL. Health outcomes among non-Caucasian living kidney donors: knowns and unknowns. Transpl Int. 2013;26(9):853. - PubMed
-
- Ommen ES, Winston JA, Murphy B. Medical risks in living kidney donors: absence of proof is not proof of absence. Clin J Am Soc Nephrol. 2006;1(4):885. - PubMed
-
- Ommen ES, LaPointe Rudow D, Medapalli RK, Schroppel B, Murphy B. When good intentions are not enough: obtaining follow-up data in living kidney donors. Am J Transplant. 2011;11(12):2575. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

