Straylight, lens yellowing and aberrations of eyes in Type 1 diabetes
- PMID: 25909012
- PMCID: PMC4399667
- DOI: 10.1364/BOE.6.001282
Straylight, lens yellowing and aberrations of eyes in Type 1 diabetes
Abstract
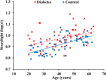
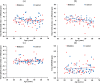
Straylight, lens yellowing and ocular aberrations were assessed in a group of people with type 1 diabetes and in an age matched control group. Most of the former had low levels of neuropathy. Relative to the control group, the type 1 diabetes group demonstrated greater straylight, greater lens yellowing, and differences in some higher-order aberration co-efficients without significant increase in root-mean-square higher-order aberrations. Differences between groups did not increase significantly with age. The results are similar to the findings for ocular biometry reported previously for this group of participants, and suggest that age-related changes in the optics of the eyes of people with well-controlled diabetes need not be accelerated.
Keywords: (330.4875) Optics of physiological systems; (330.7329) Visual optics, pathology.
Figures

References
LinkOut - more resources
Full Text Sources
