A population-based study comparing patterns of care delivery on the quality of care for persons living with HIV in Ontario
- PMID: 25971708
- PMCID: PMC4431060
- DOI: 10.1136/bmjopen-2014-007428
A population-based study comparing patterns of care delivery on the quality of care for persons living with HIV in Ontario
Abstract
Objectives: Physician specialty is often positively associated with disease-specific outcomes and negatively associated with primary care outcomes for people with chronic conditions. People with HIV have increasing comorbidity arising from antiretroviral therapy (ART) related longevity, making HIV a useful condition to examine shared care models. We used a previously described, theoretically developed shared care framework to assess the impact of care delivery on the quality of care provided.
Design: Retrospective population-based observational study from 1 April 2009 to 31 March 2012.
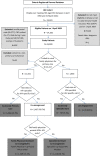
Participants: 13 480 patients with HIV and receiving publicly funded healthcare in Ontario were assigned to one of five patterns of care.
Outcome measures: Cancer screening, ART prescribing and healthcare utilisation across models using adjusted multivariable hierarchical logistic regression analyses.
Results: Models in which patients had an assigned family physician had higher odds of cancer screening than those in exclusively specialist care (colorectal cancer screening, exclusively primary care adjusted OR (AOR)=3.12, 95% CI (1.90 to 5.13), family physician-dominant co-management AOR=3.39, 95% CI (1.94 to 5.93), specialist-dominant co-management AOR=2.01, 95% CI (1.23 to 3.26)). The odds of having one emergency department visit did not differ among models, although the odds of hospitalisation and HIV-specific hospitalisation were lower among patients who saw exclusively family physicians (AOR=0.23, 95% CI (0.14 to 0.35) and AOR=0.15, 95% CI (0.12 to 0.21)). The odds of antiretroviral prescriptions were lower among models in which patients' HIV care was provided predominantly by family physicians (exclusively primary care AOR=0.15, 95% CI (0.12 to 0.21), family physician-dominant co-management AOR=0.45, 95% CI (0.32 to 0.64)).
Conclusions: How care is provided had a potentially important influence on the quality of care delivered. Our key limitation is potential confounding due to the absence of HIV stage measures.
Keywords: Human Immunodeficiency Virus; PRIMARY CARE; chronic disease; comorbidity; health services delivery.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://group.bmj.com/group/rights-licensing/permissions.
Figures
Similar articles
-
A population-based study evaluating family physicians' HIV experience and care of people living with HIV in Ontario.Ann Fam Med. 2015 Sep;13(5):436-45. doi: 10.1370/afm.1822. Ann Fam Med. 2015. PMID: 26371264 Free PMC article.
-
Health administrative data can be used to define a shared care typology for people with HIV.J Clin Epidemiol. 2015 Nov;68(11):1301-11. doi: 10.1016/j.jclinepi.2015.02.008. Epub 2015 Feb 21. J Clin Epidemiol. 2015. PMID: 25835491
-
A cohort study examining emergency department visits and hospital admissions among people who use drugs in Ottawa, Canada.Harm Reduct J. 2017 May 12;14(1):16. doi: 10.1186/s12954-017-0143-4. Harm Reduct J. 2017. PMID: 28494791 Free PMC article.
-
Finding the Value in Value-Based Care.Ann Thorac Surg. 2021 Jul;112(1):16-21. doi: 10.1016/j.athoracsur.2021.03.045. Epub 2021 Mar 29. Ann Thorac Surg. 2021. PMID: 33794158 Review. No abstract available.
-
Hospital mortality: when failure is not a good measure of success.CMAJ. 2008 Jul 15;179(2):153-7. doi: 10.1503/cmaj.080010. CMAJ. 2008. PMID: 18625987 Free PMC article. Review. No abstract available.
Cited by
-
Understanding Care Linkage and Engagement Across 15 Adolescent Clinics: Provider Perspectives and Implications for Newly HIV-Infected Youth.AIDS Educ Prev. 2017 Apr;29(2):93-104. doi: 10.1521/aeap.2017.29.2.93. AIDS Educ Prev. 2017. PMID: 28467164 Free PMC article.
-
Structural Barriers to Primary Care Among Sex Workers: Findings from a Community- Based Cohort in Vancouver, Canada (2014-2021).Res Sq [Preprint]. 2024 Aug 28:rs.3.rs-4802645. doi: 10.21203/rs.3.rs-4802645/v1. Res Sq. 2024. Update in: BMC Health Serv Res. 2025 Jan 24;25(1):134. doi: 10.1186/s12913-025-12275-x. PMID: 39257992 Free PMC article. Updated. Preprint.
-
HPV self-sampling: A promising approach to reduce cervical cancer screening disparities in Canada.Curr Oncol. 2018 Feb;25(1):13-18. doi: 10.3747/co.25.3845. Epub 2018 Feb 28. Curr Oncol. 2018. PMID: 29507479 Free PMC article. No abstract available.
-
Non-Communicable Disease Preventive Screening by HIV Care Model.PLoS One. 2017 Jan 6;12(1):e0169246. doi: 10.1371/journal.pone.0169246. eCollection 2017. PLoS One. 2017. PMID: 28060868 Free PMC article.
-
Cost-effectiveness of self-sampling and enhanced strategies for HPV prevention among men who have sex with men in China: a modeling study.BMC Med. 2025 Jul 1;23(1):362. doi: 10.1186/s12916-025-04131-w. BMC Med. 2025. PMID: 40597274 Free PMC article.
References
-
- Jaakkimainen L, Schultz SE, Klein-Geltink J et al. . Ambulatory physician care for adults. In: Jaakkimainen L, Upshur R, Klein-Geltink J, Leong A, Maaten S, Schultz S, eds. Primary care in Ontario: ICES atlas. Toronto: Institute for Clinical Evaluative Sciences, 2006:53–76.
-
- Katz A, Martens P, Chateau D et al. . Understanding the health system use of ambulatory care patients. Winnipeg, MB: Manitoba Centre for Health Policy, Department of Community Health Sciences, Faculty of Medicine, University of Manitoba; (Beaconsfield, Quebec: Canadian Electronic Library, 2013).
-
- Smith SM, Allwright S, O'Dowd T. Does sharing care across the primary-specialty interface improve outcomes in chronic disease? A systematic review. Am J Manag Care 2008;14:213–24. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous