Liver transplantation: history, outcomes and perspectives
- PMID: 25993082
- PMCID: PMC4977591
- DOI: 10.1590/S1679-45082015RW3164
Liver transplantation: history, outcomes and perspectives
Abstract
In 1958 Francis Moore described the orthotopic liver transplantation technique in dogs. In 1963, Starzl et al. performed the first liver transplantation. In the first five liver transplantations no patient survived more than 23 days. In 1967, stimulated by Calne who used antilymphocytic serum, Starzl began a successful series of liver transplantation. Until 1977, 200 liver transplantations were performed in the world. In that period, technical problems were overcome. Roy Calne, in 1979, used the first time cyclosporine in two patients who had undergone liver transplantation. In 1989, Starzl et al. reported a series of 1,179 consecutives patients who underwent liver transplantation and reported a survival rate between one and five years of 73% and 64%, respectively. Finally, in 1990, Starzl et al. reported successful use of tacrolimus in patents undergoing liver transplantation and who had rejection despite receiving conventional immunosuppressive treatment. Liver Transplantation Program was initiated at Hospital Israelita Albert Einstein in 1990 and so far over 1,400 transplants have been done. In 2013, 102 deceased donors liver transplantations were performed. The main indications for transplantation were hepatocellular carcinoma (38%), hepatitis C virus (33.3%) and alcohol liver cirrhosis (19.6%). Of these, 36% of patients who underwent transplantation showed biological MELD score > 30. Patient and graft survival in the first year was, 82.4% and 74.8%, respectively. A major challenge in liver transplantation field is the insufficient number of donors compared with the growing demand of transplant candidates. Thus, we emphasize that appropriated donor/receptor selection, allocation and organ preservation topics should contribute to improve the number and outcomes in liver transplantation.
Em 1958, Francis Moore descreveu a técnica do transplante de fígado em cães. Em 1963, Starzl e sua equipe realizaram o primeiro transplante de fígado. Nos primeiros cinco transplante de fígado, nenhum paciente sobreviveu mais que 23 dias. Até 1977, aproximadamente 200 transplante de fígado tinham sido realizados no mundo. Neste período, foi estabelecida a solução de problemas técnicos do transplante de fígado. Calne, em 1979, utilizou, pela primeira vez, a ciclosporina em dois pacientes submetidos ao transplante de fígado. Starzl e seus colaboradores relataram, já em 1989, que a sobrevida de 1.179 pacientes submetidos ao transplante de fígado em 1 e 5 anos foi, respectivamente, de 73 e 64%. Finalmente, em 1990, Starzl relatou o primeiro uso do novo imunossupressor tacrolimo em pacientes de transplante de fígado que apresentavam rejeição mesmo com o tratamento imunossupressor convencional. O transplante de fígado iniciou-se no Hospital Israelita Albert Einstein em 1990 e já foram realizados mais de 1.400 transplantes. Em 2013, foram realizados 102 transplantes de fígado de doadores falecidos. As principais indicações para o transplante foram carcinoma hepatocelular (38%), cirrose hepática secundária ao vírus C (33,3%) e cirrose alcoólica (19,6%). Destes, 36% dos transplantes apresentavam MELD biológico superior a 30. As sobrevidas do paciente e do enxerto no primeiro ano foram, respectivamente, 82,4 e 74,8%. Um dos maiores desafios da área do transplante de fígado é o número insuficiente de doadores para uma demanda crescente de candidatos ao procedimento. Dessa forma, destacamos que tópicos relacionados à seleção de doadores/receptores, alocação e preservação de órgãos devem contribuir para o aumento e a melhora dos resultados do transplante de fígado.
Figures


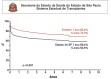

References
-
- Fox AN, Brown RS., Jr Is the patient a candidate for liver transplantation? Clin Liver Dis. 2012;16(2):435–448. Review. - PubMed
-
- Welch CS. [Liver graft] Maroc Medical. 1955;34(359):514–515. French. - PubMed
-
- Moore FD, Smith LL, Burnap TK, Dallenbach FD, Dammin GJ, Gruber UF, et al. One-stage homotransplantation of the liver following total hepatectomy in dogs. Transplantation Bulletin. 1959;6(1):103–107. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

