Long-term oncologic outcomes of laparoscopic vs open surgery for stages II and III rectal cancer: A retrospective cohort study
- PMID: 25987773
- PMCID: PMC4427672
- DOI: 10.3748/wjg.v21.i18.5505
Long-term oncologic outcomes of laparoscopic vs open surgery for stages II and III rectal cancer: A retrospective cohort study
Abstract
Aim: To evaluate the 5-year survival after laparoscopic surgery vs open surgery for stages II and III rectal cancer.
Methods: This study enrolled 406 consecutive patients who underwent curative resection for stages II and III rectal cancer between January 2000 and December 2009 [laparoscopic rectal resection (LRR), n = 152; open rectal resection (ORR), n = 254]. Clinical characteristics, operative outcomes, pathological outcomes, postoperative recovery, and 5-year survival outcomes were compared between the two groups.
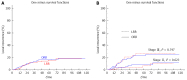
Results: Most of the clinical characteristics were similar except age (59 years vs 55 years, P = 0.033) between the LRR group and ORR group. The proportion of anterior resection was higher in the LRR group than that in the ORR group (81.6% vs 66.1%, P = 0.001). The LRR group had less estimated blood loss (50 mL vs 200 mL, P < 0.001) and a lower rate of blood transfusion (4.6% vs 11.8%, P = 0.019) compared to the ORR group. The pathological outcomes of the two groups were comparable. The LRR group was associated with faster recovery of bowel function (2.8 d vs 3.7 d, P < 0.001) and shorter postoperative hospital stay (11.7 d vs 13.7 d, P < 0.001). The median follow-up time was 63 mo in the LRR group and 65 mo in the ORR group. As for the survival outcomes, the 5-year local recurrence rate (16.0% vs 16.4%, P = 0.753), 5-year disease-free survival (DFS) rate (63.0% vs 63.1%, P = 0.589), and 5-year overall survival (OS) rate (68.1% vs 63.5%, P = 0.682) were comparable between the LRR group and the ORR group. Stage by stage, there were also no statistical differences between the LRR group and the ORR group in terms of the 5-year local recurrence rate (stage II: 6.3% vs 8.7%, P = 0.623; stage III: 26.4% vs 23.2%, P = 0.747), 5-year DFS rate (stage II: 77.5% vs 77.6%, P = 0.462; stage III: 46.5% vs 50.9%, P = 0.738), and 5-year OS rate (stage II: 81.4% vs 74.3%, P = 0.242; stage III: 53.9% vs 54.1%, P = 0.459).
Conclusion: LRR for stages II and III rectal cancer can yield comparable long-term survival while achieving short-term benefits compared to open surgery.
Keywords: Laparoscopic surgery; Locally advanced rectal cancer; Oncologic outcomes.
Figures


References
-
- Monson JR, Weiser MR, Buie WD, Chang GJ, Rafferty JF, Buie WD, Rafferty J. Practice parameters for the management of rectal cancer (revised) Dis Colon Rectum. 2013;56:535–550. - PubMed
-
- Lee SD, Park SC, Park JW, Kim DY, Choi HS, Oh JH. Laparoscopic versus open surgery for stage I rectal cancer: long-term oncologic outcomes. World J Surg. 2013;37:646–651. - PubMed
-
- Jayne DG, Thorpe HC, Copeland J, Quirke P, Brown JM, Guillou PJ. Five-year follow-up of the Medical Research Council CLASICC trial of laparoscopically assisted versus open surgery for colorectal cancer. Br J Surg. 2010;97:1638–1645. - PubMed
-
- Leung KL, Kwok SP, Lam SC, Lee JF, Yiu RY, Ng SS, Lai PB, Lau WY. Laparoscopic resection of rectosigmoid carcinoma: prospective randomised trial. Lancet. 2004;363:1187–1192. - PubMed
-
- Lujan J, Valero G, Hernandez Q, Sanchez A, Frutos MD, Parrilla P. Randomized clinical trial comparing laparoscopic and open surgery in patients with rectal cancer. Br J Surg. 2009;96:982–989. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

