Radiofrequency Ablation Is Associated With Decreased Neoplastic Progression in Patients With Barrett's Esophagus and Confirmed Low-Grade Dysplasia
- PMID: 25917785
- PMCID: PMC4550488
- DOI: 10.1053/j.gastro.2015.04.013
Radiofrequency Ablation Is Associated With Decreased Neoplastic Progression in Patients With Barrett's Esophagus and Confirmed Low-Grade Dysplasia
Abstract
Background & aims: Barrett's esophagus (BE) with low-grade dysplasia (LGD) can progress to high-grade dysplasia (HGD) and esophageal adenocarcinoma (EAC). Radiofrequency ablation (RFA) has been shown to be an effective treatment for LGD in clinical trials, but its effectiveness in clinical practice is unclear. We compared the rate of progression of LGD after RFA with endoscopic surveillance alone in routine clinical practice.
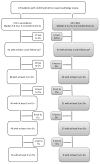
Methods: We performed a retrospective study of patients who either underwent RFA (n = 45) or surveillance endoscopy (n = 125) for LGD, confirmed by at least 1 expert pathologist, from October 1992 through December 2013 at 3 medical centers in the United States. Cox regression analysis was used to assess the association between progression and RFA.
Results: Data were collected over median follow-up periods of 889 days (interquartile range, 264-1623 days) after RFA and 848 days (interquartile range, 322-2355 days) after surveillance endoscopy (P = .32). The annual rates of progression to HGD or EAC were 6.6% in the surveillance group and 0.77% in the RFA group. The risk of progression to HGD or EAC was significantly lower among patients who underwent RFA than those who underwent surveillance (adjusted hazard ratio = 0.06; 95% confidence interval: 0.008-0.48).
Conclusions: Among patients with BE and confirmed LGD, rates of progression to a combined end point of HGD and EAC were lower among those treated with RFA than among untreated patients. Although selection bias cannot be excluded, these findings provide additional evidence for the use of endoscopic ablation therapy for LGD.
Keywords: Clinical Setting; Eradication; Esophageal Cancer; Prevention.
Copyright © 2015 AGA Institute. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
The authors have no personal or financial conflicts of interest in any content or products mentioned in this manuscript.
Figures
References
-
- Rasool S, Ganai AB, Syed Sameer A, et al. Esophageal cancer: associated factors with special reference to the Kashmir Valley. Tumori. 2012;98:191–203. - PubMed
-
- Spechler SJ, Sharma P, Souza RF, et al. American Gastroenterological Association medical position statement on the management of Barrett’s esophagus. Gastroenterology. 2011;140:1084–1091. - PubMed
-
- Wani S, Mathur S, Sharma P. How to manage a Barrett’s esophagus patient with low-grade dysplasia. Clin Gastroenterol Hepatol. 2009;7:27–32. - PubMed
Publication types
MeSH terms
Supplementary concepts
Grants and funding
- 1 K08 DK084347-01/DK/NIDDK NIH HHS/United States
- K24 DK078228/DK/NIDDK NIH HHS/United States
- P30 DK050306/DK/NIDDK NIH HHS/United States
- T32 DK007740/DK/NIDDK NIH HHS/United States
- U54-CA163004/CA/NCI NIH HHS/United States
- K08 DK084347/DK/NIDDK NIH HHS/United States
- P01-CA098101/CA/NCI NIH HHS/United States
- P01 CA098101/CA/NCI NIH HHS/United States
- K23 DK090209/DK/NIDDK NIH HHS/United States
- P30 CA015083/CA/NCI NIH HHS/United States
- P30 CA016520/CA/NCI NIH HHS/United States
- P30 DK084567/DK/NIDDK NIH HHS/United States
- P30DK050306/DK/NIDDK NIH HHS/United States
- P50 CA127003/CA/NCI NIH HHS/United States
- K24-DK078228/DK/NIDDK NIH HHS/United States
- U54 CA163004/CA/NCI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical