Foot deformities, function in the lower extremities, and plantar pressure in patients with diabetes at high risk to develop foot ulcers
- PMID: 26087865
- PMCID: PMC4472554
- DOI: 10.3402/dfa.v6.27593
Foot deformities, function in the lower extremities, and plantar pressure in patients with diabetes at high risk to develop foot ulcers
Abstract
Objective: Foot deformities, neuropathy, and dysfunction in the lower extremities are known risk factors that increase plantar peak pressure (PP) and, as a result, the risk of developing foot ulcers in patients with diabetes. However, knowledge about the prevalence of these factors is still limited. The aim of the present study was to describe the prevalence of risk factors observed in patients with diabetes without foot ulcers and to explore possible connections between the risk factors and high plantar pressure.
Patients and methods: Patients diagnosed with type 1 (n=27) or type 2 (n=47) diabetes (mean age 60.0±15.0 years) were included in this cross-sectional study. Assessments included the registration of foot deformities; test of gross function at the hip, knee, and ankle joints; a stratification of the risk of developing foot ulcers according to the Swedish National Diabetes Register; a walking test; and self-reported questionnaires including the SF-36 health survey. In-shoe PP was measured in seven regions of interests on the sole of the foot using F-Scan(®). An exploratory analysis of the association of risk factors with PP was performed.
Results: Neuropathy was present in 28 (38%), and 39 (53%) had callosities in the heel region. Low forefoot arch was present in 57 (77%). Gait-related parameters, such as the ability to walk on the forefoot or heel, were normal in all patients. Eighty percent had normal function at the hip and ankle joints. Gait velocity was 1.2±0.2 m/s. All patients were stratified to risk group 3. Hallux valgus and hallux rigidus were associated with an increase in the PP in the medial forefoot. A higher body mass index (BMI) was found to increase the PP at metatarsal heads 4 and 5. Pes planus was associated with a decrease in PP at metatarsal head 1. Neuropathy did not have a high association with PP.
Conclusions: This study identified several potential risk factors for the onset of diabetic foot ulcers (DFU). Hallux valgus and hallux rigidus appeared to increase the PP under the medial forefoot and a high BMI appeared to increase the PP under the lateral forefoot. There is a need to construct a simple, valid, and reliable assessment routine to detect potential risk factors for the onset of DFU.
Keywords: diabetic foot; foot anthropometrics; foot deformities; neuropathy; plantar pressure; prevention; risk factors.
Figures
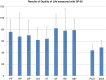

References
-
- Abbott CA, Carrington AL, Ashe H, Bath S, Every LC, Griffiths J, et al. The North-West Diabetes Foot Care Study: incidence of, and risk factors for, new diabetic foot ulceration in a community-based patient cohort. Diabet Med. 2002;19:377–84. - PubMed
-
- Frykberg RG, Lavery LA, Pham H, Harvey C, Harkless L, Veves A. Role of neuropathy and high foot pressures in diabetic foot ulceration. Diabetes Care. 1998;21:1714–9. - PubMed
-
- Veves A, Murray HJ, Young MJ, Boulton AJ. The risk of foot ulceration in diabetic patients with high foot pressure: a prospective study. Diabetologia. 1992;35:660–3. - PubMed
-
- Andersen H. Motor dysfunction in diabetes. Diabetes Metab Res Rev. 2012;28:89–92. - PubMed
-
- Ribu L, Hanestad BR, Moum T, Birkeland K, Rustoen T. A comparison of the health-related quality of life in patients with diabetic foot ulcers, with a diabetes group and a nondiabetes group from the general population. Qual Life Res. 2007;16:179–89. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous
