Enalapril Normalizes Endothelium-Derived Hyperpolarizing Factor-Mediated Relaxation in Mesenteric Artery of Adult Hypertensive Rats Prenatally Exposed to Testosterone
- PMID: 25972013
- PMCID: PMC4652613
- DOI: 10.1095/biolreprod.115.130468
Enalapril Normalizes Endothelium-Derived Hyperpolarizing Factor-Mediated Relaxation in Mesenteric Artery of Adult Hypertensive Rats Prenatally Exposed to Testosterone
Abstract
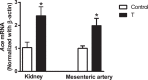
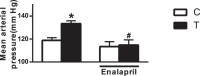
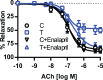
Prenatal exposure to elevated testosterone levels induces adult life hypertension associated with selective impairments in endothelium-derived hyperpolarizing factor (EDHF)-mediated relaxation in mesenteric arteries. We tested whether the angiotensin-converting enzyme inhibitor enalapril restores EDHF function through regulating the activities of small (Kcnn3) and intermediate (Kcnn4) conductance calcium-activated potassium channels in mesenteric arteries. Pregnant Sprague-Dawley rats were injected subcutaneously with vehicle or testosterone propionate (0.5 mg/kg/day from Gestation Day 15 to 19), and their 6-mo-old adult male offspring were examined. A subset of rats in these two groups was given enalapril (40 mg/kg/day) for 2 wk through drinking water. Blood pressures were assessed through carotid arterial catheter and endothelium-dependent mesenteric arterial EDHF relaxation, using wire myography. Ace and Kcnn3 and Kcnn4 channel expression levels were also examined. Renal and vascular Ace expression and plasma angiotensin II levels were increased in testosterone offspring. Blood pressure levels were significantly higher in testosterone offspring than in controls, and treatment with enalapril significantly attenuated blood pressure in testosterone offspring. EDHF relaxation in testosterone offspring was reduced compared to that in controls, and it was significantly restored by enalapril treatment. Kcnn4 channel expression and function were similar between control and testosterone rats, but it was not affected by enalapril treatment. Relaxation mediated by Kcnn3 was impaired in testosterone offspring, and it was normalized by enalapril treatment. Furthermore, enalapril treatment restored expression levels of Kcnn3 channels. These findings suggest that enalapril has a positive influence on endothelial function with improvement in EDHF relaxation through normalization of Kcnn3 expression and activity.
Keywords: EDHF; Kcnn3 channel; blood pressure; enalapril; endothelium; mesenteric arteries; pregnancy; testosterone.
© 2015 by the Society for the Study of Reproduction, Inc.
Figures




Similar articles
-
Prenatal testosterone induces sex-specific dysfunction in endothelium-dependent relaxation pathways in adult male and female rats.Biol Reprod. 2013 Oct 24;89(4):97. doi: 10.1095/biolreprod.113.111542. Print 2013 Oct. Biol Reprod. 2013. PMID: 23966325 Free PMC article.
-
Enalapril treatment alters the contribution of epoxyeicosatrienoic acids but not gap junctions to endothelium-derived hyperpolarizing factor activity in mesenteric arteries of spontaneously hypertensive rats.J Pharmacol Exp Ther. 2009 Aug;330(2):413-22. doi: 10.1124/jpet.109.152116. Epub 2009 May 1. J Pharmacol Exp Ther. 2009. PMID: 19411610 Free PMC article.
-
Altered myogenic constriction and endothelium-derived hyperpolarizing factor-mediated relaxation in small mesenteric arteries of hypertensive subtotally nephrectomized rats.J Hypertens. 2006 Nov;24(11):2215-23. doi: 10.1097/01.hjh.0000249699.04113.36. J Hypertens. 2006. PMID: 17053543
-
[Angiotensin II receptor antagonist improves age-related impairment of EDHF-mediated hyperpolarization].Nihon Rinsho. 2002 Oct;60(10):1949-56. Nihon Rinsho. 2002. PMID: 12397690 Review. Japanese.
-
Adaptive changes of mesenteric arteries in pregnancy: a meta-analysis.Am J Physiol Heart Circ Physiol. 2012 Sep 15;303(6):H639-57. doi: 10.1152/ajpheart.00617.2011. Epub 2012 Jul 20. Am J Physiol Heart Circ Physiol. 2012. PMID: 22821990 Review.
Cited by
-
Testosterone plays a permissive role in angiotensin II-induced hypertension and cardiac hypertrophy in male rats.Biol Reprod. 2019 Jan 1;100(1):139-148. doi: 10.1093/biolre/ioy179. Biol Reprod. 2019. PMID: 30102356 Free PMC article.
-
Endothelium-Dependent Hyperpolarization (EDH) in Hypertension: The Role of Endothelial Ion Channels.Int J Mol Sci. 2018 Jan 21;19(1):315. doi: 10.3390/ijms19010315. Int J Mol Sci. 2018. PMID: 29361737 Free PMC article. Review.
-
The potential role of testosterone in hypertension and target organ damage in hypertensive postmenopausal women.Clin Interv Aging. 2019 Apr 29;14:743-752. doi: 10.2147/CIA.S195498. eCollection 2019. Clin Interv Aging. 2019. PMID: 31118595 Free PMC article.
-
Animal Models to Understand the Etiology and Pathophysiology of Polycystic Ovary Syndrome.Endocr Rev. 2020 Jul 1;41(4):bnaa010. doi: 10.1210/endrev/bnaa010. Endocr Rev. 2020. PMID: 32310267 Free PMC article. Review.
-
Prenatal Testosterone Exposure Decreases Aldosterone Production but Maintains Normal Plasma Volume and Increases Blood Pressure in Adult Female Rats.Biol Reprod. 2016 Aug;95(2):42. doi: 10.1095/biolreprod.116.141705. Epub 2016 Jul 6. Biol Reprod. 2016. PMID: 27385784 Free PMC article.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

