Cardiovascular-related healthcare resource utilization and costs in patients with hypertension switching from metoprolol to nebivolol
- PMID: 26005514
- PMCID: PMC4437480
Cardiovascular-related healthcare resource utilization and costs in patients with hypertension switching from metoprolol to nebivolol
Abstract
Background: The prevalence of hypertension is increasing in the United States and the associated costs are soaring. Despite the many treatment options, only approximately 50% of Americans with hypertension achieve optimal control. Patients receiving nebivolol, a third-generation beta-blocker, have fewer adverse events and better treatment persistence compared with patients receiving other antihypertensive agents. Little is known about the impact of switching from a second-generation beta-blocker, such as metoprolol, to nebivolol on healthcare resource utilization and costs.
Objective: To assess the impact of switching patients with hypertension from metoprolol to nebivolol on the associated healthcare resource utilization and cost.
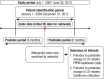
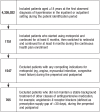
Method: This retrospective claims-based analysis included 765 adults aged ≥18 years who were diagnosed with hypertension between January 1, 2008, and December 31, 2012. Data were extracted from the HealthCore Integrated Research Database; the study was conducted between July 1, 2007, and June 30, 2013. To be included in the study, patients had to receive metoprolol for ≥6 months before switching from metoprolol to nebivolol (the preperiod), and continue to use nebivolol for an additional 6 months after switching (the postperiod). Patients with compelling indications for metoprolol but not for nebivolol were excluded from the study. The primary outcome measures were healthcare resource utilization and costs for cardiovascular (CV)-related events. The CV-related resource utilization was calculated based on 100 patients per month; the CV-related costs were calculated per patient per month (PPPM) in 2013 US dollars.
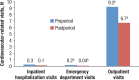
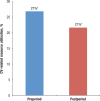
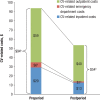
Results: A total of 765 patients were included in the analysis. Compared with the preperiod, patients switching to nebivolol had significantly fewer CV-related emergency department visits (0.2 [standard deviation (SD), 1.9] vs 0.04 [SD, 0.8], respectively; P = .012) and fewer CV-related outpatient visits (9.2 [SD, 19.9] vs 6.7 [SD, 17.5], respectively; P <.001). The numbers of inpatient visits in the preperiod and postperiod were similar (0.3 [SD, 2.4] vs 0.1 [SD, 1.5], respectively; P = .164). Patients switching to nebivolol also had significantly lower CV-related emergency department costs ($6 [SD, $78] vs $1 [SD, $27] PPPM, respectively; P = .028) and lower CV-related total medical costs ($94 [SD, $526] vs $54 [SD, $266] PPPM, respectively; P = .020).
Conclusion: This analysis of real-world data suggests that patients with hypertension who switch from the second-generation antihypertensive metoprolol to the third-generation hypertensive nebivolol have significantly lower CV-related healthcare resource utilization (eg, emergency department and outpatient visits) and lower CV-related medical costs.
Keywords: cardiovascular events; healthcare resource utilization; hypertension; metoprolol; nebivolol.
Figures
Similar articles
-
Economic impact of switching from metoprolol to nebivolol for hypertension treatment: a retrospective database analysis.J Med Econ. 2014 Oct;17(10):685-90. doi: 10.3111/13696998.2014.940421. Epub 2014 Jul 17. J Med Econ. 2014. PMID: 25007315
-
Economic benefits associated with beta blocker persistence in the treatment of hypertension: a retrospective database analysis.Curr Med Res Opin. 2015 Apr;31(4):615-22. doi: 10.1185/03007995.2015.1013624. Epub 2015 Feb 17. Curr Med Res Opin. 2015. PMID: 25651483
-
Persistence with nebivolol in the treatment of hypertension: a retrospective claims analysis.Curr Med Res Opin. 2012 Apr;28(4):591-9. doi: 10.1185/03007995.2012.668495. Epub 2012 Mar 16. Curr Med Res Opin. 2012. PMID: 22352883
-
Nebivolol: a third-generation beta-blocker for hypertension.Clin Ther. 2009 Mar;31(3):447-62. doi: 10.1016/j.clinthera.2009.03.007. Clin Ther. 2009. PMID: 19393838 Review.
-
Nebivolol for the Treatment of Essential Systemic Arterial Hypertension: A Systematic Review and Meta-Analysis.Am J Cardiovasc Drugs. 2021 Mar;21(2):165-180. doi: 10.1007/s40256-020-00422-0. Am J Cardiovasc Drugs. 2021. PMID: 32710438
References
-
- James PA, Oparil S, Carter BL, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA. 2014; 311: 507–520. Erratum in: JAMA. 2014; 311:1809. - PubMed
-
- Go AS, Mozaffarian D, Roger VL, et al; for the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics—2013 update: a report from the American Heart Association. Circulation. 2013; 127: e6–e245. Erratum in: Circulation. 2013; 127:e841. - PMC - PubMed
-
- Heidenreich PA, Trogdon JG, Khavjou OA, et al; for the American Heart Association Advocacy Coordinating Committee; Stroke Council; Council on Cardiovascular Radiology and Intervention; Council on Clinical Cardiology; Council on Epidemiology and Prevention; Council on Arteriosclerosis, Thrombosis and Vascular Biology; Council on Cardiopulmonary, Critical Care, Perioperative and Resuscitation; Council on Cardiovascular Nursing; Council on the Kidney in Cardiovascular Disease; Council on Cardiovascular Surgery and Anesthesia; Interdisciplinary Council on Quality of Care and Outcomes Research. Forecasting the future of cardiovascular disease in the United States: a policy statement from the American Heart Association. Circulation. 2011; 123: 933–944. - PubMed
-
- Sundström J, Arima H, Jackson R, et al; for the Blood Pressure Lowering Treatment Trialists' Collaboration. Effects of blood pressure reduction in mild hypertension: a systematic review and meta-analysis. Ann Intern Med. 2015; 162: 184–191. - PubMed
-
- National Center for Health Statistics. Health, United States, 2013: With Special Feature on Prescription Drugs. Hyattsville, MD: US Department of Health & Human Services; 2014. www.cdc.gov/nchs/data/hus/hus13.pdf. Accessed October 14, 2014. - PubMed
LinkOut - more resources
Full Text Sources