Use of an Intravascular Fluorescent Continuous Glucose Sensor in ICU Patients
- PMID: 25972280
- PMCID: PMC4525661
- DOI: 10.1177/1932296815585872
Use of an Intravascular Fluorescent Continuous Glucose Sensor in ICU Patients
Abstract
Background: Hyperglycemia and hypoglycemia are associated with adverse clinical outcomes in intensive care patients. In product development studies at 4 ICUs, the safety and performance of an intravascular continuous glucose monitoring (IV-CGM) system was evaluated in 70 postsurgical patients.
Methods: The GluCath System (GluMetrics, Inc) used a quenched chemical fluorescence mechanism to optically measure blood glucose when deployed via a radial artery catheter or directly into a peripheral vein. Periodic ultrasound assessed blood flow and thrombus formation. Patient glucose levels were managed according to the standard of care and existing protocols at each site. Reference blood samples were acquired hourly and compared against prospectively calibrated sensor results.
Results: In all, 63 arterial sensors and 9 venous sensors were deployed in 70 patients. Arterial sensors did not interfere with invasive blood pressure monitoring, sampling or other aspects of patient care. A majority of venous sensors (66%) exhibited thrombus on ultrasound. In all, 89.4% (1383/1547) of arterial and 72.2% (182/252) of venous measurements met ISO15197:2003 criteria (within 20%), and 72.7% (1124/1547) of arterial and 56.3% (142/252) of venous measurements met CLSI POCT 12-A3 criteria (within 12.5%). The aggregate mean absolute relative difference (MARD) between the sensors and the reference was 9.6% for arterial and 14.2% for venous sensors.
Conclusions: The GluCath System exhibited acceptable accuracy when deployed in a radial artery for up to 48 hours in ICU patients after elective cardiac surgery. Accuracy of venous deployment was substantially lower with significant rates of intravascular thrombus observed using ultrasound.
Keywords: continuous glucose monitoring; hospital; intensive care; intravascular.
© 2015 Diabetes Technology Society.
Conflict of interest statement
Figures

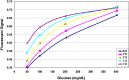









References
-
- Lazar HL, McDonnell M, Chipkin SR, et al. The Society of Thoracic Surgeons practice guideline series: blood glucose management during adult cardiac surgery. Ann Thorac Surg. 2009;87(2):663-669. - PubMed
-
- Jacobi J, Bircher N, Krinsley J, et al. Guidelines for the use of an insulin infusion for the management of hyperglycemia in critically ill patients. Crit Care Med. 2012;40(12):3251-3276. - PubMed
-
- Finfer S, Liu B, Chittock DR, et al. Hypoglycemia and risk of death in critically ill patients. N Engl J Med. 2012;367(12):1108-1118. - PubMed
-
- Hermanides J, Bosman RJ, Vriesendorp TM, et al. Hypoglycemia is associated with intensive care unit mortality. Crit Care Med. 2010;38(6):1430-1434. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

