The learning curve for robotic distal pancreatectomy: an analysis of outcomes of the first 100 consecutive cases at a high-volume pancreatic centre
- PMID: 25906690
- PMCID: PMC4474504
- DOI: 10.1111/hpb.12412
The learning curve for robotic distal pancreatectomy: an analysis of outcomes of the first 100 consecutive cases at a high-volume pancreatic centre
Abstract
Background: Robotic distal pancreatectomy (RDP) is performed increasingly, but knowledge of the number of cases required to attain procedural proficiency is lacking. The aim of this study was to identify the learning curve associated with RDP at a high-volume pancreatic centre.
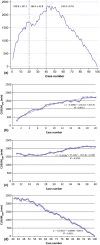
Methods: Metrics of perioperative safety and efficiency for all consecutive RDPs were evaluated. Outcomes were followed to 90 days. Cumulative sum (CUSUM) analysis was used to identify inflexion points corresponding to the learning curve.
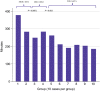
Results: Between 2008 and 2013, 100 patients underwent RDP. There was no 90-day mortality. In two patients (2.0%), surgery was converted to laparotomy. Thirty procedures were performed for pancreatic adenocarcinoma. Precipitous operative time reductions from an initial operative time of 331 min were observed after the first 20 and 40 cases to 266 min and 210 min, respectively (P < 0.0001). The likelihood of readmission was significantly lower after the first 40 cases (P = 0.04), and non-significant reductions were observed in incidences of major (Clavien-Dindo Grade II or higher) morbidity and Grade B and C leaks, and length of stay.
Conclusions: In this experience, RDP outcomes were optimized after 40 cases. Familiarity with the platform and dedicated training are likely to contribute to significantly shorter learning curves in future adopters.
© 2015 International Hepato-Pancreato-Biliary Association.
Figures

References
-
- Merchant NB, Parikh AA, Kooby DA. Should all distal pancreatectomies be performed laparoscopically? Adv Surg. 2009;43:283–300. - PubMed
-
- Magge D, Gooding W, Choudry H, Steve J, Steel J, Zureikat A, et al. Comparative effectiveness of minimally invasive and open distal pancreatectomy for ductal adenocarcinoma. JAMA Surg. 2013;148:525–531. - PubMed
-
- Kooby DA, Hawkins WG, Schmidt CM, Weber SM, Bentrem DJ, Gillespie TW, et al. A multicenter analysis of distal pancreatectomy for adenocarcinoma: is laparoscopic resection appropriate? J Am Coll Surg. 2010;210:779–785. discussion 786–787. - PubMed
-
- Kim SC, Park KT, Hwang JW, Shin HC, Lee SS, Seo DW, et al. Comparative analysis of clinical outcomes for laparoscopic distal pancreatic resection and open distal pancreatic resection at a single institution. Surg Endosc. 2008;22:2261–2268. - PubMed
-
- Jayaraman S, Gonen M, Brennan MF, D'Angelica MI, DeMatteo RP, Fong Y, et al. Laparoscopic distal pancreatectomy: evolution of a technique at a single institution. J Am Coll Surg. 2010;211:503–509. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

