Central venous-to-arterial carbon dioxide difference as a prognostic tool in high-risk surgical patients
- PMID: 25967737
- PMCID: PMC4486687
- DOI: 10.1186/s13054-015-0917-6
Central venous-to-arterial carbon dioxide difference as a prognostic tool in high-risk surgical patients
Abstract
Introduction: The purpose of this study was to evaluate the clinical relevance of high values of central venous-to-arterial carbon dioxide difference (PCO2 gap) in high-risk surgical patients admitted to a postoperative ICU. We hypothesized that PCO2 gap could serve as a useful tool to identify patients still requiring hemodynamic optimization at ICU admission.
Methods: One hundred and fifteen patients were included in this prospective single-center observational study during a 1-year period. High-risk surgical inclusion criteria were adapted from Schoemaker and colleagues. Demographic and biological data, PCO2 gap, central venous oxygen saturation, lactate level and postoperative complications were recorded for all patients at ICU admission, and 6 hours and 12 hours after admission.
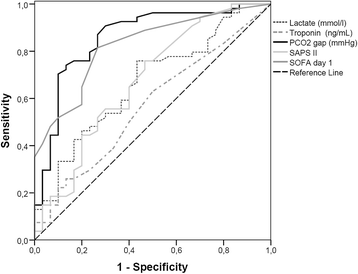
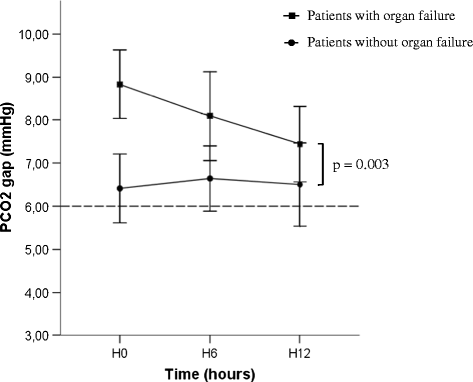
Results: A total of 78 (68%) patients developed postoperative complications, of whom 54 (47%) developed organ failure. From admission to 12 hours after admission, there was a significant difference in mean PCO2 gap (8.7 ± 2.8 mmHg versus 5.1 ± 2.6 mmHg; P = 0.001) and median lactate values (1.54 (1.1-3.2) mmol/l versus 1.06 (0.8-1.8) mmol/l; P = 0.003) between patients who developed postoperative complications and those who did not. These differences were maximal at admission to the ICU. At ICU admission, the area under the receiver operating characteristic curve for occurrence of postoperative complications was 0.86 for the PCO2 gap compared to Sequential Organ Failure Assessment score (0.82), Simplified Acute Physiology Score II score (0.67), and lactate level (0.67). The threshold value for PCO2 gap was 5.8 mmHg. Multivariate analysis showed that only a high PCO2 gap and a high Sequential Organ Failure Assessment score were independently associated with the occurrence of postoperative complications. A high PCO2 gap (≥6 mmHg) was associated with more organ failure, an increase in duration of mechanical ventilation and length of hospital stay.
Conclusion: A high PCO2 gap at admission in the postoperative ICU was significantly associated with increased postoperative complications in high-risk surgical patients. If the increase in PCO2 gap is secondary to tissue hypoperfusion then the PCO2 gap might be a useful tool complementary to central venous oxygen saturation as a therapeutic target.
Figures

Comment in
-
Nachrichten aus der internationalen Fachliteratur.Anasthesiol Intensivmed Notfallmed Schmerzther. 2016 Jan;51(1):4-6. doi: 10.1055/s-0041-109183. Epub 2016 Feb 9. Anasthesiol Intensivmed Notfallmed Schmerzther. 2016. PMID: 26859468 German. No abstract available.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

