Apical traction: a novel visual echocardiographic parameter to predict survival in patients with pulmonary hypertension
- PMID: 26034094
- PMCID: PMC4882877
- DOI: 10.1093/ehjci/jev131
Apical traction: a novel visual echocardiographic parameter to predict survival in patients with pulmonary hypertension
Abstract
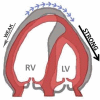
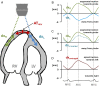
Aims: In some pulmonary hypertension (PH) patients, we noted a motion pattern where the right ventricular (RV) apex is pulled towards to left ventricle (LV) during systole, caused by traction from the LV ('apical traction', AT). Herein, we characterize patients with AT to investigate its prognostic significance.
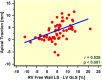
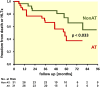
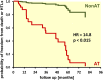
Methods and results: Echocardiograms of 62 pre-capillary PH patients (42 females, age 61 ± 15 years) were retrospectively analysed. The presence of AT was assessed visually and confirmed by speckle-tracking analysis. Fractional area change (FAC), tricuspid annular plane systolic excursion (TAPSE), RV free-wall longitudinal strain (LS) as well as LV function were measured. A primary end point of death or heart/lung transplantation was set. AT was observed in 31 patients. They had worse functional capacity, lower TAPSE (1.3 ± 0.2 vs. 1.9 ± 0.4, P ≤ 0.001) and FAC (20.3 ± 6.1 vs. 33 ± 7.1%, P ≤ 0.001), worse RV free-wall LS (-12.4 ± 3.4 vs. -20.8 ± 4.9%, P < 0.001), and higher systolic pulmonary arterial pressure (92 ± 15 vs. 75 ± 23, P < 0.001). LV function was similar in both groups. The primary end point occurred in 16 patients with and 8 without AT. AT was an independent predictor of the outcome (HR: 14.826, 95% CI: 1.696-129.642, P = 0.015).
Conclusion: AT occurs in RVs with impaired systolic function in PH patients. It may serve as a new, easily to assess visual parameter to predict the outcome in these patients. Its prognostic importance needs to be validated by prospective studies.
Keywords: apical traction; pulmonary hypertension; right ventricular function; speckle-tracking echocardiography; survival.
Published on behalf of the European Society of Cardiology. All rights reserved. © The Author 2015. For permissions please email: journals.permissions@oup.com.
Figures
References
-
- McLaughlin VV, Archer SL, Badesch DB, Barst RJ, Farber HW, Lindner JR, et al. ACCF/AHA 2009 expert consensus document on pulmonary hypertension a report of the American College of Cardiology Foundation Task Force on Expert Consensus Documents and the American Heart Association developed in collaboration with the American College of Chest Physicians; American Thoracic Society, Inc.; and the Pulmonary Hypertension Association. J Am Coll Cardiol 2009;53:1573–619. - PubMed
-
- Farber HW, Loscalzo J. Pulmonary arterial hypertension. N Engl J Med 2004;35:1655–65. - PubMed
-
- McLaughlin VV, Presberg KW, Doyle RL, Abman SH, McCrory DC, Fortin T, et al. American College of Chest Physicians.American College of Chest Physicians. Prognosis of pulmonary arterial hypertension: ACCP evidence-based clinical practice guidelines. Chest 2004;126(1 Suppl):78–92. - PubMed
-
- Humbert M, Sitbon O, Chaouat A, Bertocchi M, Habib G, Gressin V, et al. Survival in patients with idiopathic, familial, and anorexigen-associated pulmonary arterial hypertension in the modern management era. Circulation 2010;122:156–63. - PubMed
-
- Ghio S, Klersy C, Magrini G, D'Armini AM, Scelsi L, Raineri C, et al. Prognostic relevance of the echocardiographic assessment of right ventricular function in patients with idiopathic pulmonary arterial hypertension. Int J Cardiol 2010;140:272–8. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

