Meta-analysis of subtotal stomach-preserving pancreaticoduodenectomy vs pylorus preserving pancreaticoduodenectomy
- PMID: 26034372
- PMCID: PMC4445114
- DOI: 10.3748/wjg.v21.i20.6361
Meta-analysis of subtotal stomach-preserving pancreaticoduodenectomy vs pylorus preserving pancreaticoduodenectomy
Abstract
Aim: To investigate the differences in outcome following pylorus preserving pancreaticoduodenectomy (PPPD) and subtotal stomach-preserving pancreaticoduodenectomy (SSPPD).
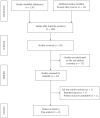
Methods: Major databases including PubMed (Medline), EMBASE and Science Citation Index Expanded and the Cochrane Central Register of Controlled Trials (CENTRAL) in The Cochrane Library were searched for comparative studies between patients with PPPD and SSPPD published between January 1978 and July 2014. Studies were selected based on specific inclusion and exclusion criteria. The primary outcome was delayed gastric emptying (DGE). Secondary outcomes included operation time, intraoperative blood loss, pancreatic fistula, postoperative hemorrhage, intraabdominal abscess, wound infection, time to starting liquid diet, time to starting solid diet, period of nasogastric intubation, reinsertion of nasogastric tube, mortality and hospital stay. The pooled odds ratios (OR) or weighted mean difference (WMD) with 95% confidence intervals (95%CI) were calculated using either a fixed-effects or random-effects model.
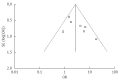
Results: Eight comparative studies recruiting 650 patients were analyzed, which include two RCTs, one non-randomized prospective and 5 retrospective trial designs. Patients undergoing SSPPD experienced significantly lower rates of DGE (OR = 2.75; 95%CI: 1.75-4.30, P < 0.00001) and a shorter period of nasogastric intubation (OR = 2.68; 95%CI: 0.77-4.58, P < 0.00001), with a tendency towards shorter time to liquid (WMD = 2.97, 95%CI: -0.46-7.83; P = 0.09) and solid diets (WMD = 3.69, 95%CI: -0.46-7.83; P = 0.08) as well as shorter inpatient stay (WMD = 3.92, 95%CI: -0.37-8.22; P = 0.07), although these latter three did not reach statistical significance. PPPD, however, was associated with less intraoperative blood loss than SSPPD [WMD = -217.70, 95%CI: -429.77-(-5.63); P = 0.04]. There were no differences in other parameters between the two approaches, including operative time (WMD = -5.30, 95%CI: -43.44-32.84; P = 0.79), pancreatic fistula (OR = 0.91; 95%CI: 0.56-1.49; P = 0.70), postoperative hemorrhage (OR = 0.51; 95%CI: 0.15-1.74; P = 0.29), intraabdominal abscess (OR = 1.05; 95%CI: 0.54-2.05; P = 0.89), wound infection (OR = 0.88; 95%CI: 0.39-1.97; P = 0.75), reinsertion of nasogastric tube (OR = 1.90; 95%CI: 0.91-3.97; P = 0.09) and mortality (OR = 0.31; 95%CI: 0.05-2.01; P = 0.22).
Conclusion: SSPPD may improve intraoperative and short-term postoperative outcomes compared to PPPD, especially DGE. However, these findings need to be further ascertained by well-designed randomized controlled trials.
Keywords: Delayed gastric emptying; Meta-analysis; Pancreatic surgery; Pancreaticoduodenectomy; Pylorus preserving Subtotal stomach preserving pancreaticoduodenectomy.
Figures


References
-
- Watson K. Carcinoma of ampulla of vater successful radical resection. Br J Surg. 1944;31:368–373.
-
- Traverso LW, Longmire WP. Preservation of the pylorus in pancreaticoduodenectomy. Surg Gynecol Obstet. 1978;146:959–962. - PubMed
-
- Lin PW, Shan YS, Lin YJ, Hung CJ. Pancreaticoduodenectomy for pancreatic head cancer: PPPD versus Whipple procedure. Hepatogastroenterology. 2005;52:1601–1604. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

